News
Is it ethical to infect humans with SARS-CoV-2?
A proposed UK vaccine trial that will infect healthy volunteers has raised concern among Australian experts who fear long-term health ramifications.
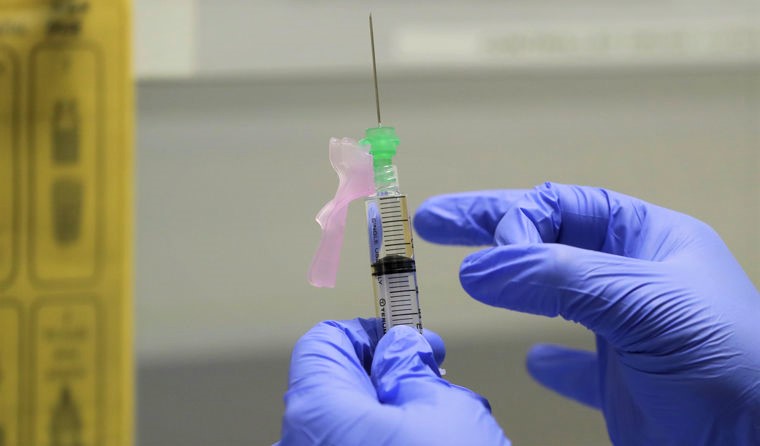 The proposed trial would see healthy volunteers aged 18–30 infected with SARS-CoV-2 – but experts are apprehensive. (Image: AAP)
The proposed trial would see healthy volunteers aged 18–30 infected with SARS-CoV-2 – but experts are apprehensive. (Image: AAP)
Would you volunteer to be infected with a potentially fatal virus? A virus that has killed more than one million people and led to government-enforced lockdowns across the globe?
Scientists at the Imperial College London are hoping people will do exactly that.
The UK Government’s COVID-19 Vaccine Taskforce has agreed to pay Open Orphan, a Dublin-based commercial clinical-research organisation, up to £10 million to conduct the UK COVID Challenge study.
With the necessary ethics approval, the initial trial would see 30–50 healthy volunteers aged 18–30 infected with SARS-CoV-2. If the majority are not infected, the team will seek permission to administer higher doses until most volunteers have been exposed to the virus, in a bid to test vaccine efficacy.
An investigator on the study, immunologist Professor Peter Openshaw, said the trial has the potential speed up understanding of the coronavirus to develop an effective vaccine, as well as treatments.
‘Deliberately infecting volunteers with a known human pathogen is never undertaken lightly. However, such studies are enormously informative about a disease,’ he said.
‘It is really vital that we move as fast as possible towards getting effective vaccines and other treatments for COVID-19, and challenge studies have the potential to accelerate and de-risk the development of novel drugs and vaccines.’
Of course, this is not the first human challenge trial, a number of which have been conducted for influenza and seasonal coronaviruses.
An early model of such a study is the Common Cold Unit. Based in the UK from 1946–89, volunteers would be infected with coronaviruses and housed in small groups, isolated from others in the community.
Associate Professor Ian Mackay, a clinical virologist at the Australian Infections Diseases Research Centre at the University of Queensland, says such trials in controlled environments can have many benefits.
‘Those studies in the UK back then were really important,’ he told newsGP.
‘In that process, we learned a heck of a lot about respiratory viruses, about surfaces, about how much mucus was produced, how the mental impact of a cold could affect people’s productivity, all sorts of things.
‘I see this as being similar to that in that we can learn a lot of things like how much virus is required to start off an infection.’
That is not to say, however, that the virologist does not have concerns.
‘We still haven’t quantified what drives this outcome called “long COVID”,’ Associate Professor Mackay said.
‘We do know that this virus spreads around the entire body, that for a period of time it’s detectable in the blood, which means it can get to any tissue and it does seem to get to just about every tissue.
‘There are publications and anecdotes linking to neurological issues, cardiac issues. These are all serious outcomes, and some of these may not be immediately apparent, but may be a problem for life, going on after the infection.’

Associate Professor Ian Mackay says human challenge trials can provide important insights into the coronavirus, with potential to speed up vaccine development.
Professor Raina MacIntyre has similar fears.
An expert in influenza and emerging infectious diseases, and Head of the Biosecurity Program at the Kirby Institute at UNSW Sydney, she says although volunteers will be screened for any known risk factors, severe COVID cannot be ruled out.
