News
GPs to receive cash incentives to vaccinate aged care and disability workers
The RACGP has welcomed the plan for GPs to collect $1000 once they vaccinate 50 workers, and $20 per worker thereafter.
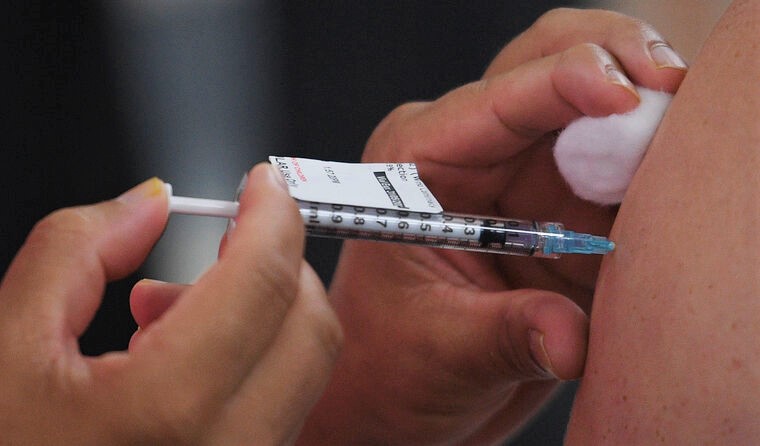 GPs will receive a $1000 payment once they vaccinate 50 vaccinate aged care and disability workers, and $20 per worker thereafter. (Image: AAP)
GPs will receive a $1000 payment once they vaccinate 50 vaccinate aged care and disability workers, and $20 per worker thereafter. (Image: AAP)
With National Cabinet having set national vaccination targets aimed at allowing Australia to reach a post-COVID normal, the Federal Government is now offering GPs cash incentives to help to speed up the rollout and protect vulnerable people in the community.
GPs will now receive a $1000 payment once they vaccinate 50 vaccinate aged care and disability workers, and $20 per worker thereafter. The funding is only available for vaccinations that are provided via a dedicated in-reach service, but can be claimed in addition to existing flag-fall arrangements and the Medicare items for delivering COVID vaccines.
The incentive is cumulative, which mean the vaccinations can be delivered in one or multiple facilities. In addition, the payments can be backdated to mid-April and will be available until the end of October 2021.
RACGP President Dr Karen Price has backed the plan, describing the new incentive payments as a positive step forward.
‘Many people may not realise the vital role GPs play in caring for older people in aged care facilities, so it is a logical step for GPs to be incentivised to vaccinate those who care for people in these facilities,’ she said.
‘GPs are the backbone of the COVID-19 vaccine rollout and they are doing a tremendous job; however, the rollout has presented many challenges for general practice, so these additional payments are just what the doctor ordered.’
The vaccination of Australia’s aged care workers, who are often on the frontline of COVID outbreaks, has moved slowly to this point. Government figures from July showed just one in four of the country’s aged care workers had been fully vaccinated, and 43% had received one dose.
The Government has mandated that all aged care workers must receive their first vaccine dose by mid-September in order to work in the sector.
Dr Price said urgently vaccinating aged care and disability workers could save lives.
‘Vaccinating our older patients and people with a disability is essential,’ she said. ‘However, that is not a complete solution because if workers are not vaccinated they could inadvertently spread the virus to the people they look after, and the consequences can prove disastrous.
‘For any aged care or disability worker my message is straightforward: it is vital that you are vaccinated as soon as possible. Even if you are a young and healthy person, this virus still poses a threat to you and the people you care for.’
According to a Department of Health fact sheet, general practices with capacity to support in-reach clinics should contact their local Primary Health Network (PHN) to coordinate the clinics, and priority consideration may be given to practices that have an existing relationship with a residential aged care facility (RACF).
Both the RACF and general practice must engage with their local PHN before and after any in-reach clinic to report:
- the planned date of in-reach vaccination clinic
- confirmation that the clinic was delivered
- the number of staff vaccinated.
However, disability workforce in-reach clinics may be coordinated directly between disability support providers and primary care providers, without the need to involve their PHN.
To be eligible to receive the payments, primary care providers must report the relevant details for each facility visited through the COVID-19 Vaccine Administrative System (CVAS), which will be functional from Thursday 12 August.
Payments for general practices will be made in November through the Practice Incentive Program (PIP), and GPs providing MBS assessment items must be linked to the practice approved for PIP.
The new incentives for GPs to administer the vaccine come in the same week Prime Minister Morrison
downplayed the suggestion of cash payments to individuals for receiving the vaccine.
‘Financial incentives are likely to discourage vaccination, particularly amongst those who are concerned about adverse effects,’ he said during question time on Tuesday.
‘Those 80% of older Australians who have turned up and rolled up their sleeves, they didn’t need the cash. They just needed to know that it was good for them, it was good for their family, it was good for their community and it was good for their country.’
But speaking on Wednesday, the head of Australia’s COVID Vaccine Strategy, Lieutenant General John Frewen,
said the Government incentives are being considered but are currently not needed because ‘Australians are coming forward’.
‘Demand is still exceeding supply right now, so the time for incentives I think may be later in the year when we’re getting into some of the more hesitant sort of groups,’ he said.
‘We will look at all of the sorts of positive alternatives. There is cash, there is the idea of lotteries, all these things are being discussed.
‘Getting vaccinated is the right thing to do, it’s the right thing for individuals and it is the right thing for our nation.’
Log in below to join the conversation.
aged care COVID-19 disability Practice Incentive Program vaccine rollout
newsGP weekly poll
Would it affect your prescribing if proven obesity management medications were added to the PBS?