News
One of the world’s most contagious viruses has returned to Australia
Measles was eliminated in Australia five years ago, but new cases are streaming in from overseas.
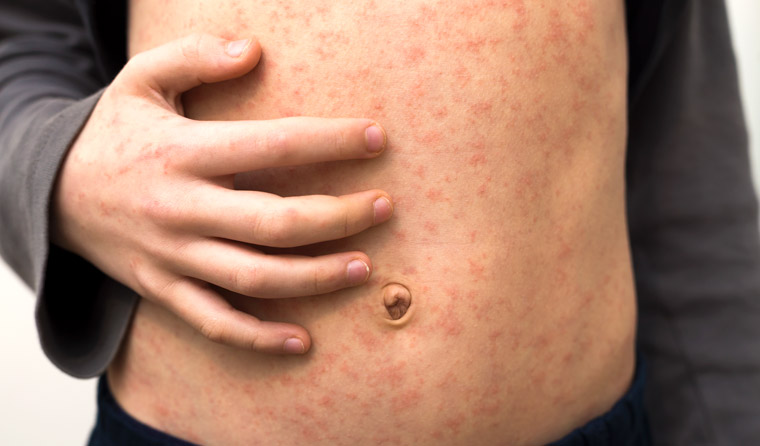 Dr Jon Adams was only able to confirm measles when his patient’s flu swab came back negative and he presented with a rash
Dr Jon Adams was only able to confirm measles when his patient’s flu swab came back negative and he presented with a rash
It was late Friday afternoon a few weeks ago when a young man walked into Dr Jon Adams’ consulting room at the Northern Beaches Medical Centre in Sydney.
He had been in before with bad flu-like symptoms. The flu swab came back negative.
This time, the young man came back complaining that he had woken up with a rash and conjunctivitis.
‘As soon as I saw that, I knew straight away it was more serious,’ Dr Adams told newsGP.
The rash was the tell-tale sign of measles, one of the most contagious viruses known to humans. A single person with measles can infect 12–18 others in an unvaccinated population.
And while most people recover, the virus can lead to lethal complications.
Children’s author Roald Dahl lost his seven-year-old daughter to the virus in 1962.
He later wrote movingly about the tragedy:
‘Are you feeling all right?’ I asked her.
‘I feel all sleepy,’ she said.
In an hour, she was unconscious. In twelve hours she was dead.
Now a measles patient was sitting in front of Dr Adams.
Australia was declared free of the contagious virus in 2014, meaning there was no ongoing local transmission. But the virus is alive and well overseas, with a serious outbreak in Auckland, New Zealand, as well as in the Philippines and many other countries.
The latest global outbreak is the largest since 2006, with almost three times the number of cases reported this year compared to last year. Australia has seen an unusually high number of cases this year.
Dr Adams’ patient had just returned from a holiday in New Zealand.
Once he saw the rash, Dr Adams knew important steps had to be taken.
‘As soon as the diagnosis was made, we isolated the person and made contact with NSW public health to tell them we had a suspected case of measles,’ he said.
‘We then closed the medical centre and ensured people who were in the waiting room were managed for their exposure.’
That meant asking everyone in the waiting room their measles immunisation status and offering on-the-spot immunisations to anyone who was a risk, such as an infant who had not yet had his 12-month measles-mumps-rubella (MMR) vaccine.
Another person could not be given live vaccine, so was given immunoglobulin.
Giving the vaccine within three days of exposure mitigates the risk, Dr Adams said.
The clinic – which is located in the Northern Beaches Hospital – then closed for a comprehensive terminal clean, to remove any trace of the highly contagious virus from areas the patient visited, including the waiting room, bathroom and consultation room.
Then patients who might have previously been in contact with the measles patient on previous visits needed to be notified. That job – contact tracing – was done by NSW’s public health unit.
‘Public health contacted them the following morning. Of that group, about half came back immediately,’ Dr Adams said. ‘That day, we had one doctor designated to manage those contacts.’
Dr Adams praised the public health unit.
‘It was a great team effort; they ordered in more vaccines and immunoglobulin for us and coordinated the response from their premises,’ he said.
‘Anyone in the waiting room was at risk of exposure.’
 Dr Jon Adams and Dr Penny Burns had to rapidly manage a case of measles within their practice.
Dr Jon Adams and Dr Penny Burns had to rapidly manage a case of measles within their practice.
For Dr Adams, the measles case – which led to a public alert – came as a wake-up call.
His patient’s condition deteriorated, eventually leading to pneumonia. After a stint in hospital, he eventually made a full recovery. The patient’s sister also came down with the virus.
‘What makes measles hard is that the initial symptoms are indistinguishable from a flu-like illness. It was only when the flu swab was negative and he returned with the rash that we knew,’ Dr Adams said.
‘We see a lot of flu as a medical centre located adjacent to an emergency department. We knew that there were lots of cases of measles overseas, so it’s been at the back of our minds.
‘But the reality of what needs to happen when you do finally see a measles patient, it’s a wake-up call. You need to be very proactive and make sure you take all necessary steps to keep all staff and patients safe.’
Dr Adams said the case has focused his attention on his patients’ travel histories.
‘Travel histories are really important. If people are coming back from a hotspot, it’s important to think of this diagnosis early on,’ he said.
‘Public health would much rather you call and seek advice earlier rather than later.’
Australian National University researcher and disaster medicine specialist GP Dr Penny Burns also works at the clinic.
‘There’s been an increase in measles globally. We need 95% coverage for herd immunity and there’s been a dip in vaccinations in some places,’ she told newsGP.
‘The risk is really high when you’ve got pregnant women or people who can’t be immunised in your waiting room. You have to contain the case quickly, isolate them and manage contacts.
‘This is quite a serious disease and can be fatal. The scary thing about measles is that you can get a devastating brain problem – sub-acute sclerosing panencephalitis – years after the virus, which is fatal.’
Across the Tasman, New Zealand GP Dr Phil Schroeder has been tackling the ongoing measles outbreak for months, which he describes as ‘very disruptive’.
Dr Schroeder provides emergency support to GPs in the Canterbury region on the South Island. Measles has consequently become a large component of his work.
‘In March we had an outbreak in my province of Canterbury, but the large outbreak at the moment is in Auckland, which has literally gone ballistic. It’s become a large epidemic,’ he told newsGP.
‘It’s having a huge impact. Every time a parent calls up concerned about their child’s rash, we have to treat it as if it is [measles], until proven otherwise. That means we won’t see the person in the facility if we get pre-warning and instead triage them in their car or the carpark, if at all possible.
‘We are getting two or three a week at the moment, and though most are false alarms it still creates pandemonium.
‘It’s the most contagious virus known to humankind – it trumps just about everything else.’
New Zealand also declared measles eliminated in 2017.
‘Most of the developed world has eliminated it, but it’s now taken off as a worldwide phenomenon,’ Dr Schroeder said. ‘That means vaccine stocks are at an all-time low, just as we might want to vaccinate more.’
And the outbreak seems far from over. Dr Schroeder predicts that, with the constant volume of air traffic between Auckland and Australia, a larger outbreak was almost certain.
infectious disease measles public health travel medicine
newsGP weekly poll
Within general practice, do you think there are barriers to providing flu vaccinations? If so, what are they?