News
From the UK COVID frontline: what GPs can expect from the vaccine rollout
GP Dr Colin Fitzpatrick talks to newsGP about coordinating the delivery of Pfizer/BioNTech vaccines across 110 Northern Ireland aged care facilities, and why they may not be suited to a nationwide rollout.
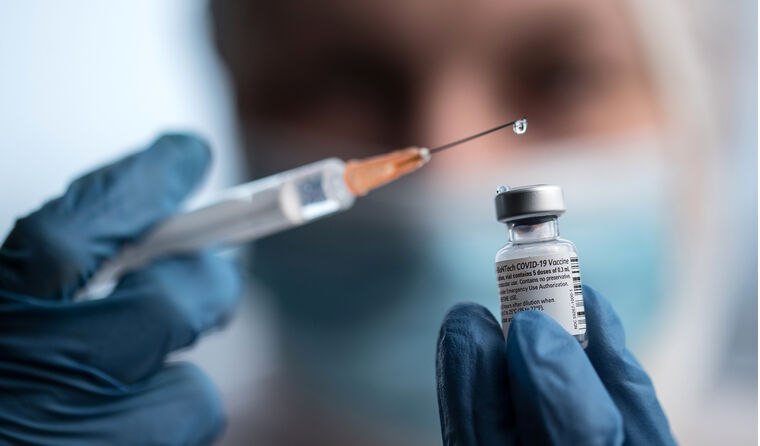 The Pfizer/BioNTech candidate is reportedly ‘phenomenally sensitive’ to movement. (Image: AAP)
The Pfizer/BioNTech candidate is reportedly ‘phenomenally sensitive’ to movement. (Image: AAP)
When Northern Ireland experienced its first wave of the coronavirus, GP Dr Colin Fitzpatrick was at the centre of the health response in aged care; a challenging and distressing time he tries not to think about too much.
‘I must say that was probably the most traumatic experience of my entire professional career – it’s not something that we’re used to seeing in general practice,’ he told newsGP.
‘In the early outbreaks I remember being in a care home where almost a third of the whole population of the nursing home died of COVID in a period of a few days.
‘The only time I’ve actually experienced that level of death is way back in the days of the Troubles in Belfast when I was working in the emergency department. That was fairly traumatic, but this was almost worse.’
Northern Ireland is currently undergoing a six-week lockdown as it moves into its third wave of the virus, having recorded 95,361 cases and 1606 deaths to date.
Its vaccination program is now well underway, with both the Pfizer/BioNTech and Oxford/AstraZeneca vaccines in circulation. As of 13 January, a total of 121,711 vaccines had been administered, of which 19,010 were second doses.
Dr Fitzpatrick, who is a senior adviser for NHS Resolution and clinical director of South Eastern Health and Social Care Trust, coordinated the rollout of the Pfizer vaccine across 110 of the country’s aged care facilities.
Starting on 14 December, it took 10 teams – each led by a GP overseeing between 4–12 nurses –
10 days to administer the first dose to anywhere between 600–800 patients a day, with the second round completed on 13 January.
‘We have worryingly had one or two patients who have had two doses of the Pfizer vaccine, and yet a week later after a second dose presented with symptoms and tested positive for COVID – that was a wee bit worrying,’ Dr Fitzpatrick said.
‘We would hope that we’ll start to see the care home outbreaks disappear in the next few weeks.’
Speaking to newsGP while undergoing mandatory quarantine in Brisbane, Dr Fitzpatrick is about to embark on a stint in Australia and hopes to give local GPs insight into his experience using the mRNA vaccine.
Beyond the logistical challenge of the vaccine’s storage requirement of –70°C, Dr Fitzpatrick says it is ‘phenomenally sensitive’ to movement.
‘They’re carried very carefully into the building to avoid shaking or dropping them … literally, if you drop a vial, it has to be discarded,’ he said.
‘[Then] before you use it, you have to dilute the vaccine with saline. So you inject 1.8 mils of saline into each vile. Once that is done, it’s really sensitive to movement.’
As a result, Dr Fitzpatrick said he and his colleagues had to go to ‘extreme lengths’ to avoid transporting the vaccine from room to room.
‘My mum, for example, is in a nursing home and she’s more or less bed bound. But we hoisted her out onto a wheelchair and wheeled her to the vaccine rather than bringing the vaccine to her because the vaccine is so sensitive,’ he said.
