News
Pulse oximeters ‘no better than asking patients’: Study
Using pulse oximeters offers no noticeable improvement in health outcomes for COVID-19 patients in home care, a trial carried out in the US suggests.
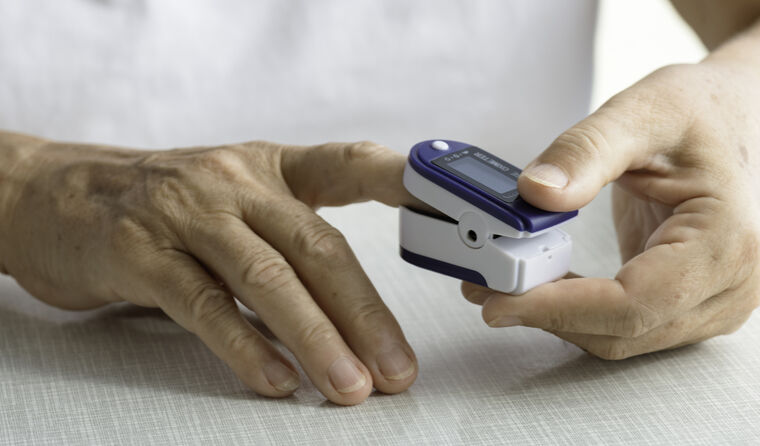 Pulse oximeters have been widely distributed as part of the response to COVID-19.
Pulse oximeters have been widely distributed as part of the response to COVID-19.
Researchers in a randomised trial on pulse oximeters have said using the devices may not improve outcomes if COVID-19 patients are already being monitored.
The research, published in the New England Journal of Medicine (NEJM) this week, was carried out at the University of Pennsylvania’s Perelman School of Medicine.
The trial looked at the results of 611 patients confirmed with COVID-19 who were given a pulse oximeter to use at the same time as participating in the organisation’s COVID Watch program, which sends automated text messages to monitor patients at home.
A control group of 606 COVID-19 patients only took part in the COVID Watch program.
The main outcome measured the number of days each patient was alive and out of hospital for the 30 days after they were enrolled in the study.
‘Among patients with COVID-19, the addition of home pulse oximetry to remote monitoring did not result in a greater number of days alive and out of the hospital than subjective assessments of dyspnea alone,’ the NEJM correspondence describing the trial states.
The number of days the patients in the pulse oximetry group spent alive and out of hospital worked out at a mean of 29.4 days compared to 29.5 days in the control group.
There were 43 hospitalisations and five deaths within the group that included pulse oximeters, and 41 hospitalisations and three deaths in the standard program.
‘Compared to remotely monitoring shortness of breath with simple automated check-ins, we showed that the addition of pulse oximetry did not save more lives or keep more people out of the hospital,’ Assistant Professor Anna Morgan, the medical director of the COVID Watch program and one of the lead authors for the study, said.
The researchers also said there was no notable difference according to ethnicity.
Pulse oximeters have been employed in many international responses to COVID-19, including Australia, largely due to concerns about the potential for the disease to cause silent hypoxia.
Dr Nicole Allard, a Melbourne GP who co-Chairs the Primary and Chronic Care panel of the National COVID-19 Clinical Evidence Taskforce, said the study emphasises the importance of keeping up to date with emerging research.
‘It’s really important that there’s ongoing evaluation and embedded research in our approach to a new disease,’ she told newsGP.
However, Dr Allard is also careful not to rush to conclusions about the use of the devices.
‘This study shows that just giving someone a pulse oximeter and getting them to record it regularly didn’t necessarily make a difference,’ she said.
‘It doesn’t say that the practice of getting pulse oximeters out to people in the community, especially people at higher risk of deterioration, isn’t a worthwhile exercise.
‘I think what it says is the way we use pulse oximeters maybe needs to be examined further.’
Dr Allard also says the devices had proved effective with earlier variants of concern.
‘Especially during the Delta wave, it was very useful to have pulse oximetry augmenting assessment of someone with extreme fatigue,’ she said.
Last October, the Federal Health Minister Greg Hunt announced that general practices would be supplied pulse oximeters via the National Medical Stockpile and Primary Health Networks (PHNs) to help monitor symptomatic patients being managed in the home.
More than $22 million was allocated to supply pulse oximeters and help PHNs distribute them alongside PPE in the Mid-Year Economic and Fiscal Outlook last December.
The devices are targeted for use among patients with a higher risk of complications to allow them to self-monitor oxygen saturation levels. They are currently being provided both through primary care and hospital programs.
However, the exponential increase in case numbers due to the Omicron variant of concern has changed the dynamics surrounding distribution of the device, Dr Allard says – and that might mean its use needs to be even more targeted.
‘Things are going to change, whether it’s early treatment or how to monitor people, and we have just got to keep scanning the literature and being aware of what’s happening out there,’ she said.
‘There’s just been such a deluge of research, it’s impossible for any individual clinician to keep up with it.’
The study authors noted there is currently no evidence to suggest that patients who cannot access a monitoring scheme or on-call clinicians would not benefit from the use of pulse oximeters.
‘Overall, these findings suggest that a low-tech approach for remote monitoring systems based on symptoms is just as good as a more expensive one using additional devices,’ Assistant Professor Krisda Chaiyachati, one of the principal investigators for the research, said.
A spokesperson for the National COVID-19 Clinical Evidence Taskforce told newsGP it is aware of the study.
‘The evidence team are currently reviewing [the research] and implications for our recommendations will be considered at the Primary and Chronic Care panel at their next meeting,’ they said.
The RACGP’s most recent Home-care guidelines for patients with COVID-19 are available on the college website.
Log in below to join the conversation.
COVID-19 NEJM New England Medical Journal pulse oximeters