News
Concerns grow over global PPE supply chains
Doctors have raised concerns over access to personal protective equipment as the Australian Government searches for alternate suppliers amid the ongoing coronavirus outbreak.
 Stockpiles of PPE, such as masks, are already being rationed in Australia.
Stockpiles of PPE, such as masks, are already being rationed in Australia.
As China continues its battle to contain the massive coronavirus outbreak within its borders, concern is rising over the effect its mass lockdown of half-a-billion citizens will have on global supply chains.
Recent efforts to kick-start the economy have been compounded by secondary outbreaks in South Korea and Japan, leading to worries over the ability of governments to secure crucial medical supplies, including personal protective equipment (PPE).
The US Department of Health and Human Services has already requested US$2.5 billion (AU$3.81 billion) to ‘support the acquisition of [PPE], especially masks’, as well as other vital medical goods, while hospitals in the UK have been warned against stockpiling masks amid fears of a shortage in supply.
Australian Federal Health Minister Greg Hunt also said this week’s activation of Australia’s COVID-19 Pandemic Plan included efforts to secure supply chains for necessities such as medical supplies and personnel.
‘What this does is, it now moves to a full preparation phase for all of the supply chains, the medicines, we’re working on the national inventories, [and] the national medical stockpile,’ he said.
State and territory health ministers have also been asked to demonstrate preparations they have made with regard to the supply of medical items such as masks and medicines, as well as ensuring there is a ‘surge capacity’ in hospitals.
However, AMA WA President and anaesthetist Dr Andrew Miller, who has a background in general practice, told newsGP he has concerns over future access to PPE and pointed out that WA Health is not assisting GPs who are unable to secure equipment through traditional methods.
‘We have to have a bit of a think about what we’re going to do in that environment [possibly running out of PPE], and how long we can delay this thing getting into the community,’ he said.
‘The point that the chief health officers are making at the moment is that they’d love to be able to help, but pretty much nobody’s going to have any once this thing hits because we’re not getting any more out of China and we’re using our usual stock in “business as usual” activity at the moment.’
Western Australia Chief Health Officer Dr Andy Robertson confirmed WA Health is not currently supplying GPs with PPE to treat suspected coronavirus cases, despite directing the public to general practices for testing.
‘PPE supplies for GPs are coming from the Commonwealth Government and being distributed by the WA Primary Health Alliance [WAPHA],’ he told newsGP.
‘Given the current low risk of COVID-19 transmission in Australia, with no known community spread, there is very limited benefit in distributing PPE, which is in limited supply both within Australia and internationally.
‘Should this situation change, however, we will look at what PPE equipment is required.’
RACGP President Dr Harry Nespolon has also called for more communication and support from governments, telling the ABC GPs urgently need more PPE in order to safely assess people who might have coronavirus.
‘If there’s going to be up to 40% of Australians affected by coronavirus, giving each surgery a few masks is not going to work,’ he said. ‘We don’t want a large number of GPs to get sick.
‘We need to know what practical role the Government wants GPs to play and to have that role properly resourced.
‘These practical measures [need to be] set up now, rather than waiting until there is a pandemic.’
Dr Miller said it is frustrating that it appears GPs are not being supported by state governments, even though they are being relied on to take the pressure off already overcrowded public hospitals.
‘It’s all very well for them to say, “You need to go and see your GP in these circumstances so you don’t flood the emergency department”, but then they throw their hands in the air and say, “But we can’t share any of our equipment with you, even if we’ve got it”,’ he said.
‘Partly what I’m trying to do is break down some of these silos and say, “Look, this isn’t a normal bureaucratic situation, where you apply normal bureaucracy”. We have to get the right gear to the right people in areas of need.’
Dr Miller did concede, however, that the situation is not unique to WA or even Australia, with global shortages likely to be an issue to the point where local healthcare workers may need to improvise their own PPE.
‘It is a big problem. What we need is a bit of discussion about what the alternatives to traditional masks and so on are going to be; what can we actually put into practice that might be of some help, even though we know it’s not going to be of great use for most people,’ he said.
‘We saw in China people wearing the office water bottles cut off on their heads and, whilst that seems a bit ridiculous, at least it stops droplet spray in the face.
