News
Breast density: Should it be reported?
GP Dr Sandy Minck’s experience has led her to believe screening programs should notify women of the potential cancer implications.
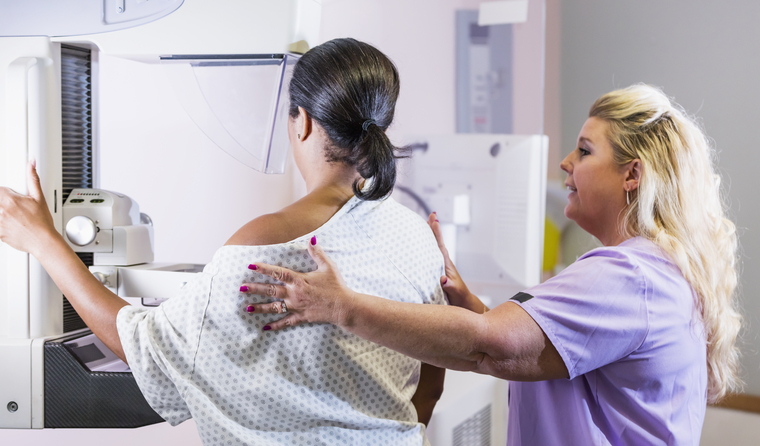 Breast density reporting is not a regular part of cancer screening programs in most parts of Australia.
Breast density reporting is not a regular part of cancer screening programs in most parts of Australia.
Dr Sandy Minck is just over six weeks post a risk-reducing mastectomy and is relieved. Had she been attending the usual BreastScreen appointments for her ‘complex, extremely dense breasts’, she says her fate may have been different.
‘The relief is real,’ Dr Minck told newsGP.
Dense breasts are both common and normal. More than half of all women under the age of 50 have dense breasts, as do about 40% of women in their 50s and about 25% of women over 60. Breast density is not related to breast size and cannot be determined by feel or touch.
However, it is associated with an approximately four-fold increased risk of breast cancer.
According to Dr Alia Kaderbhai, Chair of RACGP Specific Interests Breast Medicine, it can also complicate a cancer diagnosis.
‘It has a masking effect,’ she told newsGP.
‘That is, dense breast tissue lowers the sensitivity of mammography which can increase the chance of cancer going undetected.’
This is because, like cancer, the fibroglandular tissue appears white on a mammogram, which Dr Minck says can result in delayed diagnosis of more advanced cancers.
For this reason, Dr Minck has been attending a private breast clinic for annual mammograms and ultrasounds – a measure that may have saved her life. Last year, after microcalcification was detected, a biopsy showed atypical lobular hyperplasia (ALH).
‘A self-funded MRI showed an area suspicious of ductal carcinoma in situ [DCIS]. An excision biopsy found lobular carcinoma in situ [LCIS],’ the GP said.
‘I also self-funded a clinical geneticist consultation and testing which revealed a CHEK2 mutation. All my risk factors together resulted in a lifetime risk of 45–75%, depending on which model I used.’
But Dr Minck is concerned that for most women following the traditional screening pathways, these warning signs would not have been identified.
‘I don’t think I would have been able to achieve this if I had been attending BreastScreen,’ she said.
‘I believe I am in this position today due to my medical knowledge, contacts, and financial stability.’

Dr Sandy Minck underwent a risk-reducing mastectomy after her combined risk factors suggested a 45–75% lifetime risk of developing breast cancer. (Image: Supplied)
The current position of BreastScreen Australia on breast density and screening is to ‘not routinely record breast density or provide supplemental testing for women with dense breasts’.
One concern cited is the increased anxiety and worry about breast cancer and harms such as a high false positive biopsy rate.
‘[This is] despite significant advocacy from consumers, researchers and professional organisations for many years,’ Dr Minck said.
‘Note that BreastScreen WA have been notifying women and their GPs [about breast density] for over 10 years and BreastScreen SA is continuing to notify women at three sites after conducting a trial.
‘Many private breast clinics will also notify women, resulting in marked inequity depending on location or finances.’
Dr Kaderbhai agrees that the reporting fluctuates depending on where a patient is screened, and notes that there is variation between private and public facilities.
‘Some will report it and others won’t unless you specifically request it,’ she said. ‘[And] it varies from state to state.
‘Currently there is no legislation around reporting of breast density in Australia.’
The US Food and Drug Administration recently mandated breast density notification, while the European Society of Breast Imaging 2022 recommends ‘women should be appropriately informed about their individual breast density’.
Meanwhile, the Royal Australian and New Zealand College of Radiologists’ (RANZCR) position statement on breast density is that the addition of ultrasound to mammography increases cancer detection rates.
‘However, while additional cancers may be found, these tests may also cause harm through false positive results and none has been proven to reduce breast cancer deaths,’ the statement reads.
‘It is important to note that in women who have dense breasts but no other risk factors for breast cancer, there is no evidence that the benefits of additional imaging tests outweigh the harms.’
RANZCR’s reporting guidelines for mammography recommend breast density be listed in the mammogram report, but that this does not apply for the BreastScreen programs because a formal report is not issued.
Dr Minck says this needs to change.
‘Women do not have access to appropriate information to make informed, shared decisions about the screening that is best for them,’ she said.
‘I had no idea of the significance of breast density and was quite dumbfounded that this was a question that needed to be asked.’
However, Dr Kaderbhai says there are mixed opinions about whether guidelines regarding breast density should be introduced.
‘I believe that we do need a standardised approach around breast density reporting,’ she said.
‘It’s confusing when one state is doing one thing and another state is doing something different.
‘We definitely need some guidelines and further education for GPs, so we know what to do with this information and how to advise our patients.’
According to Australian research, most GPs know little about breast density. Dr Minck is now an advocate and hopes her story increases awareness among GPs.
‘I have managed to significantly reduce my risk of breast cancer,’ she said.
‘Unfortunately, my fellow advocate Krysty Sullivan was not so lucky.’
Ms Sullivan had a normal BreastScreen mammogram and 11 months later felt a lump which was subsequently diagnosed as triple-negative breast cancer.
She had two tumours larger than two centimetres, yet neither were seen on mammogram due to her dense breasts but were easily visible on ultrasound.
‘It is now my mission to work towards all Australians being able to access fully funded, personalised breast cancer risk assessment and management pathways,’ Dr Minck said.
‘This starts with breast density notification and education. Women need to understand the double whammy risk of dense breasts.
‘If we are serious about patient-centred care, then the future of general practice is to have patients as partners in care.’
Information about BreastScreen SA’s breast density research can be found online. BreastScreen WA’s website has more information on breast density.
Log in below to join the conversation.
breast cancer breast density mammograms screening
newsGP weekly poll
Within general practice, do you think there are barriers to providing flu vaccinations? If so, what are they?