Feature
Overcoming barriers to cervical screening: Self-collection
As Australia works towards eliminating cervical cancer, Dr Lara Roeske re-emphasises a pathway that can help reach under or never-screened women.
 Dr Lara Roeske is keen to re-emphasise the importance of offering the option of self-collection for under and never-screened women.
Dr Lara Roeske is keen to re-emphasise the importance of offering the option of self-collection for under and never-screened women.
There has been much positive news recently around cervical cancer, namely that a combination of human papillomavirus (HPV) vaccination and screening could see the disease eliminated in many countries by 2100 – and in Australia, perhaps even as early as 2035.
Dr Lara Roeske, GP and Director of Education and Liaison physician at VCS Pathology, is delighted by this news – but also acknowledges that barriers remain, even under the new five-yearly screening program, particularly among specific groups of women.
‘Our lowest participation [in cervical screening] occurs in rural and remote Australia, in areas of socio-economic disadvantage, amongst culturally and linguistically diverse groups of women, and also in Indigenous women,’ she told newsGP.
‘It is also important to consider women who have had a previous negative pap smear experience; women who are victims of sexual violence and trauma; older women; women who have been HPV-vaccinated and believe that they might not need to be screened.
‘And then women who may be involved in roles such as caring for young children or for older relatives, who are juggling work and family life, so are basically just too busy for their own self-care.
‘Women who are same-sex attracted and transgender men are also often particularly vulnerable and avoid screening.’
The same figures that show the effectiveness of the screening program also highlight the importance of trying to identify and include women who have been reluctant to take part in it.
‘We know that that up to 90% of invasive cervical cancer in Australia is diagnosed in women who are either under-screened or never-screened, and that these women remain at the highest risk of developing it,’ Dr Roeske said.
‘Six out of 10 Australian women have been shown to participate at the recommended interval, which means four out of 10 don’t … So it’s really important to identify eligible women in your practice.’
A screening pathway has been developed which can help to overcome the barriers to the process under or never-screened women experience – self-collection.
However, this pathway has experienced its own barriers, including the fact that until recently, there was only one laboratory within Australia accredited to process self-collected samples.
GPs’ have also held concerns about the accuracy of tests based on self-collected samples, but Dr Roeske says these barriers have been addressed, starting with the accreditation of a second laboratory, Douglass Hanly Moir Pathology.
‘VCS Pathology was the first laboratory in Australia to be accredited to process tests, and has now processed almost 3000 self-collects and accepts self-collected samples Australia-wide,’ she said.
‘The other laboratory is situated in Sydney, and can also accept self-collects from satellite sites.
‘So in terms of getting reliable test results for self-collected samples, and accessing a laboratory, there has been an improvement.’
Dr Roeske also wants to emphasise that the use of self-collected samples has a strong evidence-base, and that Australia is a world-leader in this area.
‘The self-collection pathway is a Medical Services Advisory Committee-endorsed pathway, it’s included in our national guidelines,’ she said.
‘In fact, Australia has pioneered self-collection, we are the first country in the world to endorse this as part of national guidelines.
‘So it’s a ground-breaking test and initiative.’
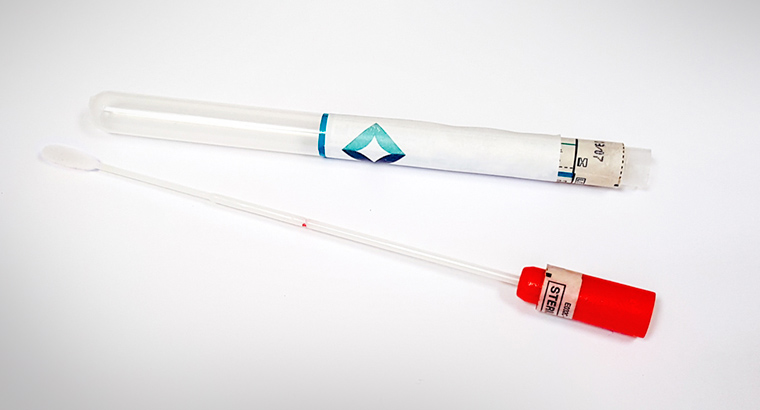 The Copan 552C dry-flocked swab is the only swab that has been validated for self-collection in the National Cervical Screening Program.
The Copan 552C dry-flocked swab is the only swab that has been validated for self-collection in the National Cervical Screening Program.
She is also keen to reassure GPs that the accuracy of tests using self-collected samples has been backed by research.
‘A recently published meta-analysis has demonstrated the effectiveness and accuracy of self-collection – so a self-collected sample is as accurate as a clinician or a GP-collected sample,’ Dr Roeske said.
‘So that’s great news – we don’t want GPs worrying about the accuracy of the test result.’
While a clinician or GP-collected sample is still preferred, the choice of self-collection offers a way to reach women who may be uncomfortable with this.
‘We always suggest a GP offers [the speculum exam] at the outset, so that’s the first option, a clinician-collected sample from the cervix,’ Dr Roeske said.
‘GPs will find that sometimes the conversation actually leads to a woman saying, “That’s fine, I’ll have the speculum exam and cervical screening”.
‘But should the woman refuse for whatever reason, or should she be identified as being under or never-screened and refuse, then as long as she’s over 30 and it’s been at least four years since her last cervical screening test result, you can offer and support her self-collect.’
While self-collected samples have shown accuracy in test results, Dr Roeske cautioned that this is reliant on ensuring the correct procedure is followed.
‘The self-collection needs to be done with a particular type of swab, known as the Copan 552C swab,’ she said.
‘The swab has a flocked end, so it looks a bit like a cotton bud, and the way it is wound ensures a maximal collection of vaginal cells to optimise accuracy.
‘Women need to be told where to insert the swab, and some aren’t familiar with their genital anatomy and might need particularly sensitive support and guidance around this: It should be inserted into the vagina, not more than a few centimetres, rotated once or twice and withdrawn, returned to the tube and then back to the GP or the nurse.’
Unlike other types of self-collected screening, such as the National Bowel Cancer Screening Program, cervical cancer samples can only be collected at a general practice, not in the home or at a laboratory.
‘That’s because it’s an opportunity for GPs to discuss the importance of screening and preventive health,’ Dr Roeske said.
‘It’s also an opportunity to explain how the test is done, and to support women. And very importantly, it’s so that women understand follow up requirements and negative and positive results.’
Overall, Dr Roeske wants to emphasise to her GP colleagues what a difference the self-collection option can make to individual women, and to rates of cervical cancer.
‘[VCS Pathology] modelled self-collection prior to the rollout of the renewed program, and we found that when eligible women were offered self-collection, 87.5% of them took up the option,’ Dr Roeske said.
‘But what was really significant was when follow up was required around positive results, over 90% adhered to it – a testament to the power of this pathway to re-engage women back into screening and reduce the risk of cervical cancer in this group that we know are more likely to develop cervical cancer than anyone else.’
Cervical cancer Cervical screening HPV vaccine screening Self-collection Women’s health
newsGP weekly poll
Which of the following areas are you more likely to discuss during a routine consultation?