Opinion
COVID-19 and GPs’ leadership role in aged care
GPs will help determine whether Australia’s response is a ‘shocking tale of neglect’ or a powerful legacy, Prof Leanne Rowe writes.
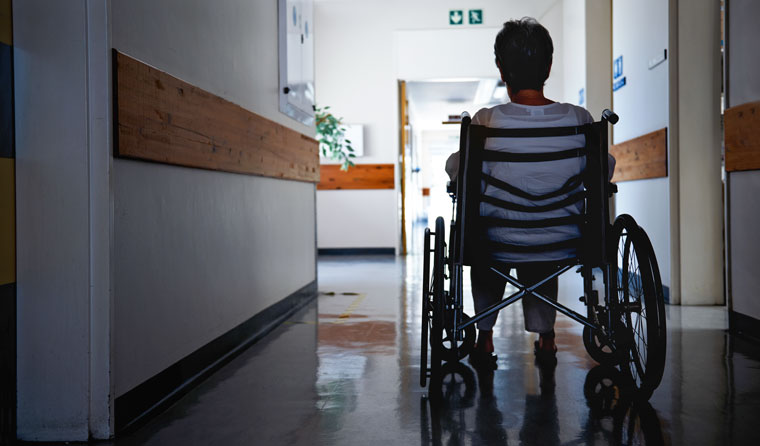 Professor Rowe believes a flattening curve means ‘GPs have the opportunity to prevent the ravaging of more than 200,000 older people in residential aged care facilities’.
Professor Rowe believes a flattening curve means ‘GPs have the opportunity to prevent the ravaging of more than 200,000 older people in residential aged care facilities’.
Of all the images that will haunt us when the COVID-19 pandemic is over, chief among them will be the mass palliation and deaths of vulnerable residents in aged care facilities, particularly in the US and Europe.
As many other countries failed to prepare for the scale and speed of the pandemic, acutely ill aged care residents with COVID-19 or other medical and surgical conditions are reportedly being denied access to hospitals, and refrigerator trucks are acting as morgues because of overburdened funeral homes.
Despite the dire warnings, delays in infection control and lockdowns have resulted in catastrophic aged care COVID-19 outbreaks that spread ‘like fire through dry grass’.
Of course, we all know frail residents are vulnerable. The fatality rate of COVID-19 is about 15% in the over-80 age group, and worse for people with comorbid disorders.
Fortunately, as we are seeing a flattening of the COVID-19 curve in Australia, GPs have the opportunity to prevent the ravaging of more than 200,000 older people in residential aged care facilities.
We still have time to change the course of history.
Many GPs have already ensured their senior patients or their representatives understand how to access remote consultations via telephone and videoconferencing.
Reviews of health assessments, care plans, including asthma, diabetes and mental health plans, and medication management can now be undertaken via videoconferencing, as can consultations by psychiatrists, psychologists, physiotherapists, endocrinologists, pain specialists, geriatricians, ophthalmologists, oncologists and palliative care physicians.
Aged care residents can also be supported to enable their My Health Record to ensure they and their carers have an up-to-date list of current medications, summary of clinical conditions and complex care plans in residential aged care homes.
Clearly, continuity of care and access to the clinical record are of critical importance including when the usual GP is unwell or away, or a patient requires after-hours care, hospitalisation or palliative care.
It is essential that any aged care resident has their psychiatric diagnosis documented in their My Health Record, especially if they are taking any psychotropic medication. Without this clinical information, aged care facilities are failing their accreditation due to alleged chemical restraint and are being sanctioned, resulting in further cuts in funding.
Residential aged care facilities must also consider ways to encourage face-to-face health consultations for their residents during the pandemic.
The draft RACGP aged care standards recommend facilities make provision for a GP consultation/treatment room (eg a simple disinfected room with desk, chair, bed and sink), which is now even more important for face-to-face visits to protect all staff and residents, and to allow appropriate procedures to be performed out of hospitals.
As aged care facilities have special access to personal protective equipment (PPE) and other infection control measures, there should not be any risk to GPs or other health professionals who visit.
In addition, GPs can address many of the major quality and safety issues highlighted in the interim report of the (now postponed) Royal Commission into Aged Care Quality and Safety, entitled ‘A shocking tale of neglect’.
A number of examples of substandard care were highlighted by the royal commission, including the lack of access to general practice and other health services, resulting in:
- inadequate prevention and management of wounds
- poor continence management
- poor food, nutrition and hydration
- insufficient attention to oral health, leading to widespread malnutrition, chronic dental and other pain, and secondary conditions
- a high incidence of assaults by staff on residents, and by residents on other residents and on staff
- common use of physical and chemical restraint on residents
- overprescribing of psychotropic agents without a psychiatric diagnosis or consent by patients or their representatives
- poor or fragmented palliative care and end-of-life care.
Despite these disturbing findings, many residential aged care facilities provide a high standard of care, but most struggle with limited government funding.
The royal commission also highlighted that our aged care workforce was already under pressure, often doing their best under excessive workloads prior to COVID-19. Consequently, there are ongoing severe difficulties in recruiting and retaining aged care staff, resulting in a lack of continuity of nursing and personal care workers, further inhibiting the ability of GPs and other health professionals to provide a high standard of healthcare in homes.
However, by accurately documenting the complex clinical needs of aged care residents, including psychiatric conditions, GPs may help residential aged care providers access
higher acuity funding to pay more skilled staff to care for their patients.
Although the current lockdown acutely exacerbates many of these quality and safety issues, there are many practical ways GPs can routinely monitor and carefully manage the health and wellbeing of their senior patients, including their mental health.
This is not about over-servicing and cold calls. This is about a patient’s own GP working constructively with residential aged care staff and being proactive about prevention and early intervention, rather than reactive after a crisis.
The RACGP,
Primary Health Networks and
governments are providing valuable resources to GPs, other primary healthcare professionals and aged care providers to help make this a reality.
When we look back at the enduring images after the COVID-19 pandemic is over, I hope Australian GPs will be remembered for their leadership in providing high-quality acute and chronic care, with frequent review of vulnerable patients either in residential aged care homes or in their own homes throughout the pandemic and beyond.
Rather than a ‘shocking tale of neglect’, Australian GPs, in partnership with aged care providers, still have time to leave us with inspiring images of a powerful legacy.
The RACGP has more information on coronavirus available on its website.
Log in below to join the conversation.
aged care coronavirus COVID-19
newsGP weekly poll
Are you interested in prescribing ADHD medication?