News
Another quarantine outbreak raises questions over airborne transmission
The newly-confirmed coronavirus case is a Melbourne hotel worker branded a ‘model employee’, who did not breach any infection control protocols. So how did he catch the virus?
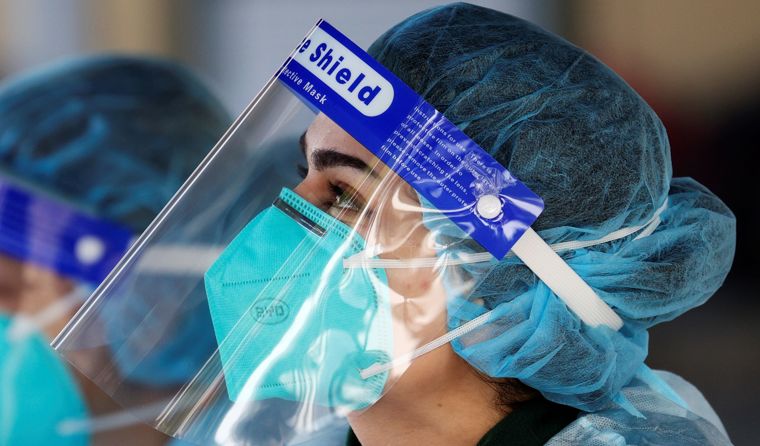
 Victorian healthcare workers at the Grand Hyatt hotel wearing PPE, including P2 respirators. (Image: AAP)
Victorian healthcare workers at the Grand Hyatt hotel wearing PPE, including P2 respirators. (Image: AAP)
Victorians were on edge on Wednesday night, as Premier Daniel Andrews announced the second outbreak from Australian hotel quarantine in the past five days – and third for 2021.
The confirmed coronavirus case, a 26-year-old resident support officer who had been working at the Grand Hyatt Hotel as part of the Australian Open quarantine program, brought the state’s 28-day streak of no community transmission to an end.
However, unlike the outbreak in Western Australia – where it was revealed the security guard had not been wearing a mask, despite working on a floor containing people infected with the highly contagious UK variant – Premier Andrews said the new case had followed all infection control precautions.
‘We have reviewed literally days of CCTV footage, and this person has been a model employee, whether it is donning PPE [personal protective equipment], all the protocols, all the other rules that are followed up,’ he said.
‘We can find no problem, no breach of protocol or anything of that nature in terms of his employment.’
As per recently updated protocols, the worker undertook a routine test at the end of his shift on 29 January, but despite returning a negative result, he went on develop symptoms and tested positive on 3 February.
The man had been working on the same hotel floor as two groups of travellers who had tested positive to the highly infectious UK variant of the virus. Yet Premier Andrews said authorities do not know how the worker actually contracted the virus, with the case once again reigniting the debate around airborne transmission.
‘One of the things we can’t rule out is that there’s aerosol transmission, so airborne transmission,’ Premier Andrews said on Thursday.
‘I know the AHPPC [Australian Health Protection Principal Committee] has been dealing with some of these issues and no doubt this will be a feature of the report I give National Cabinet tomorrow.’
Leading occupational hygienist Kate Cole says she has no doubt that aerosol transmission had a role to play, and that it reaffirms the need for a national approach to infection control.
‘Unfortunately, it’s not surprising that this has happened given the low amount of focus put on airborne transmission by the various guidelines across Australia,’ she told newsGP.
‘States and territories refer back to federal guidance to help them make informed decisions and, unfortunately, our federal guidance from ICEG [Infection Control Experts Group] and other bodies hasn’t kept pace with the evolving science on this issue.’
Following the 13 January case in Brisbane’s hotel quarantine that led to a three-day lockdown, ICEG Chair Professor Lyn Gilbert told the ABC the group would update its advice.
But close to three weeks and two hotel quarantine cases later, advice around airborne transmission in the Communicable Diseases Network Australia (CDNA) National Guidelines has not changed.
ICEG member and infectious disease specialist Professor Peter Collignon told newsGP he could not comment on the guidelines, but said he has yet to see convincing evidence on aerosol spread.
‘Why wouldn’t you think it would be through touching surfaces as much as breathing it in?’ he told newsGP.
‘In Melbourne, at least as far as I’m aware, the room that the family of five were in was directly opposite the door from the other room where the lady got infected and … both doors were open at the one time on one occasion.
‘I can imagine it’s not more than two metres. So again, isn’t that more likely to be consistent with how we know this spreads – which is predominantly by droplets from infected people?
‘If it really is aerosols, you’d expect large numbers of people quite distant from the source to get infected, and that’s not what's happening; we’re seeing single cases.’
However, Professor Collignon has previously acknowledged that airborne transmission can occur, telling the ABC that a Brisbane cleaner who contracted COVID last month could have gotten it as a result of a ‘rare aerosol event’.
‘[Aerosol transmission] undoubtedly does occur. And nobody said it doesn’t. But in the proper perspective of the total spread of this, it seems to be mainly close proximity and droplets and being associated with people that have got symptoms,’ he said.
