Feature
COVID trade-offs: How to keep testing rates high
With low case numbers and coronavirus fatigue setting in, is it time to make testing more palatable and favour quantity as much as quality?
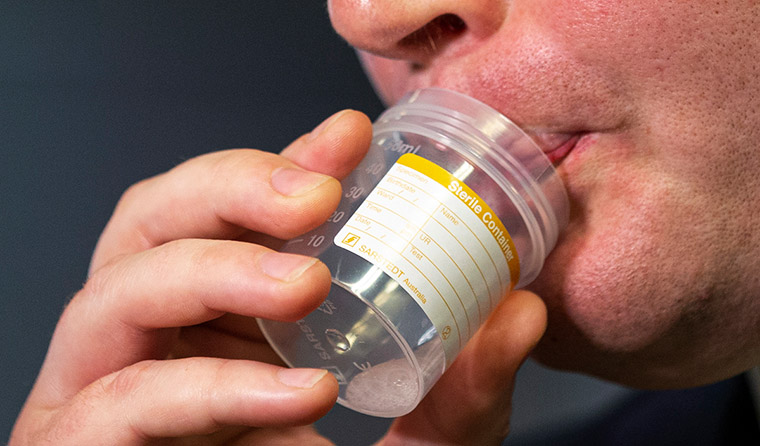 Saliva tests are being used to test some high risk workers in Victoria.
Saliva tests are being used to test some high risk workers in Victoria.
Nearly 10 months since coronavirus first arrived on Australian shores, and with many states recording ‘doughnut days’ of zero cases, there are fears coronavirus complacency could soon creep in across the country
Already, only around 50% of people with flu-like symptoms are following recommendations to get a test, while significant numbers of people are failing to self-isolate when sick or social distance appropriately.
Australia’s seven-day testing average has almost halved from its peak of just under 80,000 daily tests in August, to slightly more than 40,000 over the past week.
Signs of complacency – lack of distancing, not wearing a mask – have also prompted Victorian Premier Daniel Andrews to issue a warning that such behaviour risks triggering further outbreaks, even as the state recorded five days without a positive test (as of publication on Wednesday 4 November).
‘We just don’t want to see any more scenes of people too close together and people not wearing their masks,’ he said. ‘Make good choices for safety. It’s still lurking there, it’s still smouldering.
‘It is fragile and it will not last if every Victorian doesn’t play their part.’
The lack of symptomatic people coming forward for testing has prompted general practice researcher Professor Paul Glasziou to consider whether associated protocols around quarantine and self-isolation could be relaxed in an effort to make the entire process less onerous.
‘There are residual questions about the support for people in quarantine and making that clear to people,’ Professor Glasziou told newsGP.
‘We could maybe even shorten the duration of quarantine to make people more prepared to report to get tested, and to report close contacts as well.
‘Two weeks is a very long time.’
Similar issues have been reported in Europe – where some people in Germany, Belgium and Croatia have been unwilling to participate in testing or provide details on close contacts due to the fear of being quarantined – and countries such as the Netherlands and Norway only require 10-day quarantine periods.
But Professor Glasziou describes any move to reduce quarantine duration as a ‘trade-off’.
‘We know that there’s a long tail and that some people won’t become positive until after two weeks,’ he said. ‘But our bigger problem actually has been getting everybody tested and getting all the contacts done.
‘This is a question that really needs better research, but if you tell people they could come out of quarantine after a week – if they test negative – then they may be more willing to get tested and more willing to report close contacts as well.’
Deakin University Epidemiology Chair Professor Catherine Bennett told newsGP case isolation depends on the time that has already passed when people are tested, as well as the duration of symptoms, but that maintaining isolation until 72 hours after symptoms is a ‘safe strategy’.
‘Close contacts are generally required to quarantine for 14 days, but if they’re no longer in direct contact with the case – ie not staying in same house – they can be released at day 11 if they test negative then,’ she said.
‘It is only if they don’t agree to a day 11 test that quarantine is extended to day 21.’
However, Professor Bennett said health authorities should consider wider use of other less invasive, but also potentially less accurate, methods such as the saliva tests currently being trialled in Victoria as a way of encouraging people with mild symptoms to get tested.
‘You may be slightly more likely to miss some actual cases through false negatives, but if this is being used to test people who otherwise would not be tested at all, then it is a win,’ she said.
‘Especially for children and people getting repeat tests, such as workers in high-risk settings.’
Another option involving people submitting saliva samples is ‘pooled testing’, an approach advocated by University of Sydney Professor of Decision Sciences Ben Fahimnia.
Professor Fahimnia told the ABC that Australia’s current lack of cases means it is the ideal time for authorities to adjust their approach to testing.
‘Australia has done a great job in controlling the virus, obviously, but I think the problem is to maintain this status from now on,’ Professor Fahimnia said.
‘We know this is not going to just go away all of a sudden. We have to be prepared for another surge toward the end of the year … and pool testing is definitely a cost-effective approach to do so by keeping track of the virus.’

Professor Paul Glasziou says too many people are looking for a ‘100% solution’.
Such an approach would involve a group of people, which can range from individual households to entire suburbs, providing saliva swab samples that can be taken at home and deposited in dedicated testing bins.
These samples would then be pooled together and put through a single test, similar to the way the Chinese city of Wuhan conducted mass testing following concerns of a second wave.
A negative test result sees everyone in that group deemed negative, whereas a positive sample would see each person in the group tested individually.
This approach has been used previously to screen for things like chlamydia and gonorrhoea, and on donated blood to test for hepatitis B and C, but there are concerns that the larger the pool the less accurate the results.
Grattan Institute health policy expert Dr Stephen Duckett told newsGP he is not in favour of reducing quarantine periods in an effort to encourage people to come forward due to concerns regarding missing cases and confusing public messaging, but did say a shift in communication is needed.
‘The chance of having COVID after 14 days is trivially small, but the chance of having it after, say, eight days is around 20% – so the risk is quite high,’ he said.
‘[But] as we continue to have zero days, I think people will say, “The chance of me having COVID is very low, so I’m not getting tested even if I’ve got these symptoms”.
‘The issue is, when does the messaging change … from the messaging we’ve had during the second wave, to the messaging we need to avoid a third wave, which are slightly different situations.’
Dr Duckett says health authorities have to be clearer about the different risks people now face, as opposed to six weeks ago in Melbourne when there was wider community transmission.
‘You might need to change the rules a bit to say, “If you’ve got three of these or two of these symptoms, this is when you must come forward”,’ he said.
‘[Under that plan] you could still come forward if you’ve only got one, but we really want to get on top of this … that’s the sort of thing we need to be turning our minds to about this continuing vigilance issue and preventing the third wave.’
Professor Glasziou says the key is compromise.
‘One of the problems in general is people are looking for a 100% solution and not looking at the trade-offs that are there,’ he said.
‘What we need is a series of 90% solutions, but layers of those that pick up things. That will get us closer to the 99.9% coverage that we want.’
Log in below to join the conversation.
coronavirus COVID-19 quarantine self-isolation testing
newsGP weekly poll
How supportive are you of private health insurers funding additional general practice services that are not currently covered by Medicare?