News
‘There’s a lot of vaccine hesitancy out there’
Aboriginal and Torres Strait Islander health experts speak to newsGP about steps to address misinformation and hesitancy ahead of phase 1b.
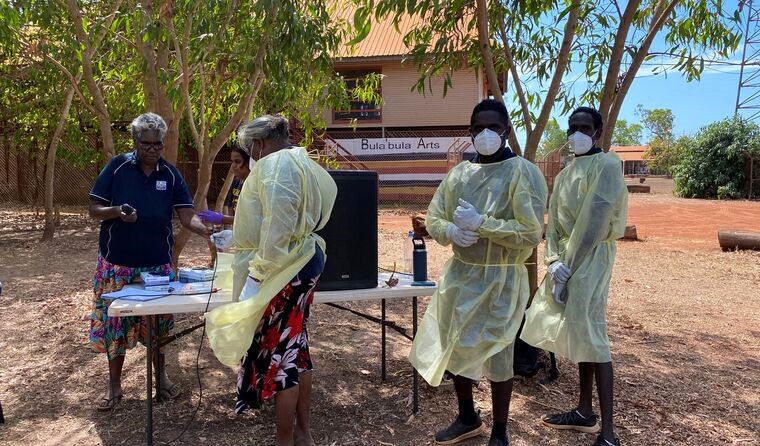 Willingness to receive the vaccine has decreased among Aboriginal and Torres Strait Islander people, a longitudinal study has shown. (Image: NACCHO)
Willingness to receive the vaccine has decreased among Aboriginal and Torres Strait Islander people, a longitudinal study has shown. (Image: NACCHO)
As Australia prepares to move into phase 1b of the coronavirus vaccine rollout, Aboriginal Community Controlled Health Organisations (ACCHOs) are buckling down on tackling vaccine hesitancy.
GP Dr Tanya Schramm is a Palawa woman and Chair of the Expert Committee behind the COVID-19 clinical recommendations for Aboriginal and Torres Strait Islander people.
She told newsGP misinformation has been rampant, and that social media has played a central role in its dissemination.
‘There’s been a huge social media campaign in general with … the anti-vax movement putting a lot of stuff out … and that has obviously just overflowed into our Aboriginal and Torres Strait Islander communities,’ Dr Schramm said.
‘The vaccine messages haven’t necessarily been consistent, and things are changing so rapidly. So people are becoming a bit unsure all of a sudden about vaccinations and their ability to trust the vaccine.’
When it comes to vaccine uptake in Australia, Aboriginal and Torres Strait Islander people are known to have higher uptake than non-Indigenous Australians. But a longitudinal study conducted in January by the Australian National University found Aboriginal and Torres Strait Islander people are also among those who have become less willing to receive the coronavirus vaccine.
Given the heightened risk posed by coronavirus to Aboriginal and Torres Strait Islander people, those aged 55 and over will be eligible to receive the vaccine under phase 1b, slated to commence next week.
Dr Schramm says the timeline itself also has a role to play in people’s apprehension.
‘We’re quite early in the vaccination process – for obvious reasons,’ she said.
‘But because we’re getting it earlier than say the general population, there’s concern that there may be … a problem with it.’
GP Dr Jason Agostino is the Medical Advisor at the National Aboriginal Community Controlled Health Organisation (NACCHO) and member of the Aboriginal and Torres Strait Islander Advisory Group on COVID-19.
He told newsGP that steps are being taken to address this concern.
‘There’s a lot of vaccine hesitancy out there, [but] I don’t think we have an anti-vax movement,’ Dr Agostino said.
‘What we have is hesitancy around this vaccine and a lot of misinformation going around to people [who have] reasonable questions that they want answered.
‘We’ve got a specific factsheet about vaccines for Aboriginal and Torres Strait Islander people talking about the experiences of other First Nations [people], and really clarifying that Aboriginal and Torres Strait Islander people aren’t guinea pigs here.
‘The reason that they’re priority populations is because Aboriginal and Torres Strait Islander health leaders have fought hard to make sure that they have access to vaccines early.’
Since the pandemic was declared in March 2020, ACCHOs have been at the forefront of efforts to keep the virus out of their communities.
To assist them in developing and promoting accurate and culturally appropriate messaging, the Federal Government has committed more than $500,000.
However, Dr Agostino says the Therapeutic Goods Aministration’s (TGA) vaccination advertising guidelines did create some apprehension.
‘It scared a lot of our communities from putting out messages,’ he said.
‘We’ve had meetings with the TGA and clarified the difference between what is advertising and what is health promotion, and definitely, what our health services do is health promotion.
‘So we’re just trying to give them the confidence to get out there and do what they do best, which is create locally tailored messages that really resonate with the community.’
Dr Agostino says efforts have also been focused on strengthening safety surveillance systems to alleviate any concerns.
‘We’re working with AusVaxSafety and NCIRS [National Centre for Immunisation Research and Surveillance] to make sure that we have good coverage of Aboriginal and Torres Strait Islander people in our safety surveillance and that that data is getting regularly reported to the Aboriginal and Torres Strait Islander COVID-19 Advisory Group,’ he said.
‘So there’s a lot of things going on.’
Looking to the United States and Canada where vaccine rollouts are well underway with First Nations communities, Dr Schramm says it offers assurance for the Australian context.
‘We haven’t as yet seen any issues or problems with it,’ she said.
‘So we need to take that on and put that message out there to the community to know that this is safe, it is okay and is working well in other Indigenous communities around the world.’
Dr Agostino agrees, and says the success seen abroad reinforces the importance of the rollout being community-led.
‘If we look at First Nations communities in the United States and Canada, they’ve actually got faster vaccine uptake than the non-Indigenous populations,’ he said.
‘What we’ve learned from that is about the vaccine rollout being community-led. So, when the community is leading it, when the community is aware that it’s their health leaders that want this vaccine, and they’re the ones rolling up their arms getting it, they have control about who gets the vaccine and when, that’s when we’re seeing really great uptake.’
Dr Schramm says GPs have an important role to play in ensuring people know where to access reliable sources of information.
‘Be open to actually ask your patients what are their direct concerns, and being able to provide them with really clear, concise answers [and] particular places to find appropriate information about the vaccination,’ she said.
‘So that that message gets to the community about what are the actual risks? What are the actual side effects that I can expect from the vaccine? Why do I need to have it? And what is the advantage to me, and the rest of my community?
‘Get that message out there in a very culturally appropriate way, as we did for all of the messaging in and around COVID.
‘It just takes people a bit of time. If we can do that, I think the vaccination program in itself will be very positive as well.’
Log in below to join the conversation.
Aboriginal and Torres Strait Islander health COVID-19 cultural safety vaccines
newsGP weekly poll
Health practitioners found guilty of sexual misconduct will soon have the finding permanently recorded on their public register record. Do you support this change?