‘People without symptoms can transmit it as well, but people who are coughing and sneezing and have symptoms are much more likely to transmit virus much further than somebody who is asymptomatic and maybe singing or shouting occasionally.’
Contradicting this theory is a study published last month in Proceedings of the Royal Society A, which found that when two people are in a poorly ventilated space and not wearing masks, prolonged talking is much more likely than a short cough to spread the virus.
While genomic sequencing has yet to confirm whether or not the Melbourne hotel worker has the UK variant, Professor Nigel McMillan, Program Director of Infectious Diseases and Immunology at the Menzies Health Institute Queensland, says it could provide more insight.
‘Since these new variants have come to our shores, we’ve now had three cases break out from three different states in terms of hotel quarantine,’ he told newsGP.
‘The idea being circulated right now is that there is a higher viral load. Now this is causing problems in the way quarantine systems are working because to have it happen in three independent places is obviously no accident.
‘In terms of the aerosol spread, this has been hotly debated. But perhaps we’ve pushed over a threshold here now, and we’ve just pushed that contact time and space to be a bit shorter where people only need to be a bit further away and still get it.’
ICEG member Professor Peter Collignon says more focus should be given to eye protection. (Image: AAP)
Ms Cole says the new variant has brought about more pressing need for aerosol spread to be recognised, but says it doesn’t negate that it should have been done ‘more than six months ago’.
‘We’ve seen, unfortunately, the learnings that we’ve had to go through in Victoria during that second wave, and the need to increase PPE for healthcare workers. We shouldn't need to wait for additional outbreaks or additional people to get COVID within the workplace, before we act,’ she said.
‘When you’ve got a hazard that’s airborne, then you can look at things like ventilation really, really closely, in addition to upgrading PPE to be respiratory protection – and when we say that, we mean N95, P2 respirators, not surgical masks.
‘Surgical masks don’t provide respiratory protection from airborne hazards.’
Professor Collignon agrees that ventilation is a key issue, and one where the guidance is lacking.
‘Ventilation is an issue because even if it’s droplets, for instance, if you’ve got poor ventilation, depending on the wind behind you, they may go further than a metre or two,’ he said.
‘The trouble with developing guidelines is they will be very difficult to write because if you’re doing evidence-based guidelines, you’ll find there’s very poor evidence for this.
‘So I think this is where we need more research.’
Despite the apparent lack of evidence, other countries and areas with similar health systems, such as Canada and the EU, have released their own guidance on ventilation. The World Health Organization (WHO) has also contributed to ventilation guidance that was released in May last year.
While Australia waits for advice on ventilation, Professor Collignon says more focus should be given to eye protection.
‘That’s the one thing that I think we don’t do very well from infection control,’ he said.
‘I’ve seen a lot of quarantine hotel photos where people are wearing surgical masks, which is fine, but they’re not wearing eye protection in the form of a face shield.
‘The eyes are as important as your nose and your mouth, so you do need a face shield on if you’re within two or three metres of somebody who’s likely to have an infection in my view.’

Victoria responded to a spate of coronavirus infections among healthcare workers last year by updating its personal protective equipment guidelines regarding the use of P2 masks.
Another argument that continues to resurface is that of moving quarantine programs out of metropolitan cities into remote settings.
While Professor MacMillan is not a proponent of the idea, he says he can see some benefit when it comes to ventilation and access to natural light.
‘When you are in a facility where all the rooms are separate, like huts and the like, when you open the door you’re into the outside and the sun is there – the sun is our best sterilant ever,’ he said.
‘UV light kills these viruses off pretty rapidly. There’s not much sunlight in hotel corridors.
‘But I’m not advocating it, purely because by the time we actually do it, our vaccines will have arrived, and it’s also more of a logistical issue.
‘My recommendation always would be for infected people to go into a negatively pressured infectious diseases ward. It’s not like those particular wards are overrun right now, and it certainly ensures that you have highly trained staff whose job is to look after infectious disease patients – all that training’s already done.’
Whatever direction authorities decide to take, Ms Cole says that as a precautionary approach, formally acknowledging the role of aerosol spread should be a non-negotiable.
‘Until we recognise airborne transmission, and until we put control measures in place, the message we’re sending is that we don’t care enough to provide safe workplaces and that outbreaks are inevitable,’ she said.
‘Our message should be we have strong borders, we have strong systems in place. Yes, it’s a safe place to quarantine, and yes, if you go to work in hotel quarantine, we will protect you.
‘But until we have national guidelines that recognise airborne transmission and recommend a precautionary approach with practical control measures, we’re going to still see these things happening and outbreaks in hotel quarantine will continue to occur.’
Log in below to join the conversation.
aerosols airborne transmission coronavirus COVID-19 hotel quarantine UK variant
newsGP weekly poll
As a GP, do you use any resources or visit a healthcare professional to support your own mental health and wellbeing?