News
Government must ‘urgently and substantially’ invest in general practice: RACGP President-elect
Dr Harry Nespolon predicts a bleak future for Australian healthcare without major Government investment in general practice.
 RACGP President-elect Dr Harry Nespolon believes that while general practice is at the centre of Australian healthcare, ‘it continues to be taken for granted by governments’.
RACGP President-elect Dr Harry Nespolon believes that while general practice is at the centre of Australian healthcare, ‘it continues to be taken for granted by governments’.
Out-of-pocket costs of more than $40 per GP visit and declining bulk billing rates.
That’s the future for Australian healthcare unless the government ‘urgently and substantially’ invests in general practice, according to RACGP President-elect Dr Harry Nespolon.
New RACGP analysis of Medicare data shows that the status quo will result in a total reversal of the recent increase in bulk billing, with the increase to slow to zero and an average out-of-pocket cost of $40.69 per visit by 2020.
‘General practice is the cornerstone of Australians’ healthcare. Unfortunately, it continues to be taken for granted by governments,’ Dr Nespolon said.
‘Although we welcome the return of yearly indexation of patient Medicare rebates, it still does not catch general practice up on the past five years, which has seen an erosion of the patient rebate in real terms.
‘We believe that urgent investment is required.’
Projected out-of-pocket patient costs
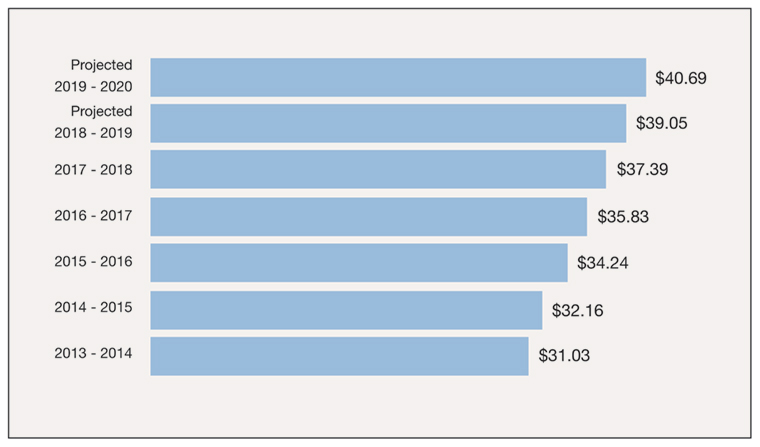 Adapted from the Department of Health. Annual Medicare statistics
Adapted from the Department of Health. Annual Medicare statistics –
Financial year 1984–85 to 2017–18. Canberra: DoH, 2018.
In its 2017 budget, the Federal Government began phasing out the controversial Medicare rebate freeze after five years.
‘Without a significant increase to the rebate and real results from the
MBS review, I am concerned about what the patient experience will look like in the near future,’ Dr Nespolon said.
‘Patients want to spend more time with their GP, and it has been shown that the more time a patient spends with their GP the better their long-term health will be.
‘More effort must be made to keep patients out of hospitals and protected from costly out-of-pocket expenses.’
A recent
report found that Australians are now spending almost $3 billion a year on out-of-pocket non-hospital healthcare.
The new analysis comes soon after the latest official Medicare data showed bulk-billing rates were at a
historic high of 86.1%.
Dr Nespolon said long and complex general practice consultations are not being adequately supported by Medicare, an issue of increasing importance as Australia ages, bringing with it a rising rate of a host of chronic diseases.
‘An extra 10–30 minutes in a GP consultation, particularly for patients with chronic and complex needs, can mean that a condition is identified earlier or health risks, like obesity and mental health issues, receive proper preventive treatment before a patient ends up with a more serious lifelong condition,’ he said.
‘When a GP has the proper amount of time with a patient, we are able to properly treat the whole patient.’
healthcare funding medicare out-of-pocket costs