Analysis
Modern radiation therapy and keratinocyte cancer management
SPONSORED: Technological advances now allow treatment to be sculpted to large areas of skin affected by pre-cancerous lesions and invasive disease.
 Radiation therapy can be an especially good option for lesions in areas where surgery would result in significant cosmetic imperfections and, for patients unsuitable for surgery.
Radiation therapy can be an especially good option for lesions in areas where surgery would result in significant cosmetic imperfections and, for patients unsuitable for surgery.
Australia continues to have the unenviable status as the skin cancer capital of the world.
The incidence of keratinocyte cancers, basal and squamous cell carcinomas (BCCs and SCCs), has increased consistently for the past 30 years. It is now estimated that approximately 70% of Australian men and 58% of women will have at least one keratinocyte cancer excised in their lifetime, costing the economy around $1.2 billion each year.
Treatment success for keratinocyte carcinomas is very good in comparison to other cancers; however, early diagnosis and treatment is important to prevent morbidity, and in the setting of SCCs reduce the risk of metastatic spread.
Excision or Mohs continues to be the gold-standard treatment, although radiation therapy is a well-established non-invasive alternative with cure rates similar to surgery for certain presentations.
Radiation therapy can be an especially good option for lesions in areas where surgery would result in significant cosmetic imperfections, for patients unsuitable for surgery, or in the adjuvant setting for high-risk lesions.
A prior diagnosis increases the risk of future skin cancers as patients age, which is associated with lifestyle patterns and often widespread areas of sun exposure.
Extensive skin field cancerisation (EFSC) refers to the accumulation of ultra-violet light (UVL)-damage and genetic mutations that heighten the risk of cancerous transformation. EFSC is frequently associated with widespread areas of pre-cancerous actinic keratoses that are at risk of cancerisation, and therefore also require treatment.
Often patients with ESFC have a protracted history of multidisciplinary management and combination therapy such as topical antineoplastics, photodynamic therapy (PDT), cryotherapy, curettage and electrodessication, and excisions. Some patients, with persistent changes despite trialling other therapeutic options, are looking for non-invasive strategies to manage disease.
Technological advances in radiation therapy, such as volumetric modulated arc therapy (VMAT), allow treatment to be sculpted to large areas of skin affected by pre-cancerous lesions and invasive disease, known as wide field radiotherapy.
Recent 12-month follow-up data has revealed promising outcomes for patients with extensive disease who were treated with widefield radiotherapy. These data underscore some promising advances in the radiation therapy space, particularly how it can be applied to different presentations of skin cancer.
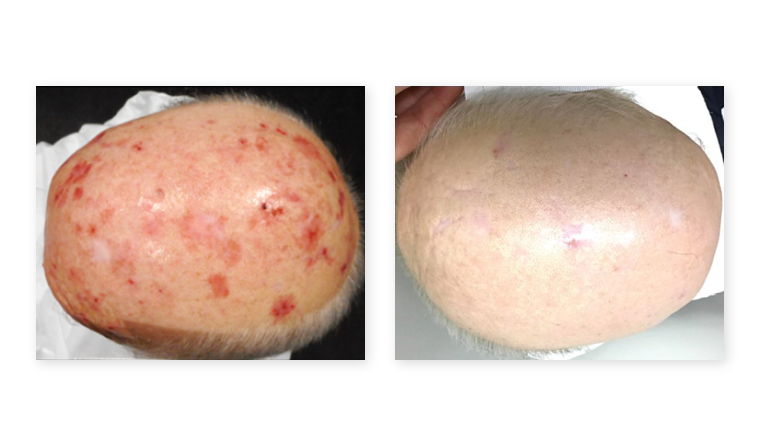
A patient treated with widefield radiation therapy, showing scalp before treatment commenced, and at 24-month follow-up. (Image: Supplied)
GPs are integral to the diagnosis and treatment of skin cancer, and the longitudinal management of patients with widespread disease.
As such, Genesis Care is offering a holistic, GP-focused education program on skin cancer and the role of radiation therapy, covering definitive, adjuvant treatment both for local and regional control and widefield interventions.
Modern Radiation Therapy techniques for the treatment of Keratinocyte Carcinomas (Non-Melanoma Skin Cancer)
This program features four modules, each running for 60–90 minutes, covering:
- keratinocyte cancer incidence, risk factors and treatments
- radiation therapy advances, its application to skin cancer and treatment guidelines
- radiation therapy skin reactions, patient management and FAQs
- interactive case study analysis and referral guidelines.
The first three modules are completed online at the learner’s own pace with incorporated assessment and feedback. The final module is a live, interactive webinar led by a local radiation oncologist, with a focus on real-world case studies. These sessions are small (10–15 participants) to encourage participation and provide an opportunity to ask direct questions.
This program is accredited as part of the RACGP continuing professional development (CPD) program for a full 40-CPD points. It is also eligible for ACRRM and Skin Cancer College CPD hours-based learning.
To register, visit Genesis Care online education program and use the code ‘SKINRT’ when registering.
Log in below to join the conversation.
Genesis Care keratinocyte radiation therapy skin cancer
newsGP weekly poll
Health practitioners found guilty of sexual misconduct will soon have the finding permanently recorded on their public register record. Do you support this change?