News
What GPs need to know about the flesh-eating Buruli ulcer
With Buruli ulcer now at epidemic levels in parts of Australia, the RACGP has developed a new educational activity for GPs.
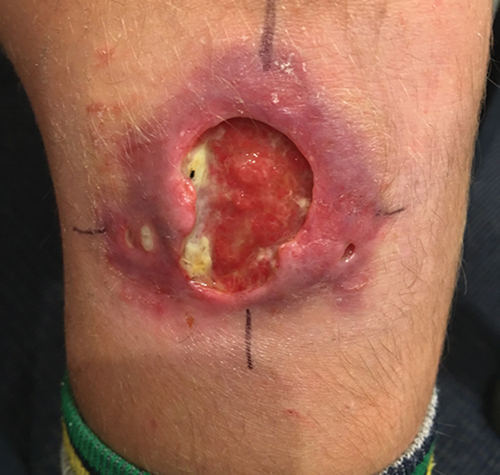
 Ulcers can initially present as relatively minor before exhibiting more severe symptoms.
Ulcers can initially present as relatively minor before exhibiting more severe symptoms.
WARNING: ARTICLE CONTAINS GRAPHIC IMAGE
Australian cases of the rare flesh-eating Buruli ulcer are rising rapidly, leading experts to call for an equally rapid scientific response.
The ulcer, caused by bacterium mycobacterium ulcerans, can cause large, destructive lesions of skin, soft tissue and even bone.
Statistics in a new Medical Journal of Australia (MJA) article show that case numbers have grown to their highest ever level, with 236 cases recorded between November 2016 and November 2017. The bacterial infection, which has been known to exist in Australia since 1948, is said to be particularly devastating on Victoria’s Mornington Peninsula, with confirmed infections increasing by around 400% in the last four years.
‘[In Victoria], the community is facing a worsening epidemic, defined by cases rapidly increasing in number, becoming more severe in nature, and occurring in new geographic areas,’ the MJA authors write, led by Associate Professor Daniel O’Brien, an infectious diseases consultant with Barwon Health in Geelong.
Buruli ulcer is associated with wetlands, particularly those with stagnant water, but the exact method of transmission is still unknown. Theories include floods, mosquitoes, possum faeces or spray irrigation.
The disease can strike people who have visited affected areas even for a single day.
In response, the RACGP has produced targeted information and a professional educational activity aimed at helping GPs identify and manage the ulcer. ‘
Identifying and managing Buruli ulcer’ is designed to help GPs with the diagnostic challenge of distinguishing the rare Buruli ulcer from far more common skin ulcers.
Early identification of the Buruli ulcer is essential for successful management. Cure rates
approach 100% on combination antibiotic regimens such as rifampicin and clarithromycin. However, these drugs are not listed on the Pharmaceutical Benefits Scheme (PBS) and can have severe side effects. Many patients also need plastic surgery to repair the damage.
According to the RACGP, ‘Identifying and managing Buruli ulcer’ is one of the first educational activities made by GPs for GPs in the diagnosis and management of Buruli ulcer.
The most important risk factor for acquiring Buruli ulcer is having lived in or visited an endemic region. These regions include the Mornington and Bellarine peninsulas near Melbourne – where the ulcer is sometimes dubbed the Bairnsdale Ulcer. In Queensland, it is known as the Daintree Ulcer.
The lesions are most frequently found on exposed body areas and infection may be linked to many factors, including insect bites, environmental contamination or trauma.
Buruli-ulcer flesh-eating-ulcer mycobacterium-ulcerans
newsGP weekly poll
How often do patients ask you about weight-loss medications such as semaglutide or tirzepatide?