News
Ear disease in Aboriginal and Torres Strait Islander children
Updated guidelines on managing otitis media aim to address what has been called a ‘public health emergency’.
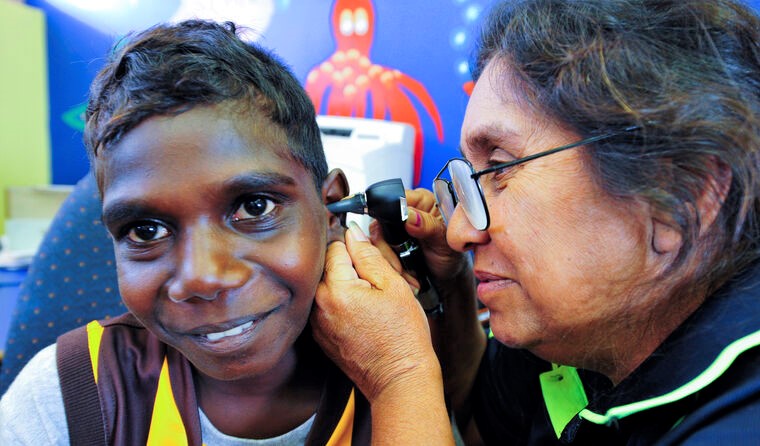 Only one in 10 Aboriginal and Torres Strait Islander children under the age of three in remote NT communities has healthy ears. (Menzies School of Health Research)
Only one in 10 Aboriginal and Torres Strait Islander children under the age of three in remote NT communities has healthy ears. (Menzies School of Health Research)
In remote communities across the Northern Territory (NT), only one in 10 Aboriginal children younger than three years have healthy ears, a new report in the Medical Journal of Australia (MJA) has found.
Five have otitis media (OM) with effusion (OME) or ‘glue ear’, and four have suppurative OM – acute OM (AOM) with or without perforation, or chronic suppurative OM (CSOM)
‘The level of ear disease in Aboriginal [and Torres Strait Islander] children is defined by the World Health Organization [WHO] as meeting a public health emergency,’ the study’s lead author Professor Amanda Leach told newsGP.
According to Professor Leach, leader of the Ear Health Research Program at the Child Health Division of Menzies School of Health Research, any rate of OM above 4% is considered a public health emergency. The rate of chronic suppurative OM in Aboriginal and Torres Strait Islander children in the NT currently sits between 12–15%.
‘We started off here with around 24%, so it’s definitely come down,’ she said. ‘But we’re a long way away from that target.’
The new paper includes the 2020 update to clinical guidelines for the management of OM in Aboriginal and Torres Strait Islander populations, which for the first time feature the Grading of Recommendations, Assessment, Development and Evaluation (GRADE) approach.
Changes in management as a result of the guidelines include:
- targeted recommendations for both high- and low-risk children
- strongly recommending antibiotics for persistent OME in high-risk children
- strongly recommending azithromycin for AOM where adherence is difficult or there is no access to refrigeration
- recommending concurrent audiology and surgical referrals where delays are likely
- recommending surgical referral for CSOM at the time of diagnosis.
A new digital app,
OMapp, has also been designed to aid clinicians when assessing ears and is available through the
MJA paper.
Professor Leach hopes these resources will help clinicians manage a range of ear conditions.
‘We want to eradicate the serious end of the disease and the disabling hearing loss that causes,’ she said.
‘But we don’t want to let go of the fact that once you’ve gotten rid of the perforated eardrum you’re still left with this glue ear, which also is associated with disabling hearing loss in a number of children.’
Another key message Professor Leach would like to impart is the importance of initial assessment of Aboriginal and Torres Strait Islander children’s ears.
‘Particularly if you’ve got a high-risk Aboriginal child, look at the ears,’ she said.
‘Our mantra here is: “Every ear, of every child, at every opportunity”.
‘Do an ear assessment and learn, if you can, pneumatic otoscopy so you can test if there is fluid behind the eardrum, rather than just looking at it.’
If pneumatic otoscopy cannot be used, Professor Leach recommends using tympanometry with normal otoscopy.
