Profile
An Australian GP in Papua New Guinea: Part 2
In the second of a two-part profile, newsGP looks at Australian GP Dr David Mills and the challenges he faced when establishing vital primary healthcare services and training in Papua New Guinea.
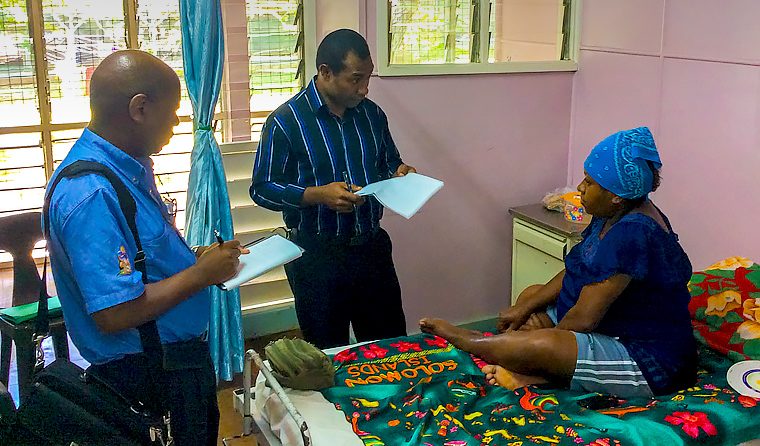 RACGP Rural Censor Dr Ken Wanguhu (left) supports the training pathway Dr Mills helped to establish by overseeing annual exams and assessments in PNG.
RACGP Rural Censor Dr Ken Wanguhu (left) supports the training pathway Dr Mills helped to establish by overseeing annual exams and assessments in PNG.
In addition to his efforts in heling to build the Kompiam Rural Hospital in Papua New Guinea’s (PNG) Enga Province, one of the most disadvantaged areas in the country, Dr Mills has made significant inroads in the area of healthcare training.
Building a pathway
Dr Mills’ contribution to primary healthcare in PNG has extended to implementing a specific pathway for general practice training, including designing the curriculum for and setting up the Masters of Medicine (MMED) (Rural) postgraduate program at the University of Papua New Guinea (UPNG).
‘It is probably the equivalent of a Fellowship of general practice in the RACGP or ACRRM [Australian College of Rural and Remote Medicine], and it’s really the only general practice training program in the country,’ he told newsGP.
Prior to the establishment of UPNG’s MMED, medical graduates tended to specialise in other areas and remain in the city of Port Moresby, leaving the more inaccessible rural and remote areas of PNG largely without doctors. What doctors there were often came from overseas and didn’t tend to stay long.
To rectify this situation, Dr Mills negotiated with the PNG government to recognise general practice as a specialty. This paved the way for the establishment of the six-year MMED program, delivered by the UPNG in partnership with the PNG Society for Rural and Remote Health and the Churches Medical Council.
Dr Mills did much of the work of establishing the program and designing the curriculum. He also connected the program with RACGP Rural’s Near Neighbours program. Through Near Neighbours, UPNG MMED trainees are provided with honorary overseas membership of the RACGP, access to journals through the John Murtagh Library, and to the gplearning online learning resource.
In addition, Near Neighbours provides exam support by sending Dr Ken Wanguhu, GP and RACGP Rural Censor, to PNG to oversee the annual UPNG MMED exams. His role involves quality assurance of the exam questions, marking, and writing a report about the process for the university.
The general practice skills taught in PNG are more focused on procedural medicine than they would be in Australia, with an emphasis on areas such as ultrasound and anaesthetics, which are necessary for all doctors in the more remote parts of the country. Assessment processes also vary.
‘Students have a real patient who has pathology; they do ultrasound on real patients. And, because the student numbers are small, we can use the same patients time and again,’ Dr Wanguhu told newsGP.
In line with Dr Mills’ hard-earned experiences as a GP in the PNG highlands, students are also tested on a range of non-medical skills.
‘For example, a GP [in PNG] must be able to be the hospital manager; they have to do good spreadsheets, because they’ve got to make a budget and then run the money,’ Dr Wanguhu said. ‘We would never test that in Australia.
‘[GPs in PNG] don’t have technicians for their fridges for their vaccines or their solar panels. They have to do the maintenance work themselves, so that’s a skill you’ve got to have.
‘Another skill they are taught is public speaking and debating. They have to go out and talk to the community, then they’ve got to go and talk to the politicians.
‘So all of those things are tested in the exam. It’s not just medical knowledge.’
Dr Wanguhu believes that the establishment of the MMED program, which took in its first entrants in 2008, has had a clear impact on the health and wellbeing of the people living in the PNG highlands and other remote areas of the country.
‘It is massive, because there were no doctors,’ he said. ‘By having doctors in those areas, things improve. Because if there’s a doctor, then there’s got to be a facility that will support the doctor, so the facilities improve. You get better outreach teams, you get more money.
‘So there are lots of measurables that we can show in PNG that have improved.’
Although helping with the exams is hard work, Dr Wanguhu feels it is well worth it in order to contribute to the development of primary care in PNG. However, he reserves his strongest praise for Dr Mills, whom he credits with making it all possible.
‘He’s the one that set it up,’ he said. ‘Yes, we support him, but he’s done an amazing amount of work and he’s an amazing human being.’
Dr Mills, of course, would never describe himself in such terms. While very modest about his achievements in PNG, he is clear about the rewards.
‘The [Kompiam] hospital is the heart of the district now and the people do hold it in very high regard,’ he said. ‘And we have a big role to play in most of the community issues. You have this amazing opportunity to play a huge role in shaping the attitudes of the next generation.
‘And then, of course, every time you can take someone out of the bush who’s in obstructive labour and deliver their baby, or just get someone out of pain, or do something that heals someone, it is a very rewarding thing.’
kompiam-hospital near-neighbours-program RACGP-rural
newsGP weekly poll
What is your chief concern with role substitution?