‘I think it is highly unethical and dangerous,’ Professor MacIntyre told newsGP.
‘When an infection is serious and potentially lethal, volunteers [are] at risk, even if young and healthy. We do not yet know the infectious dose of SARS-CoV-2, so if they are given a high exposure dose, it could be fatal, even in young people.’
Infectious diseases specialist Associate Professor Sanjaya Senanayake agrees.
Though older people have been disproportionately affected by SARS-CoV-2, he is hesitant to rule out the impacts on other cohorts.
‘The issue for me is that we are still learning about COVID, there are lots of unknowns. While a lot of healthy young people seem to not get a severe illness requiring hospitalisation, there are those who do, there are those who die, who may have risk factors that we’ve yet to appreciate,’ Professor Senanayake told newsGP.
‘Even those people who aren’t admitted to hospital and who have a mild illness at home, as a proportion, will go on to develop more chronic symptoms as well. That’s the issue with COVID.’
Professor Sarah Palmer, Co-Director of the Centre for Virus Research at the Westmead Institute for Medical Research, says the trial is unlikely to give insight into the effects of the virus on the most vulnerable cohorts.
‘They are proposing to enrol people who are young, so [the] majority would probably have a mild infection. But then it would not really give us any information or would not be useful for learning anything about people who are elderly and most at risk for a severe infection,’ she told newsGP.
‘So it wouldn’t really be a very good model for setting the response to this virus and people who have a more severe response to this infection.
‘Maybe the one bright spot that you could learn from such a human trial would be, how often does reinfection happen if you follow the trial participants? You can learn, how long does immunity last? If you’ve been exposed to the seasonal coronaviruses, does that give you some protection against SARS-CoV-2?’
If the trial gets the green light, it has been reported that volunteers who test positive would be treated with an antiviral, suggested to be remdesivir.
But given the drug was shown to have no effect on mortality or illness duration in the World Health Organization (WHO) Solidarity trial, experts say such a treatment is inadequate.
‘With a lot of these challenge trials, there’s often a rescue therapy in place. So if someone gets really sick, you can give them a particular medication and they’re okay,’ Associate Professor Senanayake said.
‘But we really haven’t got an effective medication for COVID that we can definitively say [works], except for dexamethasone in patients who are very unwell in hospital.’

Influenza and emerging infectious diseases expert Professor Raina MacIntyre has branded the proposed trial as ‘highly unethical and dangerous’.
Alarm over potential ethical concerns has also been raised.
While it has yet to be confirmed whether there will be financial incentive for volunteers, Nature reported that Open Orphan typically pays volunteers around £4000 for their trial.
Professor Palmer fears financial incentive result could result in volunteers overlooking possible risks.
‘If this is a trial that they offer funds to people to enrol, they may get people who are in a low socioeconomic class who maybe require funds or are doing it for the funds,’ she said.
‘And these could be people who’d be actually more at risk for a more severe response to the virus.’
Experts agree the study could speed up the process of finding answers about vaccine efficacy. But given the high rates of community transmission, Professor MacIntyre thinks advancing to a human challenge trial is unnecessary.
‘With massive surges of COVID-19 in the UK and Europe right now, you could do a normal RCT [randomised controlled trial] and have enough power because there is so much disease around,’ she said.
‘That actually is a strong argument against this.’
Associate Professor Mackay argues, however, that a controlled study environment would provide greater insight that ‘you simply can’t get out in the wild’. But with 48 vaccines currently in clinical trials around the world, 11 of which are in phase three trials, Professor Palmer thinks it is too early in the pandemic to start infecting people.
‘We have so many vaccines right now that are in phase three trials, why not wait for those to become available and to see what happens?’ she said.
‘Maybe it has to do with people getting desperate and thinking, well, we’re having to lockdown and our GDP is dropping. But I just don’t think we’re that desperate yet.’
There is no denying experts can see benefit in human challenge trials. But when asked if they would sign up, the general consensus is loud and clear.
‘To us who aren’t part of the trial, that’s true, [there are benefits],’ Associate Professor Senanayake said.
‘The question which I always ask myself is, would I want it? Would I want someone in my family to undergo a challenge trial? And, actually, the answer is no.
‘I do not want to get COVID unnecessarily. There’s still too many unknowns.’
Log in below to join the conversation.
COVID-19 human challenge trial vaccine
newsGP weekly poll
How often do patients ask you about weight-loss medications such as semaglutide or tirzepatide?