News
Formal recognition of rural generalists one step closer
Australia’s specialist general practice colleges are encouraging doctors to provide feedback on an application being assessed by the AMC.
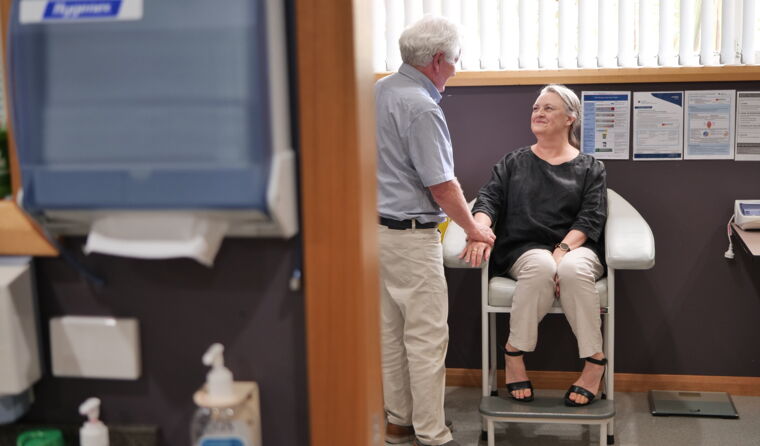 It is hoped formal recognition of rural generalism as its own specialty will improve health outcomes in regional and remote parts of Australia.
It is hoped formal recognition of rural generalism as its own specialty will improve health outcomes in regional and remote parts of Australia.
Public consultation on the second stage application to formally recognise Rural Generalist Medicine (RGM) as a specialist field is now open.
The latest phase in the process has been described as a critical milestone by the RACGP and Australian College of Rural and Remote Medicine (ACRRM), which joined forces five years ago to help initiate the change.
If successful, RACGP President Dr Nicole Higgins said the efforts will help build a strong workforce and encourage focused research to improve rural generalist services.
‘Recognition will value the additional skills and scope provided by rural and remote doctors,’ she said.
‘It shows that as professional bodies, the colleges are committed to general practice, to rural and remote GPs and to the healthcare of rural and remote communities across Australia.’
Once national consultation closes on 12 December, the Australian Medical College (AMC) will draw on findings to collate a report and make a recommendation to the Medical Board of Australia.
This recommendation will then be passed on to the Health Minister’s Committee, which will make the final determination.
‘This is an exciting milestone in our five-year effort to seek RG [rural generalist] specialist recognition,’ ACRRM President Dr Dan Halliday said.
‘We encourage rural and remote GPs and rural generalists to review the application and provide input and feedback via the public consultation. We also encourage community members to participate.
With rural and remote areas currently receiving ‘significantly less’ government-supported services than people in cities, Dr Halliday is hopefully that RGM recognition will help bridge some of the divide.
‘It is expected that building the RG workforce will address the … $6.55 million underspend that currently exists,’ he said.
‘With recognition comes the opportunity to create a single national RG quality standard, which is transparent, safe, purpose-designed, and easily understood by systems, patients and doctors.’
The Rural Generalist Recognition Taskforce is chaired by National Rural Health Commissioner Adjunct Professor Ruth Stewart and include senior representatives from both the RACGP and ACRRM.
Log in below to join the conversation.
ACRRM RACGP Rural Generalist Medicine
newsGP weekly poll
Health practitioners found guilty of sexual misconduct will soon have the finding permanently recorded on their public register record. Do you support this change?