News
mRNA COVID vaccine ‘well-tolerated’ in adolescents
According to Pfizer, its vaccine is safe and effective in children as young as 12, which could be crucial for herd immunity.
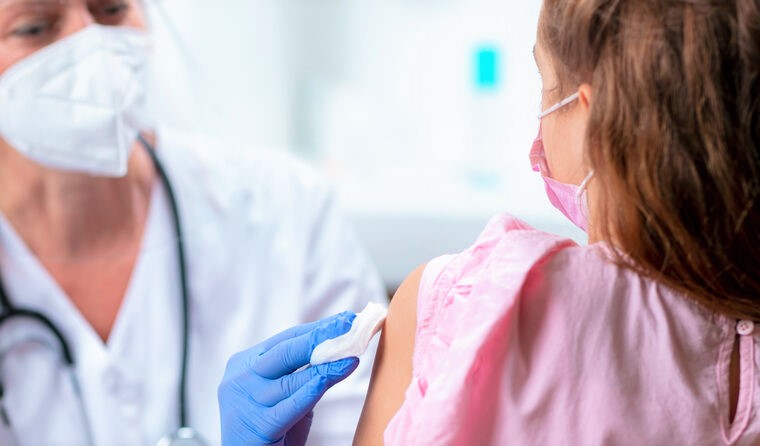 Pfizer/BioNTech is calling for its COVID-19 vaccine to be expanded for use in children, following the latest clinical trials.
Pfizer/BioNTech is calling for its COVID-19 vaccine to be expanded for use in children, following the latest clinical trials.
The latest information is reportedly based on results from a recent phase 3 trial involving 2260 adolescents aged 12–16, in which the vaccine was ‘well-tolerated’ and demonstrated ‘100% efficacy and robust antibody responses’.
‘We share the urgency to expand the authorisation of our vaccine to use in younger populations and are encouraged by the clinical trial data from adolescents between the ages of 12 and 15,’ Pfizer CEO Albert Bourla said.
‘We plan to submit these data to the FDA [US Food and Drug Administration] as a proposed amendment to our Emergency Use Authorisation in the coming weeks and to other regulators around the world, with the hope of starting to vaccinate this age group before the start of the next school year.’
Locally, the Therapeutic Goods Administration (TGA) has granted the Pfizer/BioNTech vaccine provisional approval for people aged 16 years and older, while the Oxford University/AstraZeneca vaccine has been approved for use in people 18 years and older.
The safety and efficacy results could prove crucial, as experts have expressed concern that herd immunity cannot be achieved without children being vaccinated.
‘If you do the mathematics, it’s just not possible because we’re not vaccinating children and there’s about 20% of people who won’t get the vaccine,’ Burnet Institute epidemiologist Professor Michael Toole previously told newsGP.
A University of Sydney preprint simulation of a COVID-19 vaccination program comprising 10 million people receiving the Pfizer/BioNTech and 10 million receiving the Oxford University/AstraZeneca vaccine – but only covering roughly half of the school-aged children population – also found that such an approach will not allow Australia to achieve herd immunity.
In addition, they concluded that unvaccinated children may transmit the virus freely among people most at risk, supporting the need for children to be vaccinated to achieve herd immunity.
Even though Australia is yet to approve the vaccine for children, clinical trials are underway.
Meanwhile, the University of Melbourne has released a new, interactive modelling tool designed to judge what levels of restrictions will be needed to contain outbreaks as the number of people getting vaccinated grows.
The COVID-19 Pandemic Trade-offs will analyse 648 potential scenarios over the next 12 months, based on vaccine uptake and efficacy.
The tool allows users to explore how SARS-CoV-2 infection rates, health impacts and economic impacts vary by which strategy Australia chooses to execute:
- aggressive elimination – aim for no community transmission, quickly
- moderate elimination – aim for no community transmission, less quickly
- tight suppression – aim for 1–5 new cases per million people per day
- loose suppression – aim for 5–25 new cases per million people per day
These variations will also depend on whether the chosen strategy remains consistent, or relaxes as vaccination coverage increases.
In addition to the strategy choices, values can be set for different scenarios on vaccine uptake, efficacy at reducing transmission, and the unmitigated reproduction rate of the virus strains in circulation.
In a presentation of the model, lead epidemiologist Professor Tony Blakely wrote that the ‘pretty pessimistic’ or ‘worst-case’ scenario is based on a 60% vaccine uptake, 75% efficacy for community transmission, and an
R0 of 3.75.
If an outbreak occurred and loose suppression restrictions were in place, daily cases would likely grow to more than 1000 during the phase 2a and phase 3 vaccine rollout, the model shows.
‘The likelihood of future uncontrolled outbreaks is – unsurprisingly – considerably greater if we adopt a loose suppression approach,’ Professor Blakely wrote.
‘The risk varies markedly with the R
0 of the circulating variant. Therefore, the greater infectivity of new variants is of grave concern until vaccine coverage is high for a vaccine that reduces transmission.’
Professor Blakely’s ‘best guess scenario’ comprises uptake of 75%, preventing 90% of community transmission, also with an R
0 of 3.75.
As more people received vaccines, case numbers could be kept at less than 10 a day using the aggressive and moderate elimination strategies.
‘An ongoing aggressive elimination strategy – as per New Zealand and Victoria in 2020 – will not be optimal as vaccine coverage increases,’ Professor Blakely wrote.
‘But we need to minimise viral incursions from overseas until vaccine coverage is high.’
He believes a ‘critical discussion’ will occur in 2021 about whether children should be vaccinated once the adult population receives their doses.
‘If children are not vaccinated, an Australian population strongly resilient to incursions of the virus is unlikely,’ Professor Blakely wrote.
‘As
shown by others, herd immunity will be hard – if not impossible – to achieve without vaccinating children.’
Log in below to join the conversation.
children COVID-19 herd immunity Pfizer vaccine
newsGP weekly poll
Are you interested in prescribing ADHD medication?