News
Identifying eating disorders in general practice
While GPs are crucial in identifying eating disorders, patients experiencing these conditions do not always present in an obvious way.
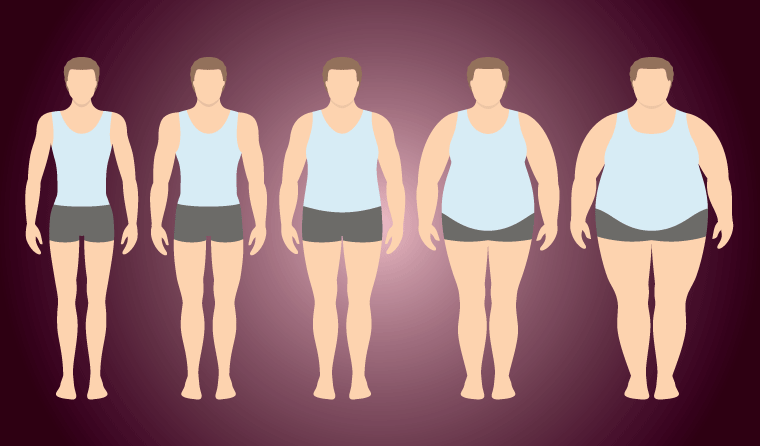 People experiencing an eating disorder are not necessarily underweight and can appear in all weight ranges.
People experiencing an eating disorder are not necessarily underweight and can appear in all weight ranges.
Even though there has been increased awareness of eating disorders and the dangers they present in recent years, some people experiencing these conditions can struggle to obtain a diagnosis due to persistent stereotypes regarding how they should look – namely, young, female and extremely underweight.
But such presentations are not reflective of all people with eating disorders and, if they remain untreated, these patients can experience very serious consequences such as osteoporosis, heart failure and death. People with an eating disorder are also up to 31 times more likely to die by suicide.
Elizabeth Rieger, Associate Professor of Psychology at the Australian National University, believes the trusted long-term relationships GPs often have with their patients can make them powerful allies in providing early intervention and treatment for eating disorders. However, these conditions can be very challenging to identify, as they are not always evident at first glance.
‘People with bulimia nervosa can be in the normal or the overweight and obese weight range, and people with binge-eating disorder are often in the obese weight range, but can also be in the normal weight range,’ she told newsGP.
‘Eating disorders are severe irrespective of the person’s weight.’
Nor can doctors necessarily rely on other ‘traditional’ characteristics.
‘Although eating disorders predominantly occur in females, binge-eating disorder is more equally distributed amongst males and females,’ Associate Professor Rieger said. ‘And though eating disorders often have their onset in late adolescence, early adulthood or even younger, they can occur throughout the lifespan.’
Because of the serious harms caused by eating disorders and the relative difficulty of reliable identification, Associate Professor Rieger believes it is helpful for practitioners to include specific screening tools in patient consults as part of general health screening.
‘These instruments are quite short. They’re often just five items, such as The Eating Disorder Screen for Primary Care [ESP] and SCOFF [Sick, Control, One stone, Fat, Food],’ she said.
Such tools can be more useful than a focus on weight because they are more likely to identify disordered psychological and eating behaviours, the key issue at the heart of these conditions.
‘Core symptoms are constant preoccupations with eating, shape and weight. The highly punishing daily routines people have to go through as a result of their eating disorder, such as strict dieting or compulsive exercising irrespective of whether they’re tired or unwell or have other important commitments,’ Associate Professor Rieger said.
‘There’s many psychological conditions that are comorbid with eating disorders, such as depression and anxiety. Body dissatisfaction is extremely high, there might be perfectionism in there. So there’s a whole range of psychopathology that makes these severe eating disorders.’
Associate Professor Rieger underlined the importance of practitioners taking a proactive stance towards eating disorders because early intervention can make all the difference.
‘Sometimes we hear stories of people presenting to hospitals and being told they’re not yet underweight enough to warrant admission,’ she said.
‘But early identification and intervention is really important in terms of people having better outcomes.’
binge-eating-disorder bulimia-nervosa eating-disorders
newsGP weekly poll
As a GP, do you use any resources or visit a healthcare professional to support your own mental health and wellbeing?