News
Why global COVID vaccination rates matter to Australia
There has been a huge focus on issues plaguing the national vaccine rollout, but some of the country’s foremost experts say trends emerging in other parts of the world are equally concerning.
 Developing nations with uncontrolled outbreaks like India are at a high risk of generating variants of concern. (Image: AAP)
Developing nations with uncontrolled outbreaks like India are at a high risk of generating variants of concern. (Image: AAP)
This week Israel, a first-world country with one of the highest rates of fully vaccinated people in the world, reinstated an indoor mask mandate after recording its highest daily case numbers in months.
The surge, fuelled by the Delta variant of concern that emerged during India’s massive second wave, is ‘a warning’, epidemiologist Professor Mary-Louise McLaws told newsGP.
She believes that regardless of domestic vaccination rates, Australia is unlikely to be fully protected from COVID while it continues to rage unchecked in the developing world.
‘The longer that low- and middle-income countries are not able to vaccinate, the greater the “test tube playground” is for this virus to go into people who may be immunocompromised and learn how to develop an even more efficient method of infection,’ Professor McLaws said.
‘It appears in the real-world rollout that before Delta happened, Pfizer was protecting Israel very well as their case numbers had dropped remarkably by about 200-fold at one stage.
‘But with Delta recently, you’re seeing all sorts of breakthroughs.’
Professor McLaws, an adviser to the World Health Organization (WHO) Infection Prevention and Control Guidance Development Group for COVID-19, says developing nations with uncontrolled outbreaks like India, are at a high risk of generating variants of concern.
This is because many people living there cannot afford to follow even basic public health measures, like mask wearing or stay-at-home orders, as they live hand-to-mouth and missing out on a day of work equates to missing a day of food. As a consequence, access to vaccination is even more important for these countries, she says.
‘In Africa, they’re really worried about the spread of variants of concern, while the WHO [also] expressed great concern at our recent meeting about Delta spreading across the world at a very fast pace,’ Professor McLaws said.
‘The G7 has just promised vaccine supply for 500 million people, yet … that doesn’t even cover the two billion living in extreme poverty, let alone poverty.
‘So, it really is a drop in the ocean. And they know it. It was underwhelming.’
Professor McLaws is also a Director of Australia’s Immunisation Coalition, which is calling for donations to UNICEF Australia to improve access to the COVID-19 vaccine in low-income countries.
‘Viruses are fairly psychopathic. They use our human foibles to improve their transmissibility … [and] learn how to effectively go from one person to the next much more rapidly,’ she said.
‘They don’t need sleep. They’re a formidable warrior.’
And while many vaccination programs are continuing at pace – particularly in the developed world – many countries are struggling to keep up with a global surge in COVID cases.
The UK, which has one of the world’s highest COVID vaccination rates, has delayed its emergence from lockdown amid a third wave of infection that’s primarily impacting younger people, while Russia is expecting to register 25,000 cases per day by the end of June.
Even countries that have already been ravaged by coronavirus, and therefore have theoretically higher immunity rates, are struggling.
Brazil set a new national record on Wednesday with 115,228 new cases identified within 24 hours, and India is already warning about a Delta Plus variant that local health authorities suggest has increased transmissibility, stronger binding to receptors of lung cells, and potential reduction in monoclonal antibody response.
But despite the resurgence, GP and Immunisation Coalition Chair Dr Rod Pearce told newsGP Australians can still help the global – and local – battle against COVID by donating $10 to provide a person in need with a vaccination.
‘The numbers here and the numbers overseas are going to be what changes the game and will allow us to go back to lives where COVID is just one of the extra diseases we have, rather than the main one,’ he said.
‘If you feel like you actually want to do something and be part of solving the problem internationally, then you’re actually solving the problem here as well.’
Dr Pearce likened the push for equitable access to vaccines to a macro form of the preventive medicine that GPs practice every day.
‘It’s like diabetes – okay, you made a diagnosis. But what about tomorrow? What about in six weeks’ time? What about six months’ time? What about six years’ time?’ he said.
