Feature
Is telehealth a lifeline for isolated patients?
Telehealth has been a boon for housebound patients and many GPs – but others say nothing can replace face-to-face consultations.
 Telehealth has been well received by most, but it cannot always meet the needs of some patient groups.
Telehealth has been well received by most, but it cannot always meet the needs of some patient groups.
Ricky Buchanan has been virtually bedbound due to chronic illness for the past 20 years.
She released a report two years ago into the medical access issues facing people like her, who are homebound or bedridden.
‘We can’t have a whole section of society who are unable to access medical care. We have to fix it,’ she said at the time.
With low funding for home visits, many GPs find it impossible to juggle busy waiting rooms and the needs of homebound people, while access to other specialists has also been difficult.
Remarkably, much of what Ms Buchanan called for in 2018 has now come to pass, with telehealth becoming universal from late March in a bid to keep GPs and patients safe from the coronavirus.
‘I would never in a million years wish for a pandemic, but I have benefitted in many ways. It’s a very strange feeling,’ Ms Buchanan told newsGP.
‘Many things I’ve been wishing for over 20 years just fell in my lap.
‘Usually, in advocacy, it progresses inches by inches and each inch is hard-fought. I really hope a lot of these things stay, even after able-bodied people don’t need them anymore.’
Ms Buchanan is not alone.
More than 80% of people recently surveyed by the Consumers Health Forum (CHF) believe telehealth is either excellent or very good.
‘[Telehealth offers] considerable medical and social benefits for the many patients who may need to consult a doctor but do not require physical examination,’ CHF Chief Executive Leanne Wells said.
‘While the telehealth survey was of modest size [95 people], the overwhelmingly favourable response indicates strong community support for the scheme to continue in the post-COVID era.’
Federal Health Minister Greg Hunt has already flagged his support for widespread telehealth to continue even after the pandemic ends.
For Ms Buchanan, the telehealth experience has been entirely positive.
‘For my conditions, it’s worked really well and I haven’t found any downsides,’ she said.
‘My general experience with chronic illness is that, most of the time, they don’t need to touch you. If blood tests are needed, home pathology can come. I feel like I’m 85% of the way to having access, just by talking on the phone.
‘Now I’m able to speak to my GP on the phone instead of having her come down here [for a home visit]. It’s just amazing.
‘Instead of feeling super guilty, because I know she’s losing money, I can make an appointment online and just mark it as telehealth. It’s better for her and better for me.
‘People like me who can’t go to medical appointments and can’t get medical care have found telehealth really helpful. It’s a much bigger group than we think it is – especially if we include those who can only leave the house once a month, and a lot of frail elderly people would be in that category.’
People in this group – which also includes those with chronic pain or autoimmune conditions – have also benefitted, according to Ms Buchanan.
‘They can leave [the house], but they’ll spend days recovering. So they usually only leave for medical visits,’ she said. ‘Now they can save their energy.
‘Several have told me it’s revelatory – now they can save their energy for what makes them happy, like visiting people or doing shopping they can’t do online.’
Ms Buchanan has seen her GP repeatedly through telehealth, and has been able to more easily see her cardiologist and hepatologist.
‘I’ve needed to see both those specialists for a long time, but I’ve had to put them off because there was no way of talking to anyone,’ she said.
‘Because of this horrific pandemic, so many things have happened to me that are really good. So many things are now available to me – not just telehealth, but museums and concerts.
‘I could listen to the Melbourne Symphony Orchestra live for the first time in 20 years.
‘I just hope a lot of those things stay around. I would be bereft if I got to experience all this and then it was taken away.’