‘Hopefully the border containment policies mean that we get at least a slow outbreak here. But if we get big numbers then at the moment ... that’s going to be the only option.’
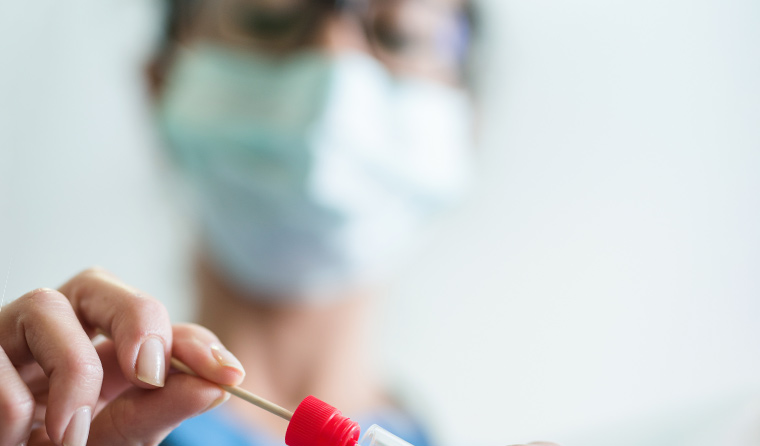
Collecting respiratory specimens, such as nasopharyngeal or oropharyngeal swabs, is a ‘low-risk procedure’ and can be performed using contact and droplet precautions, including surgical masks.
An Australian Department of Health (DoH) spokesperson did not say how many surgical or N95/P2 masks remain in the Government’s emergency stockpile, nor what percentage of PPE was sourced from China, but they did confirm to newsGP no PPE is currently produced domestically.
‘Quantities of products in the stockpile are provided on a need-to-know basis and not publicly available. Stocks are being purchased and a national stocktake underway,’ the spokesperson said.
‘The Commonwealth sources PPE from an in-country supplier who sources product from a number of overseas manufacturers. There are a number of [other] in-country suppliers, all of whom rely on overseas manufacturers.
‘As part of the contingency measures, Government is looking to alternative suppliers to build the NMS [national mask stockpile] capability and capacity.’
While the DoH would not reveal the number of masks in its stockpile, The New Daily reported on 12 February that the Government had 12 million P2 masks on hand, along with nearly 7.2 million surgical masks.
Associate Professor Mark Morgan, Chair of the RACGP Expert Committee – Quality Care (REC–QC), told newsGP he can understand the need to properly organise distribution of a limited resource and said he hopes it would be made available ‘on a needs basis, not on the ability-to-pay basis’.
However, he warned that improvised PPE could have serious consequences, as coronavirus spreading among healthcare workers, especially early in an outbreak, has the potential to be devastating.
‘There would be a real problem of knowing what PPE is effective, particularly if you’re home-making PPE, [and] whether [or not] it’s actually creating a false sense of security,’ he said.
‘If you start losing healthcare workforce early on in a pandemic spread … you lose the capacity to provide primary care and patients flood into already overstretched hospital sites.
‘Secondly, healthcare workers tend to come in contact early on in the course of a disease spreading to the community, because people come and see us, and then we’re likely to become a source of spread of infection to patients because we see a lot of people.’
Associate Professor Morgan said there is a major need to support GPs properly, as they are ‘central’ to any public health response to a pandemic.
‘People are going to be scared and many will be sick if this takes root, and GPs are the large, willing workforce with the skills to manage that. Supporting GPs to do that safely is vital,’ he said.
‘We should be thinking seriously about the availability of masks to the general public and whether it’s sensible, if supplies are going to be really constrained, to have things for sale in supermarkets and hardware stores that might become really sought after and essential products for protecting key workers to keep society running.
‘[If we ran out] the advice would have to be, “We can’t safely see people that fulfil those criteria and they need to go to a better resourced site”, which I think is a ludicrous waste of a willing and well-trained resource in general practice.’
The RACGP has more information on coronavirus available on its website.
Log in below to join the conversation.
coronavirus COVID-19 pandemic personal protective equipment PPE
newsGP weekly poll
Health practitioners found guilty of sexual misconduct will soon have the finding permanently recorded on their public register record. Do you support this change?