‘So this is really, really different to what we’re used to in doing a flu clinic in general practice.
‘Pfizer is absolutely not suitable for a mass rollout, simply because of the really difficult way you have to handle it. I’m sure they’ll find an easier way, but not in the immediate future.’
What adds to the challenge with Pfizer is that each vial contains six doses.
‘So if my patients don’t come in multiples of six I’m going to have leftover vaccine – and this is a phenomenally precious resource, so we don’t want to throw vaccine out,’ Dr Fitzpatrick said.
‘One of the trickiest things we had at the end of the day was trying to find people that we could give vaccine to.
‘The AstraZeneca one is a lot easier to handle, but it’s still not as easy as the flu vaccine because it still comes in multi-dose vials. So you’ve got to very carefully draw up a dose from a vial and then another dose, and another dose. That slows you down and introduces the potential for error.’
While Dr Fitzpatrick and his colleagues did not witness any severe adverse reactions to the Pfizer/BioNTech vaccine, such as death, he admits that allergic reactions ‘were significantly more common than I’ve ever seen in another vaccination campaign’.
‘Overall we submitted about 14 or 15 adverse drug reaction reports [out of 6000 people]. The average anaphylaxis rate for most vaccines is about 1.3 in a million,’ he said.
‘A lot of them were allergic type rashes, tachycardia, and feeling generally really unwell – sort of things you don’t normally see with flu vaccines.
‘That’s why I was pleased that I put a doctor on every team because then we had a senior medical decision maker there. I’m not saying nurses can’t handle these things themselves, but they feel more confident if there is a doctor.’

GP Dr Colin Fitzpatrick has been at the centre of Northern Ireland’s aged care response to COVID-19.
As the Federal Government awaits the Therapeutic Goods Administration’s approval for use of a COVID vaccine in Australia, reports have emerged of 29 aged care residents in Norway having died after receiving the Pfizer/BioNTech vaccine.
Dr Fitzpatrick says while he does not know the intricate details of the Norway residents or rollout, his teams took precautions with particularly high risk patients.
‘When I said we vaccinated every resident, there were a number of people we left out, and mostly because they were basically palliative and were likely to die within the next few days,’ he said.
‘So we saw no purpose in giving them the vaccine for which they would get no benefit.
‘In Norway, now I may be reading this wrong, but I think they actually vaccinated those people as well. If you vaccinate 20,000 elderly people as they did, 30 were going to die in next few days anyway. Not to sound brutal, but that’s sort of the way it is.’
The Department of Health (DoH) recently told newsGP it is currently undertaking a ‘procurement process’ to support the readiness and availability of an in-reach/surge workforce to deliver the vaccine to aged care settings, and could not provide further details about the involvement of GPs.
‘It is anticipated however, that GPs will play a key role in all aspects of the delivery of the COVID-19 Vaccination Program,’ the DoH said.
From firsthand experience, Dr Fitzpatrick says there is no doubt that ‘the residents’ GP will know them best’.
‘They have to have some input, particularly for residents who might have doubts or there may be something in their medical history because, again, this is an evolving picture,’ he said.
‘Then there are lots and lots of general vague medical queries. If somebody’s got a chest infection, are they fit to get vaccinated? I found myself examining chests and saying whether I thought somebody was fit to be vaccinated.
‘It’s much better to have a doctor about the place to assist with the tricky things that come up, particularly until you get some real experience of using the vaccine.’
What is clear is that the mass vaccination campaign Australia is set to embark on is like nothing GPs have seen before. But Dr Fitzpatrick says there is no doubt that Australia is in a much better position than most.
‘In Northern Ireland they’re more or less saying forget about general practice for a month or two, and we will do emergencies only,’ he said.
‘There is undoubtedly an excess non-COVID mortality associated with this whole thing, just because of the whole disruption it creates for the system, which is why you’re so lucky in Australia that you don’t have that.
‘But this is new, so you need to be alert and you need to be flexible because it’s going to change, and … if you’re going to vaccinate the population in the timescales that you want – which is everybody in the country vaccinated within months – it’s double the work.’
Log in below to join the conversation.
aged care AstraZeneca coronavirus COVID-19 Pfizer/BioNTech vaccinations
newsGP weekly poll
Health practitioners found guilty of sexual misconduct will soon have the finding permanently recorded on their public register record. Do you support this change?