News
Calls to lockdown aged care facilities as coronavirus spreads
More than 40 residents and staff have been diagnosed with COVID-19 in aged care facilities across Australia, highlighting the pressing need for PPE.
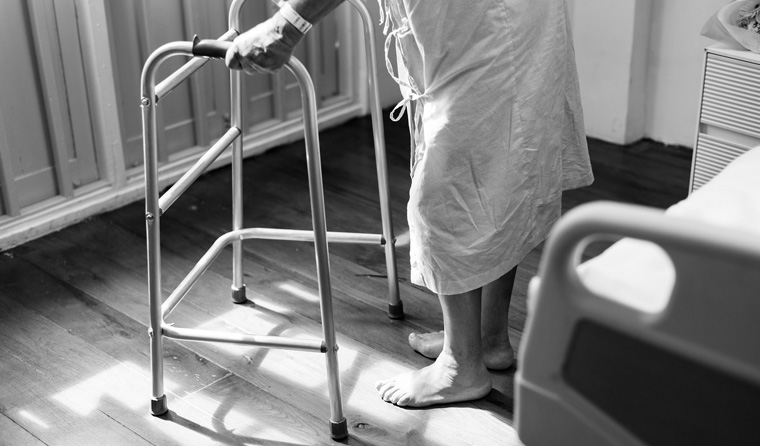 Seventeen aged care facilities across Australia have reported positive cases of coronavirus.
Seventeen aged care facilities across Australia have reported positive cases of coronavirus.
As the coronavirus spreads in aged care facilities, concerns are mounting for visiting GPs.
The Department of Health (DoH) confirmed 41 positive cases of the virus across 17 aged care facilities around Australia, including New South Wales, Queensland, Western Australia, South Australia, Tasmania and Victoria.
At BaptistCare’s Dorothy Henderson Lodge in Sydney the situation is dire, with 16 residents returning a positive test result, five of whom have died. Five staff also tested positive, as did seven close contacts.
The Aged Care Quality and Safety Commission postponed all unannounced visits to aged care facilities last week. Other site visits will continue for particular circumstances based on the level of assessed risk.
But GP and lecturer Dr Ken McCroary, who regularly sees patients in residential aged care facilities, says the numbers indicate the need to take urgent action now.
‘I’d like all facilities to be shut down to all visitors except for essential service type personnel,’ Dr McCroary told newsGP.
‘Facilities are going to need federal support in terms of providing personal protective equipment [PPE] for visiting health workers, but also the regular staff in terms of cleaners, cooking staff, etcetera. They’ll need the same support for PPE as well.’
Professor Dimity Pond, a GP with a special interest in aged care, agrees that the lack of PPE is severe and raises particular concerns for older GPs visiting facilities.
‘They are putting their health at risk and that’s a big concern,’ Professor Pond told newsGP.
Anecdotally, Professor Pond says GPs who visit aged care facilities tend to be older, making them particularly vulnerable.
‘I’m over 65 myself. We’re exactly the age group that is likely to die from COVID-19. So that’s something that weighs on people’s minds, understandably, and when you can’t protect yourself I’d have to question whether GPs would want to keep going,’ she said.
‘Once there’s been a case, I would have to really think carefully about that. Unless I get more PPE.’
In Spain, where confirmed cases have exceeded 100,000, reports have emerged of aged care patients being abandoned by health workers fearing for their own safety.
A DoH update issued to the aged care industry last week and obtained by newsGP said it was important that they be urgently advised of ‘any confirmed cases’ so these facilities can be supported with PPE. But GPs say this is too little, too late.
‘Our local PHN [primary health network] has been sending updates about the distribution of PPE that they’re getting in drip supplies from the department. But we got a box and most of the other practices I’ve spoken to are in the same situation,’ Dr McCroary said.
‘[I] had a meeting last week [and] quite a few practices have run out and they’re not getting updates from PHNs, unfortunately.’
Dr McCroary says facilities have been helpful in the transition to telehealth consultations with residents, but adds that it is not an ideal situation for the nurses who are ‘running around without PPE carrying around the phone from one room to the next’.
Dr McCroary says some of the stories he is hearing from people on the ground raise concerns as to whether basic health and safety standards are being kept.
If the virus spreads to more aged care facilities, Professor Pond believes there will need to be a ’radical rethink’ of how to approach the situation.
‘I do think that those [aged care facilities] deserve PPE, those staff should not be being exposed to COVID-19 without PPE, and even if the GPs can’t have it for their own practice and their own patients, they should not be going into those facilities without proper PPE,’ she said.
‘We don’t need to lose GPs – we don’t have enough as it is.’
The RACGP has more information on coronavirus available on its website.
Log in below to join the conversation.
aged care coronavirus COVID-19
newsGP weekly poll
Are you interested in prescribing ADHD medication?