Feature
The good, the bad and the dangerous: Advising on healthcare apps
How can GPs and patients distinguish the helpful from the useless – or even harmful – among the ever-increasing flood of healthcare apps?
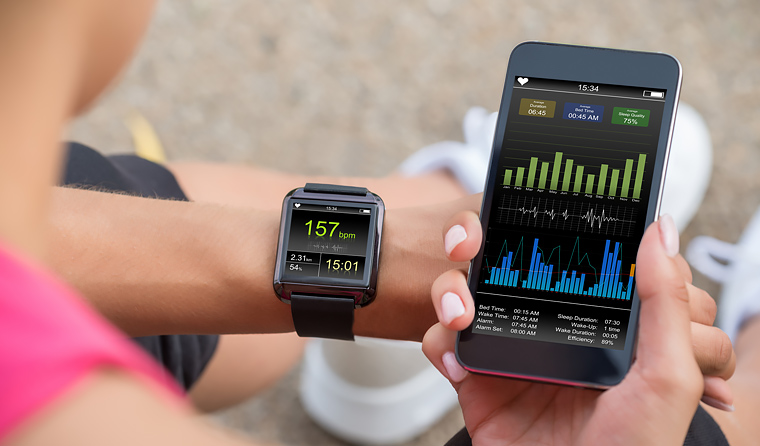 The bewildering array of healthcare apps available can make it difficult for GPs to provide patients with quality advice in this area.
The bewildering array of healthcare apps available can make it difficult for GPs to provide patients with quality advice in this area.
It has been estimated that there will be six billion smartphones in circulation throughout the world by 2020.
These increasingly powerful and increasingly available devices have connected people with instant communication, a vast repository of knowledge and a huge library of apps to help with any task, from getting meals delivered to your house to hunting ghosts.
There are also a growing number of apps designed to assist with healthcare. Some of these are genuinely helpful and could potentially even save lives.
But for every ‘good’ app, there are many, many more that are useless at best, harmful at worst.
Dr Steven Kaye, a GP and member of the RACGP Expert Committee – Practice Technology and Management (REC–PTM), explains why the information and advice provided by healthcare apps may not always be trustworthy.
‘Information and data gets collected by a consumer or patient and supplied in some way within an app,’ he told newsGP. ‘This process is inherently unreliable, given personal bias and lack of equipment calibration.
‘The data is then analysed within the app and recommendations and advice given. A lack of context and perspective combined with potentially invalid or incorrect information could lead to substandard advice.
‘Even if correct data is entered, variable quality advice might be generated by unknown app sources.’
It may seem as though advising patients on apps is a task outside of a GP’s remit. However, with thousands of healthcare apps available at the touch of a fingertip, discussions about them may become unavoidable in consultation rooms.
How can GPs stay informed and up-to-date about what apps are worthwhile?
‘The app environment moves very quickly; there are many developments in very short periods of time,’ Dr Kaye said. ‘But like all sources of information, the origin and validity [of apps] needs to be checked and verified.’
Regulation and assessment of apps by a central body could be of assistance to GPs and patients. Some of this regulation currently falls under the jurisdiction of the Therapeutic Goods Administration (TGA) if the apps are classified medical devices.
However, a recent paper published in the Medical Journal of Australia about glycaemic control apps for patients with diabetes is critical of the existing system, in which some apps are able to escape independent assessment by ensuring they are categorised as ‘low-risk’ devices even though they may perform the same function as others categorised at a higher level.
The TGA is currently reviewing its medical device registration framework with a view to bringing it in line with new rules introduced by European regulators. Dr Kaye believes this would be very helpful for GPs, although he also sees a potential role for other professional bodies.
‘GPs will tend to rely on proven technology from reputable sources,’ he said.
‘Endorsement from a peak body like the RACGP or reputable other source would also enhance the user confidence of these products.’
Dr Kaye also believes that an overarching system for apps in which they are required to meet a universal set of standards might be more practical. But however app regulation is implemented in the future, he feels GP involvement is essential.
‘Further scoping and planning will be needed, but we hope that a sustainable analysis and discussion process can be created,’ he said.
ehealth healthcare apps medical technology TGA Therapeutic Goods Administration
newsGP weekly poll
Health practitioners found guilty of sexual misconduct will soon have the finding permanently recorded on their public register record. Do you support this change?