‘Well, you can do stuff today that will actually make a difference, so that in six years’ time we’re all better off … because all those variants and that sort of stuff are not going to be here.’
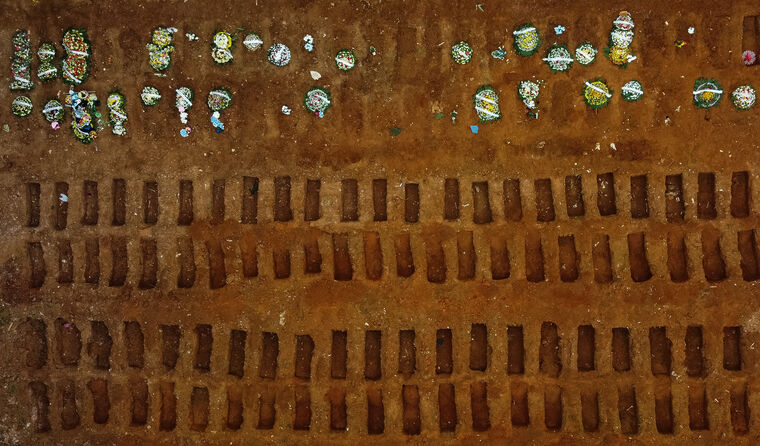
More than 500,000 people have died from COVID in Brazil, where at least one variant of concern has already emerged.
Director of the Immunisation Coalition Scientific Advisory Committee and noted infectious diseases paediatrician Professor Robert Booy told newsGP the idea is to ‘give back and pay forward’.
‘Five million people have had a vaccine in Australia so far for free. And yet, there are five billion people in the [developing] world who need to be vaccinated,’ he said.
‘The concept that you can give just $10 and protect someone else – it’s pretty special.’
The WHO estimates that around 3.9 million people have died from COVID-19 since the pandemic began, with developing countries at higher risk due to the lack of resources, infrastructure and vaccine supply.
To help combat this and control the risk of ‘vaccine nationalism’, the WHO launched the COVAX initiative, which Australia joined in September 2020.
Yet despite representing only 14% of the world’s population, high-income countries have reserved more than half of the world’s COVID-19 vaccine doses, representing a significant global issue and threat to herd immunity, according to Professor Booy.
‘This [vaccine coverage] compares to less than 5% vaccine uptake in low-income countries, which represents approximately two-thirds of the world’s population,’ he said.
‘Having no or one vaccine still allows you to get infected, and getting infected allows the virus to mutate. One virus in a chain of transmission has a new mutation about every two weeks.
‘Most of [the variants] are not a problem, but now and then a new one emerges, which increases transmissibility [or resistance]. At the moment everyone’s talking about Delta, but what we’re worried about is the “Omega” strain … that might be the end of us.
‘I’m exaggerating, but … it’s definitely in GPs’ interest for the whole world to get on top of this, in order to basically protect them from having to deal with patients who may have future variants of concern.’
Global collaboration to combine funds from higher income countries to provide vaccines for low- and middle-income countries is a necessary part of achieving herd immunity and reducing COVID-19 death rates, which Professor Booy says the Immunisation Coalition’s fundraiser is part of.
And without herd immunity, Prime Minister Scott Morrison warned earlier this week that Australia could see 5000 cases per day once borders open, even with high vaccination coverage.
But Australia’s borders cannot stay closed indefinitely, which is why Professor McLaws says Australians must take an interest in vaccinating people overseas.
‘We need to get clever and help everybody else,’ she said. ‘If we just help ourselves, we’ll have to keep the borders closed forever.
‘It’s not a Russian Roulette game that you want to play; you really want everyone to be vaccinated at a very high rate.’
To date, the Immunisation Coalition has raised almost $30,000 for vaccine access to developing countries.
Log in below to join the conversation.
COVAX COVID-19 developing nations herd immunity vaccination
newsGP weekly poll
Within general practice, do you think there are barriers to providing flu vaccinations? If so, what are they?