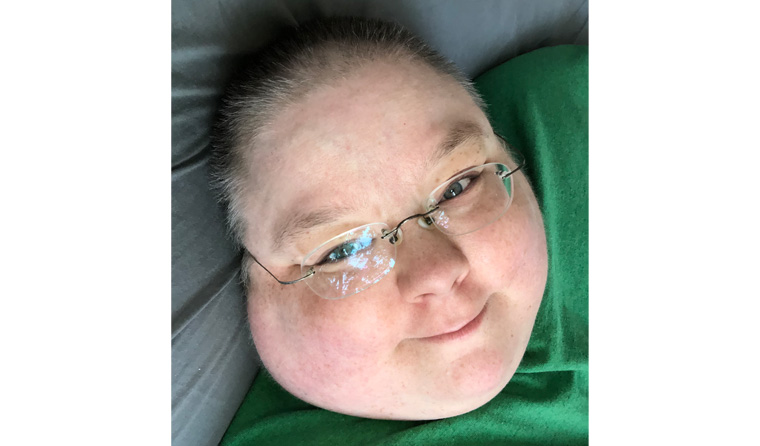
Telehealth has allowed Ricky Buchanan – who has been virtually bedbound for 20 years – to not only see her GP regularly, but also more easily see her cardiologist and hepatologist.
GPs, too, say telehealth is broadly beneficial for isolated groups.
Adelaide GP Dr Danny Byrne last year reluctantly gave up his home visits after 28 years following changes to bulk-billing incentives.
But telehealth has made it possible for him to see his homebound and frail patients remotely, checking in once a month, while practice nurses undertake care plans over the phone.
‘Instead of waiting for a crisis of some sort and doing home visits because you have to, now you can do preventive regular phone calls,’ he told newsGP.
‘It’s been great and patients are loving it. Usually, their daughter takes a day off work, or there’s a wheelchair and a carer involved.’
Melbourne GP Dr Floyd Gomez started Mobile GP to help isolated people get access to a regular GP. He told newsGP the telehealth rollout is a ‘perfect time’ to extend care to hard-to-reach groups.
‘These people were often never able to come to the clinic. What we could extract from this [situation] is the reintroduction of a regular GP into their lives,’ he said.
Brisbane GP Dr Wendy Burton said that for many patients – and GPs – universal telehealth is a boon. But it could be a negative for specific groups, such as people with mental health disorders who benefit most from face-to-face contact.
‘Overall, I’ve been loving having the telehealth option and the flexibility it gives to patients and me,’ Dr Burton said.
‘By and large, it’s a good process that I highly appreciate and hope it will continue. We’ve always been able to call patients, but now we can make it formal and part of our notes. Plus, whatever gets funded gets done, so it’s easier to allocate time to do that.’
Telehealth has made access to care easier for many of Dr Burton’s patients, avoiding the need to take time off work, travel to the clinic and sit in the waiting room.
Dr Burton recently saw an unwell child via video call. The child was sick enough to warrant a face-to-face consultation, after which Dr Burton was able to check in again with his mother the next morning, with another face-to-face follow-up to check he was improving later that week.
‘The convenience factor was just enormous. It meant his mum didn’t have to come in with a toddler and sick child,’ Dr Burton said.
But others have had less satisfying experiences.
For one of Dr Burton’s patients, a young man with a mental health disorder, telehealth simply wasn’t up to the task.
‘We had been doing telehealth but it wasn’t satisfactory. You can’t read the angst, the body language, the posture. You can’t tell if they’re avoiding your gaze,’ she said.
‘In my consulting room, it’s easier to interpret what’s going on.’
Telehealth has failed to deliver for Hope Gordon, who lives with complex PTSD.
Wrestling with spotty connections, data caps, and software compatibility issues leaves her feeling ‘exhausted, as though I have run to the hospital and back’, she writes on her blog.
She told newsGP the central issue is the gulf between her and her GP.
‘I hate technology. It feels artificial, like a TV. I can’t relate to it,’ she said. ‘I don’t know how people can conduct counselling through telehealth.
‘Trying to connect to people is just impossible. You really need face-to-face in the same space.
‘For me personally, with the frustrations of battery drain, the small picture – I hate the thing.’
But Ms Gordon said her experience may not be universal.
‘This is from the perspective of someone with complex PTSD. I can see the benefit overall, for the elderly who can’t get out,’ she said.
‘It makes healthcare more accessible for certain groups.’
Log in below to join the conversation.
coronavirus COVID-19 telehealth
newsGP weekly poll
Are you interested in prescribing ADHD medication?