News
GP visits can help avoid health ‘black hole’
New research finds the average person aged 40 and over has five unidentified health problems that can be reversed with early intervention.
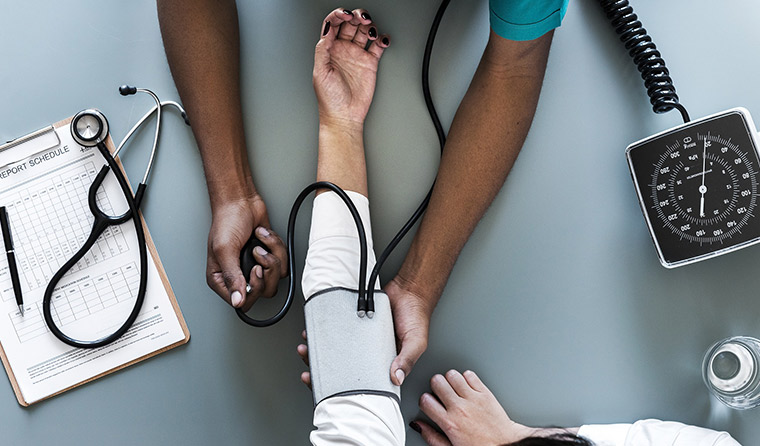 Nearly one third of the people tracked in the study had undiagnosed high blood pressure.
Nearly one third of the people tracked in the study had undiagnosed high blood pressure.
According to the Flinders University study, seeking out a health professional for regular full health screenings from around age 40 – even when feeling healthy – enables people to make changes when problems first occur.
‘People in their middle years are being sucked into the black hole of ageing,’ study lead author Professor Sue Gordon said.
‘Small reversible changes are accumulating unnoticed while people are time poor and their lives consumed by work and parenting. Often we don’t notice the problem until it’s too late for the individual to self-manage, and vastly more expensive to address.
‘So even 40 and 50 year olds have unrecognised health issues, many of which are amenable to change.’
Of the 561 adults aged 40–75 years who took part in the study, 30% had undiagnosed high blood pressure; 32% were experiencing memory and cognition problems; and 34% had undiagnosed functional hearing loss.
Study co-author and former RACGP President Professor Michael Kidd told newsGP the study adds the existing wealth of evidence supporting the value of preventive health, but that Australia still has a healthcare system skewed towards treatment.
‘Sadly it’s a perennial challenge – this is not new,’ he said.
‘We have the evidence to show preventive care interventions can make a difference, as well as the really important role that general practice can play in preventive healthcare, health promotion and early detection of serious disease to keep people as healthy as possible for as long as possible.
‘Yet … we’ve seen under-investment in preventive care and despite the best efforts of many people, not as much of a focus on prevention and health promotion.’
While conceding balancing health budgets is a massive challenge for health ministers, Professor Kidd pointed to the decline in preventive health funding from states and territories, and the Medicare freeze on general practice, as major areas for improvement.
‘It’s a really short-sighted approach to healthcare because as a population ages, as we have more people with developing chronic health conditions and especially comorbid conditions and more complex conditions, we’re going to reach a point where we can’t afford to continue to provide the healthcare that people expect,’ he said.
‘We need to be doing more now to prevent many of those conditions from developing in the first place, and to keep people as well as possible for as long as possible and away from hospitals and away from the expensive treatment that goes with that.’
Professor Gordon also called for a boost to the 1.5% of the national health budget currently spent on health promotion and prevention services.
‘Australia needs to move from an over-burdened reactive health system to proactive best health through middle and older life,’ she said.
‘Individual health screening and self-management should be a cornerstone to empower healthy ageing in Australia.’
Aside from the reducing pressure on the chronically under pressure hospital systems, Professor Kidd also said regular preventive health checks can help in the fight against ‘too much medicine’.
‘A lot of the health concerns which were revealed in the study … don’t need medication as a solution. What they need is people being given education and support about lifestyle modification, rather than tablets to effect a solution,’ he said.
‘By supporting people to eat well, to keep physically active, [and] reduce the impact of substances like tobacco and excess alcohol, as well as supporting people so that so they don’t experience great psychological distress in their lives – these are all things which happen without pharmaceutical solutions.’
funding preventive health primary care research
newsGP weekly poll
Health practitioners found guilty of sexual misconduct will soon have the finding permanently recorded on their public register record. Do you support this change?