News
GP iron infusions would save health system $124m: RACGP
The college is calling on the Government to create a new $200 MBS item to subsidise the procedure, saying it will save patients time and money.
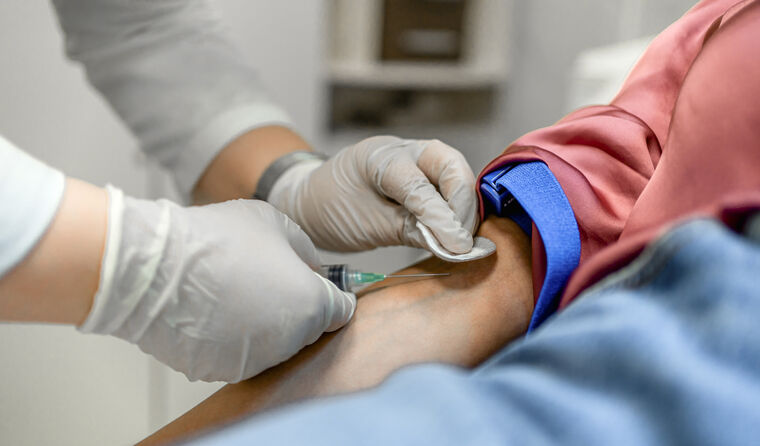 A newsGP poll found 38% of practices currently offer iron infusions.
A newsGP poll found 38% of practices currently offer iron infusions.
The creation of a new Medicare item for iron infusions would save the Commonwealth $124 million and ‘be an efficiency for our health system’, according to a new RACGP submission.
The college says advances in technology mean there is no reason the procedure cannot be performed in general practice, but currently, the out-of-pocket costs for patients remain high.
In response, it has issued a call for a new $200 Medicare Benefits Schedule (MBS) item to be introduced.
‘This solution can be implemented as soon as the MBS item is available,’ the submission said.
‘If implemented, hospitals would quickly see a reduced demand for iron infusions in outpatient clinics and emergency departments.’
The plea is part of the RACGP’s submission to the MBS Review Advisory Committee, as it works to ensure the scheme is contemporary, sustainable, evidence based, and supports universal access to high value care’.
The proposed item would specifically allow for:
- a GP to spend up to 15 minutes calculating the iron dosage, educating the patient and receiving informed consent
- the administration of the iron infusion for at least 15 minutes by a team member
- an observation period by no less than 30 minutes to monitor the patient for anaphylaxis.
The item would only be billable for patients who have been diagnosed with iron deficiency anaemia and limited to once every 12 months, with some exceptions.
Iron deficiency anaemia remains one of the most common potentially preventable hospitalisations in Australia,
accounting for 70,580 same-day admissions in 2021–22.
Historically, iron infusions have been limited to hospital settings, but the increased safety of modern formulations means they can now be safely administered in general practice.
The submission says some general practices are billing the procedure as a standard consultation item, such as items 23 or 36, but this only lowers the patient’s out-of-pocket cost by $41.40 or $80.10 respectively.
RACGP President Dr Nicole Higgins described the potential change as a ‘no-brainer’.
‘The new item should be combined with dynamic public health messaging educating patients across Australia about the causes and symptoms of iron deficiency and nutritional information about how to boost iron levels in our diet,’ she said.
‘The technology is available, but what is holding us back is the fact that there are no Medicare items subsidising iron infusions in general practice.
‘They cannot bill a longer item as nurse time cannot be included when billing these items. The monitoring time also impacts access to the consultation room for the GP to be able to see other patients, reducing overall patient load.’
A previous newsGP survey found 38% of practices currently offer iron infusions and a further 53% said they would offer them if a rebate was available.
However, the submission draws attention to the significant time and resources the infusion currently takes for already busy practices.
‘While affordability of care is a priority for general practices, they need to ensure their practice is financially viable so they can provide care into the future for their community,’ it said.
‘They take one hour to complete, comprising of 15 minutes of GP time for patient discussions and dose calculation and 45 minutes for a nurse to administer the infusion and monitor for allergic reactions.
‘During this hour, a GP could have instead treated several patients with brief 6–20-minute consultations in the same room.’
Dr Higgins said the call comes at a time of high cost of living pressures, with some patients unable to afford an iron infusion in general practice ending up on waiting lists at public hospitals or outpatient clinics.
‘Their care is delayed by months, and in the meantime their condition can significantly deteriorate, she said.
‘In addition to government savings, it would mean more patients accessing care faster and more conveniently from a GP they know and trust, furthering enhancing continuity of care.
‘The solution is right in front of us – a new Medicare item subsidising iron infusions in general practice so that more patients can get the treatment they need, when they need it.’
The MBS Review Advisory Committee currently meets four times a year to discuss submissions. Its next meeting is scheduled for 6 March.
Log in below to join the conversation.
anaemia iron deficiency MBS Medicare Medicare Benefits Schedule
newsGP weekly poll
Within general practice, do you think there are barriers to providing flu vaccinations? If so, what are they?