News
Confusion over updated coronavirus mask advice
Some authorities say surgical masks are safe to use for swabs in ‘mild cases’, but that appears to contradict other recommendations.
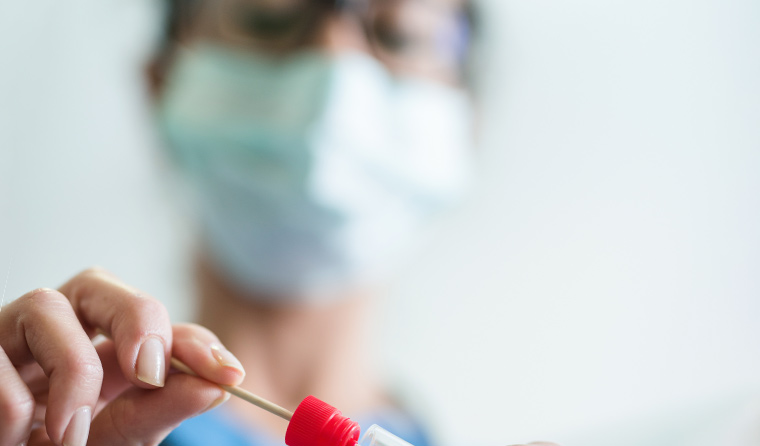 Collecting respiratory specimens, such as nasopharyngeal or oropharyngeal swabs, is a ‘low-risk procedure’ and can be performed using contact and droplet precautions, including surgical masks.
Collecting respiratory specimens, such as nasopharyngeal or oropharyngeal swabs, is a ‘low-risk procedure’ and can be performed using contact and droplet precautions, including surgical masks.
newsGP understands the guidelines, which first appeared on the NSW Health and Victorian Department of Health and Human Services (DHHS) websites, will soon be adopted nationwide following recommendations from the Infection Control Advisory Group (ICAG).
The Communicable Diseases Network Australia (CDNA) coronavirus guidelines have been updated to reflect the new position, but at the time of publication the Australian Department of Health (DoH) was still recommending more stringent personal protection measures.
The DoH advice states airborne protections, including a P2 or N95 respirator, ‘must … be used while collecting specimens’.
The RACGP has been clear in its recommendation that GPs adhere to DoH advice and use a P2 or N95 respirator when collecting coronavirus samples.
ICAG Chair Professor Lyn Gilbert told newsGP the new surgical mask recommendations are based on existing definitions of aerosol-generating procedures, which had been temporarily superseded by a more conservative approach given uncertainty surrounding the virus.
‘[The new guidelines] are different from what has been recommended previously in some jurisdictions, which were based on a highly precautionary response,’ she said. ‘However, the evidence supports contact and droplet precautions [such as] surgical masks, except for aerosol-generating procedures.
‘In the past, the collection of upper-respiratory specimens such as nasopharyngeal or throat swabs has never been regarded as an aerosol-generating procedure.’
However, the Victorian DHHS and NSW Health are also still recommending the collection of a lower-respiratory specimen – sputum – which under the existing DoH guidelines and CDNA recommendations would require an aerosol-generating procedure and thus the use of a P2 or N95 respirator.
A NSW Health spokesperson told newsGP the collection of respiratory specimens, such as nasopharyngeal or oropharyngeal swabs, is a ‘low-risk procedure’ and can be performed using contact and droplet precautions, including surgical masks, for most patients with mild illness.
‘If the patient has severe symptoms suggestive of pneumonia – for example, fever and breathing difficulty, or frequent, severe or productive coughing episodes – then contact and airborne precautions should be observed,’ the spokesperson said.
‘We understand that the Australian Department of Health is updating its fact sheets in line with this advice.’
Associate Professor Mark Morgan, Chair of the RACGP Expert Committee – Quality Care (REC–QC), told newsGP questions remain over the source of the information, how it has been disseminated, and whether it is based on evidence that has been gathered overseas.
‘It would give GPs much more confidence if, in addition to the fact sheets, there was reference information for those who want to dig into it and understand where the advice comes from,’ he said.
‘Is there a science behind this based on the measurement of viral shedding or information that’s been gathered from the experience in China and other countries, or is this just some expert opinion that could be changed again in light of health workers being infected by taking the lesser level of precaution?
‘If we start infecting the healthcare population, then our ability to manage the next phase of the pandemic will be deeply impaired.’
Associate Professor Morgan said that while the overall response to date appears to have been successful insofar as there has been no human-to-human transmission in Australia, the management and dissemination of information could be improved.
‘It’s almost as if the information about Australia’s planning remains a secret to be trickled out on a daily basis after the meeting of the communicable disease committee,’ he said.
‘People would have more confidence if the information all changed at the same time, was disseminated from the same source, and if we knew on what basis the information was changing.
‘It would be nice to understand the shape of future responses, not just today’s response.’
The updated surgical mask guidelines were released around the same time the World Health Organization
confirmed the coronavirus-related death of Dr Li Wenliang, a 34-year-old ophthalmologist in China who was the first to raise the alarm over the outbreak and later arrested by Chinese police.
At least
14 healthcare workers in China have been infected with coronavirus, according to figures most recently updated on 20 January.
Professor Gilbert said she is ‘hopeful’ finalised infection control guidelines and fact sheets, which have also been approved by the Australia Health Protection Principal Committee (AHPPC), will be on health department websites soon. She also stressed the ICAG is still taking a precautionary approach to more serious cases.
‘Airborne precautions for the collection of specimens from the minority of patients who have evidence of lower-respiratory infection or pneumonia … [and] in the GP’s clinical judgement are likely to require admission to hospital irrespective of nCoV-2019 PCR [novel coronavirus 2019 polymerase chain reaction] result [remain the same],’ she said.
‘In these sick patients, we recommend use of P2 or N95 respirators for the collection of specimens on the assumption that it may generate aerosols.
‘This also means that P2 and N95 respirators must be used correctly, must be fit-tested, otherwise they will not be effective. It also means that the specimen should be collected in a negative-pressure room or a room that can be left vacant for at least 30 minutes afterwards.
‘It is recognised that most GPs are unlikely to be able to meet these criteria for airborne precautions and therefore the recommendation is that these patients be referred to hospital.’
The new advice is the latest in a
string of updates that have been issued by various health departments across Australia, which GPs have
said are inconsistent and seem to
lack coordination.
GPs have also
had difficulties accessing masks following confusion over what masks were being issued. In recent information obtained from the DoH, it has been confirmed only surgical masks are being distributed by the Federal Government via Primary Health Networks after
lobbying from RACGP President Dr Harry Nespolon.
Some state governments are distributing surgical and P2/N95 masks.
At the time of publication, Australia had 15 confirmed coronavirus cases across Queensland, NSW, Victoria and South Australia. There have been more than 31,000 confirmed cases
worldwide and at least 638 fatalities.
The RACGP has more information on coronavirus available on its website.
Log in below to join the conversation.
coronavirus infectious disease masks public health
newsGP weekly poll
Health practitioners found guilty of sexual misconduct will soon have the finding permanently recorded on their public register record. Do you support this change?