News
Working to prevent overdiagnosis
A number of global medical heavyweights will come together in Sydney for next month’s Preventing Overdiagnosis Conference.
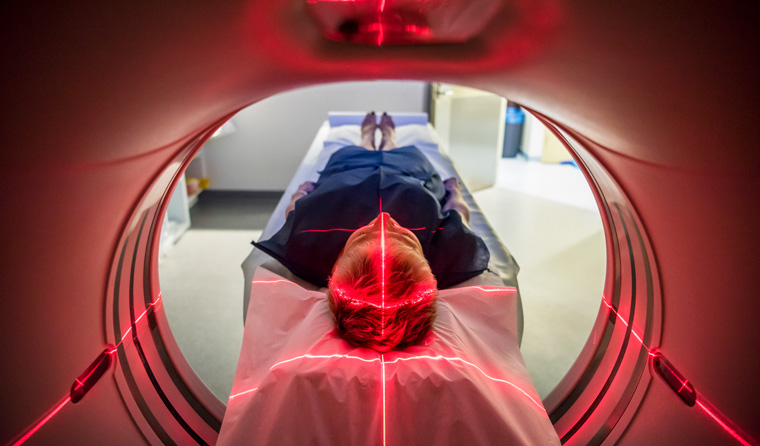 Unnecessary testing can be painful and divert resources away from patients in actual need of care.
Unnecessary testing can be painful and divert resources away from patients in actual need of care.
Set to take place on 5–7 December, the conference will examine the concept of ‘too much medicine’ and the growing evidence that overdiagnosis is a major threat to human health.
Dr Anna Stavdal, keynote speaker and President-Elect of the World Organisation for Family Doctors (WONCA), told newsGP that overdiagnosis has been a special interest of hers for the past 25 years.
‘Early in my career new “preventive medicines” started to flood the market. Cholesterol in particular, and lipids in general, were identified as risk factors for cardiovascular disease and linked to the development, and sale, of statins,’ she said.
‘Antihypertensive drugs became more sophisticated and thresholds for intervention became increasingly lower.
‘We experienced a shift in perspective and tasks in medicine and it affected my daily clinical work. Something was wrong, and I was lucky to work with people who felt a need to put this on the agenda.’
Overdiagnosis, including unnecessary tests and treatments that can be painful and dangerous, carries a risk of complication that can affect quality of life and, in extreme cases, trigger life-threatening problems. It can also be expensive and divert resources away from patients who are in actual need of care.
Assistant Professor Ray Moynihan from Bond University’s Centre for Research in Evidence-Based Practice, told newsGP that while the concept may seem counterintuitive, it can have dire consequences.
‘For example … 40% of the prostate cancer diagnosed in Australia is overdiagnosed, which is a public health crisis causing untold harm and wasting many resources,’ he said.
‘There is a great need for more research to understand the nature and extent of overdiagnosis and overtreatment, what’s driving it and how to wind it back, to reduce harm to people and redirect scarce resources to areas of genuine need.
‘It is a real threat to human health, which is why the World Health Organization [WHO] is co-sponsoring the conference, and why so many influential stakeholders are associate partners with the conference, including consumer groups and medical colleges such as the RACGP.’
The three-day multi-disciplinary conference will feature keynote addresses from the likes of Dr Stavdal and British Medical Journal Editor-in-Chief Dr Fiona Godlee. It will cover a range of topics, including the commercial drivers of overdiagnosis, the risks and benefits of genomics and precision medicine, and addressing overdiagnosis and overtreatment in musculoskeletal conditions.
Dr Stavdal believes overdiagnosis is especially relevant to GPs, as they are a key part of reducing the harms associated with too much medicine.
‘As the first point of care, we can prevent “the snowball from starting to roll” – a well-known metaphor in Norway,’ she said
‘Based on personal knowledge, we can tailor investigations and treatment to the individual, and prevent them from unnecessary testing. We can observe over time and help them navigate the rest of the healthcare system when need be, and not leave them with fragmented solutions, which very often lead to overdiagnosis.’
Dr Stavdal also concedes, however, it is a challenge for GPs to ensure they have the right balance between preventing overdiagnosis and not missing genuine health issues.
‘It can be difficult to find the line, and that is an important part of the job,’ she said.
‘One of the main features of family medicine is to manage, and live with, clinical uncertainty, something you share with your patient. The most helpful tool is to practice real person-centred care.
‘If you know your patient, the personal and the family medical history, the individual’s resources and vulnerability, you stand a better chance to find the tailor-made solutions.
‘Sometimes this can be achieved with the help of medical algorithms, but personal knowledge is the most helpful tool, while trust is a prerequisite and the basis for finding the balance.’
The conference, which the RACGP has accredited a Category 2 Activity, will be preceded by the Practising Wisely workshop, an interactive CPD course designed and run by GPs, for GPs. Co-hosted by Wiser Healthcare, it will aim to educate GPs about reducing unnecessary testing and treatment, while providing practical training opportunities to help address the problem back in the clinic.
Log in below to join the conversation.
Doctors Family of Organisation overdiagnosis WONCA World
newsGP weekly poll
As a GP, do you use any resources or visit a healthcare professional to support your own mental health and wellbeing?