Aside from the potential immediate clinical benefits associated with checking ears, it may also help improve the overall long-term health prospects for Aboriginal and Torres Strait Islander children.
Associate Professor Peter O’Mara, Chair of RACGP Aboriginal and Torres Strait Islander Health,
previously told newsGP that
poor health outcomes are linked to trauma associated with systemic and institutionalised racism in Australia, of which interaction with police and the criminal justice system is one of the major sources.
‘Aboriginal and Torres Strait Islander people are more likely to suffer hearing disorders … and the evidence is there to say that when you have a hearing disorder,
you’re more likely to be incarcerated,’ he said.
‘Some of the things that we do as GPs, like working on trying to improve ear health for children, and particularly for Aboriginal children, can have a direct impact.’
 When it comes to assessing Aboriginal and Torres Strait Islander children, Professor Amanda Leach has a mantra: ‘Every ear, of every child, at every opportunity’.
When it comes to assessing Aboriginal and Torres Strait Islander children, Professor Amanda Leach has a mantra: ‘Every ear, of every child, at every opportunity’.
It also is particularly important to check the ears of Aboriginal and Torres Strait Islander children regularly as OM is often asymptomatic in this cohort; Professor Leach says that an Aboriginal and Torres Strait Islander child may present to the GP with ‘bulging eardrums’ but may not be febrile or in pain.
‘That’s an extraordinary thing,’ she said.
‘There needs to be a follow-up schedule, a recall or some system in your practice whereby those families are rung to see if the child is improving.
‘But it is really important to have another look at that ear and check that the bulging has resolved.’
Professor Leach says that children who do not have a bulging eardrum but have an immobile middle ear effusion or glue ear also require regular follow-up.
Furthermore, a child with a persistent glue ear needs to be referred for a hearing assessment and to an ear, nose and throat (ENT) specialist to see if they meet the criteria for either a hearing aid or to have grommets inserted.
‘If a parent is at all concerned about language development or behaviour perhaps related to not hearing properly, they should also be advised about the benefit of having a hearing assessment,’ she said.
While Professor Leach’s work has focused on Aboriginal and Torres Strait Islander children in the NT, there have been similar rates of ear disease in Aboriginal and Torres Strait Islander children in Queensland.
Queensland’s Deadly Ears Program found that, of the approximately 2500 Aboriginal and Torres Strait Islander children who attended its ENT clinic service from 2015–19, three in five had an ear condition and two in five had conductive hearing loss.
Among the 651 children and young people who attended at least two ENT clinic services between 2015 and 2019:
- 77% had at least one type of ear condition at their first service, decreasing to 59% at their latest service
- the proportion of children and young people with OME approximately halved from 35% at the first service to 16% at the latest service.
While Professor Leach is glad to see improvements in both the NT and Queensland, she says clinicians who work in rural and remote areas with Aboriginal and Torres Strait Islander children need to understand the importance of ear checks in order for the progress to continue.
‘Here in the Top End, in the NT, the workforce turnover is massive,’ she said.
‘We’re dealing with really massive health issues out here and to cope with ear disease and hearing loss, which is affecting so many children, it’s just overwhelming.
‘So we’re tying to think of strategies to rapidly upskill GPs that are new to the NT [and] how we can orientate them to these issues.’
Professor Leach says it is critical for all children – including those with ‘only’ mild or moderate hearing loss – to receive such care.
‘People say, “It’s only a mild or moderate hearing loss, it’s okay”,’ she said.
‘But the WHO has assisted us with statements saying that moderate hearing loss in a child is actually disabling hearing loss and that puts them at whole different level of urgency.’
When it comes to ear disease in children, Professor Leach says she often quotes her colleague, Australia’s first Aboriginal and Torres Strait Islander surgeon, ENT specialist
Associate Professor Kelvin Kong.
‘He says that otitis media and conductive hearing loss are generally not life-threatening,’ she said.
‘But they are life-changing.’
Log in below to join the conversation.
Aboriginal and Torres Strait Islander health ear disease otitis media
newsGP weekly poll
Which of the following areas are you more likely to discuss during a routine consultation?