News
Pandemic delays cancer diagnoses
Research shows a new pandemic could be just over the horizon, and this time it’s cancer.
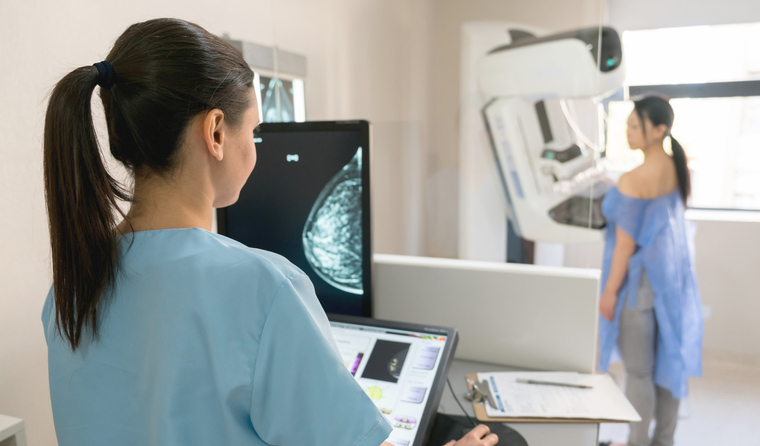 Around 145,000 fewer mammograms were conducted between January and June 2020 compared to the same period in 2018.
Around 145,000 fewer mammograms were conducted between January and June 2020 compared to the same period in 2018.
New research from the United States has confirmed what health professionals have long suspected and feared – restricted access to healthcare services during the COVID-19 pandemic has seen a delay in cancer diagnoses.
Led by the University of Maryland School of Medicine, researchers examined data from more than nine million veterans at over 1200 medical facilities and found that new cancer diagnoses have reduced by 13–23% on pre-pandemic levels, depending on cancer type.
Across the board in 2020, the data revealed that colonoscopies, prostate biopsies, cystoscopies and chest computed tomography (CT) scans were all used less frequently. In particular, colonoscopies, prostate biopsies, cystoscopies and chest CTs decreased by 45%, 29%, 21% and 10% respectively.
‘The disruption in non-emergency healthcare during the peak of the pandemic was intentional and necessary,’ research lead Dr Brajesh Lal said.
‘As we enter the recovery phase, we hope that our work will help physicians, hospitals, and healthcare organisations anticipate the extent to which they have fallen behind in their efforts to diagnose new cancers.
‘It will also help them allocate requisite resources and time to re-engage with patients.’
The backlog in cancer detection is not isolated to the US. Although research into the rates of cancer diagnoses during COVID-19 is still ongoing in Australia, a reduction in population-based screening of asymptomatic patients has been observed nationwide, with data from the Australian Institute of Health and Welfare (AIHW) showing that fewer mammograms and cervical screening tests (CST) were performed in 2020.
There were around 145,000 fewer mammograms between January and June 2020 compared to the same period in 2018, mainly due to lockdowns and the temporary closure of breast screening clinics.
Screening rates did improve in the latter half of 2020 once restrictions eased and services resumed, but an ongoing breast screening backlog has seen patients and GPs calling for extra screening capacity to address the void.
BreastScreen Victoria CEO Terri Smith told newsGP that since reopening, they have experienced high demand and longer wait times at some of their clinics due to having COVID-19 safety measures in place.
‘To accommodate these important measures, we had to reduce the overall number of appointments available,’ she said.
‘We’re working hard to open up more appointments across our program in a safe and sustainable way.’
A similar decline was seen in cervical screening numbers during the pandemic, with AIHW data showing fewer tests performed in 2020 than in 2019. However, it is difficult to comment on the true pandemic impact due to recent changes in the National CST Program, which saw Pap smears being replaced by the new five-yearly CST from 1 December, 2017 onwards.
Although the pandemic did not appear to have a direct impact on bowel cancer screening rates, it is important to note that the National Bowel Cancer Screening Program broadened its target group and increased frequency of testing in recent years.
Like the changes to cervical screening, this makes it difficult to assess the impact of the pandemic on patterns of bowel cancer screening due to a greater number of invitations being sent out around this period.
GPs need look no further than their own backyard to see the potential devastating impact cancer can have; it does not discriminate and can affect anyone at any time, with the late RACGP President Dr Harry Nespolon having passed away in 2020 following a battle with pancreatic cancer.
Current RACGP President Dr Karen Price is no stranger to cancer either. She recently discussed her experience with breast cancer for which she underwent a double mastectomy moments after being informed she had won the RACGP presidential election.
‘We need people to just keep up with seeing their GP for check-ups, for going into the routine screens, for understanding that health and disease are not inseparable, but they intertwine because that’s the life of being human,’ she said.
With COVID relatively well contained in Australia at present Ms Smith says patients are thankfully starting to resume screening and health checks. But the longer-than-usual waiting lists mean it is more important than ever for GPs and patients to arrange timely appointments.
‘It has been great to see demand for our service, which indicates that women are feeling comfortable to come back and screen,’ she said.
‘While waiting times are higher than average due to COVID-19 safety measures in our clinics, appointments are available.
‘We encourage any clients invited for their regular breast screen to book an appointment as soon as possible.’
Log in below to join the conversation.
cancer cancer diagnosis cancer screening pandemic
newsGP weekly poll
Would it affect your prescribing if proven obesity management medications were added to the PBS?