News
Dire consequences of racism on kidney disease outcomes
Urgent action is needed to confront the ‘immense’ health disparities experienced by Aboriginal and Torres Strait Islander people.
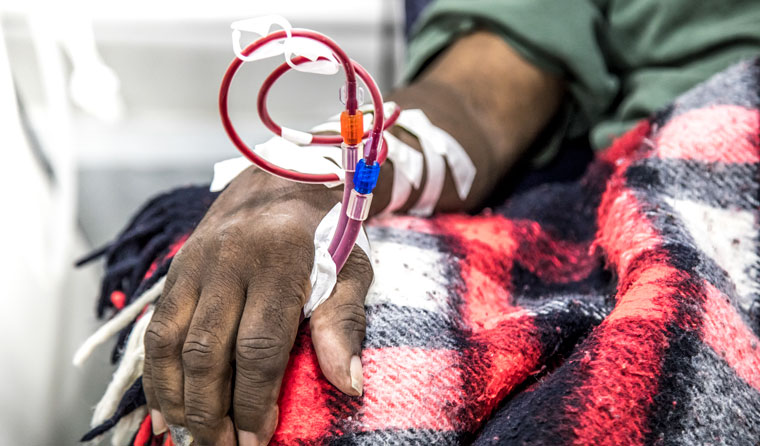 Aboriginal and Torres Strait Islander people have at least six times – in some age groups up to 15 times – the incidence of end-stage kidney disease as non-Indigenous Australians.
Aboriginal and Torres Strait Islander people have at least six times – in some age groups up to 15 times – the incidence of end-stage kidney disease as non-Indigenous Australians.
Experts have put out a call to action for states and territories to ameliorate institutional racism – including unintentional – against Aboriginal and Torres Strait Islander people.
‘Action is urgently needed to confront the immense health disparities in kidney disease outcomes suffered by Aboriginal and Torres Strait Islander peoples,’ Dr Chris Bourke, Director of Australian Healthcare and Hospitals Association (AHHA) Strategic Programs, said.
‘We believe that many of the answers to solving this problem lie in addressing racism – mostly unintentional – particularly at the institutional level, but also at the individual level.’
This is the strong message being delivered to the health sector by Dr Bourke, co-author of the perspectives brief Addressing racism to improve healthcare outcomes for Aboriginal and Torres Strait Islander people: A case study in kidney care.
Published by the AHHA’s Deeble Institute for Health Policy Research, the data is concerning.
Aboriginal and Torres Strait Islander people have at least six times – in some age groups up to 15 times – the incidence of end-stage kidney disease as non-Indigenous Australians.
Yet just a quarter have the chance to receive home-based dialysis. Only a third have the chance to receive a kidney transplant, and that drops to one-tenth if living in very remote areas.
‘We know that Aboriginal and Torres Strait Islander people have a strong preference for treatment at home. If you’re on dialysis 2–4 times a week the capacity to access in a remote community is very, very low,’ Dr Bourke told newsGP.
‘It effectively means that you can’t go back home [and] the impact on communities is profound.
‘These are people who may be of particular importance both culturally and socially within their communities and effectively can never go back. That’s terrible.’
It has long been known that Aboriginal and Torres Strait Islander people do not have equitable outcomes in terms of chronic disease, including end-stage kidney disease.
Since 2017, Queensland Health has implemented a number of strategies to address institutional racism in its health system, and South Australia has taken note. But Dr Bourke says ‘much more is needed’ and other states need to urgently look at reforming their own systems.
Together with his fellow authors, Dr Bourke suggests concerted action in required across four interconnected areas:
- Cultural safety – boards, accreditation agencies, and education and training providers can do more to promote self-reflection in non-Indigenous healthcare professionals about providing accessible and responsive care that is safe and free of racism, as judged by Aboriginal and Torres Strait Islander individuals, families and communities
- Institutional racism – healthcare organisations can actively work within the health system to reverse the exclusion of Aboriginal and Torres Strait Islander people from governance, control, and accountability of healthcare organisations, and to employ more Aboriginal and Torres Strait Islander health workers
- National safety and quality health service standards – the Australian Commission on Safety and Quality in Healthcare’s triennial accreditation processes for hospitals set out how healthcare organisations can improve service delivery to Aboriginal and Torres Strait Islander people
- Race discrimination law – existing laws tend to focus on individual rather than systemic discrimination, with racism being hard to prove, even though intention to discriminate does not have to be proven. The laws also focus on equality of opportunity rather than equality of outcomes. Nevertheless, it is important for healthcare organisations to ensure that the need to avoid discrimination is factored into their governance and operations and to be aware that the laws do provide for ‘positive discrimination’ in removing barriers to care and bringing about better outcomes
Looking to the future, Dr Bourke says it important that Aboriginal and Torres Strait Islander people are continually contributing to the dialogue, so policies ensure access to equitable care.
‘What sort of outcomes would you expect for a hospital for women, which was staffed by men, governed by men, held accountable by men, didn’t employee any women at all? It’d be terrible,’ Dr Bourke said.
‘So why would we expect good outcomes from healthcare organisations that don’t have any Aboriginal and Torres Strait islander people working in them?
‘There is documented evidence of Aboriginal and Torres Strait Islander peoples receiving poorer healthcare outcomes when treated by non-Indigenous healthcare organisations and health professionals.’
As Australia’s first Aboriginal dentist, Dr Bourke has had 40 years’ experience in the healthcare setting and understands the importance of cultural awareness.
‘Primary care is incredibly important not just for preventing disease but also helping people to live healthy and productive lives with disease,’ he said.
‘Health practitioners need to recognise their own culture and views and how that can be a barrier to providing equitable care to people from other cultures, and understand that the way you view the world is not the way other people view the world.’
While the changes required to achieve better kidney care outcomes are complex, Dr Bourke believes it is important that all healthcare workers remember their potential to have a positive influence.
‘[I want] to reemphasise the calls to action that we had in our paper,’ he said.
‘We all have the capacity to ask questions of organisations. Some of us are actually in the position to be part of the governance of organisations within the boards and committees. So there’s the opportunity to say “Well, what are we doing about this?”
‘So instead of looking at others, we need to look at home too.’
The RACGP has a range of materials to support GPs and practice teams to deliver culturally safe healthcare.
Log in below to join the conversation.
Aboriginal and Torres Strait Islanders kidney disease racism
newsGP weekly poll
How often do patients ask you about weight-loss medications such as semaglutide or tirzepatide?