News
COVID-19 linked to higher shingles risk for over 50s
Unvaccinated people over 50 who have had COVID-19 may be more at risk of developing shingles, a recent study has indicated.
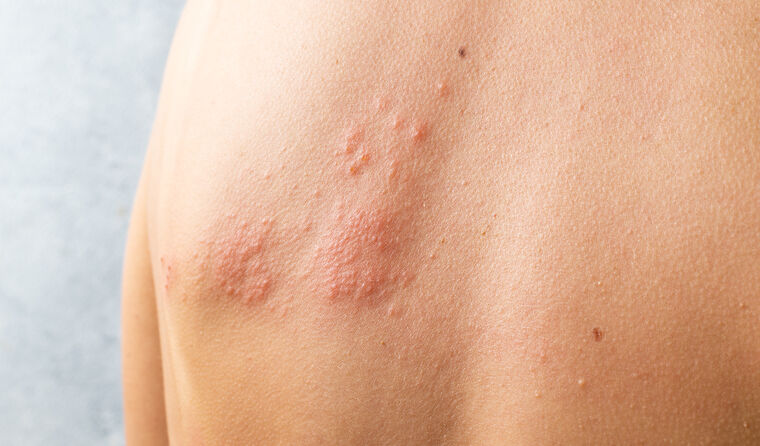 The study found the likelihood of shingles was greater among those who had COVID -19.
The study found the likelihood of shingles was greater among those who had COVID -19.
The research, which has been published in the Open Forum Infectious Diseases journal, was a retrospective cohort study designed to measure the risk of developing shingles – otherwise known as herpes zoster – following a COVID-19 diagnosis.
The EPI-ZOSTER-090 study used anonymised data from two US medical databases, most of which was gathered before the main phases of the vaccine rollout.
It compared 394,677 individuals over the age of 50 who had contracted COVID-19 with the results of 1,577,346 people who up until that point had not had the virus. All those in the study had not been vaccinated.
It found that COVID-19 diagnosis in those aged over 50 is linked to a ‘significantly increased’ risk of developing shingles.
Overall, those diagnosed with COVID-19 had a 15% higher risk of shingles than those without COVID-19, a trend that grew to 21% if they had been hospitalised with COVID-19.
The study suggests the extra risk fades after about six months.
The authors indicate that T-cell immune dysfunction caused by COVID-19 could prompt latent varicella zoster virus to reactivate, but say further research is needed to establish that.
They also write that health professionals should consider prior COVID-19 infection as a risk factor for shingles.
Professor Robert Booy, a vaccine expert at the University of Sydney, describes the research as ‘well done’, saying the results are ‘biologically plausible [and] the conclusions sensible’.
‘It’s a large study and therefore it provides reliability about the estimates,’ he told newsGP.
However, he said the danger posed by shingles in the age group is limited.
‘The risk of [shingles] is relatively low. An extra 15% adds a small amount to what is already a small amount,’ he said.
‘You can’t take COVID-19 infection as a big risk factor for getting [herpes] zoster, you can take it as causing a perturbation of a relatively small nature in the risk.’
The study was supported by GlaxoSmithKline Biologicals SA, part of the GSK group, which last year released a new shingles vaccine for those aged 50 and older in Australia.
Professor Booy said that while the study is useful, and he believes shingles vaccination at that age could be worthwhile, it may not be for everybody.
‘It’s of some relevance but it’s not compelling evidence to rush out and give everyone over 50 who’s had COVID a Zoster jab,’ he said.
‘Personally, I’m in favour of [herpes zoster] vaccination even for people in their 50s who have to pay for it but it’s not a cheap vaccine.
‘The risk is relatively low for a severe outcome in your 50s.’
For Professor Booy, there are other more pressing vaccination priorities.
‘The focus right now has to be on getting those annual flu jabs, and those third and fourth COVID jabs into people’s arms,’ he said.
Vaccination against shingles using the Zostavax vaccine is currently free under the National Immunisation Program (NIP) for people aged over 70.
A five-year catch-up program for people aged 71–79 was due to expire last year but has now been extended until the end of October 2023.
Log in below to join the conversation.
herpes zoster shingles vaccination
newsGP weekly poll
Health practitioners found guilty of sexual misconduct will soon have the finding permanently recorded on their public register record. Do you support this change?