News
Medicare subsidy rate hits historic low
Figures show a huge shift in MBS subsidy rates among specialists outside of general practice, and large regional variations.
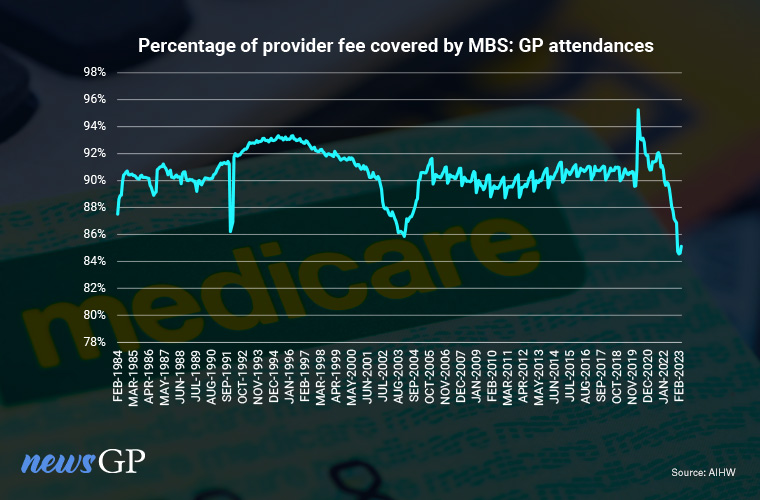 MBS subsidy coverage of general practice fees hit a record low in February 2023.
MBS subsidy coverage of general practice fees hit a record low in February 2023.
The proportion of fees covered by the MBS hit an all-time low in February this year, according to new data from the Australian Institute of Health and Welfare (AIHW).
Figures released this week track the amount of MBS health services provided, along with the proportion of the fee covered by the MBS patient subsidy, from the outset of Medicare to the present day.
It reports the subsidy rate declined to ‘well below’ any previous levels in February 2023 when it fell to 73% across all providers. The remaining portion is likely to have been covered by out-of-pocket fees or health insurance.
AIHW spokesperson Dr Adrian Webster described it as ‘the lowest national proportion since the MBS was established’.
While the amount of GP fees covered by MBS subsidies also hit a record low at the same time (84.5%), the level remained notably higher than for many other specialties.
MBS subsidies covered an average of 89% of service fees during GP visits in 2022, with the rate for general practice broadly comparable to the early days of Medicare, when it stood at 90% for the months the service operated in 1984.
However, the same is not true for other specialties, with anaesthetics and obstetrics now having the lowest subsidy rates, averaging 40% and 39% respectively during 2022.
More than 80% of provider fees for both those specialties were covered by MBS rebates at the inception of the system.
RACGP Rural Chair Associate Professor Michael Clements said the data reflected the recent increase in funding pressures across the healthcare system.
‘It’s not just a GP specific issue,’ he told newsGP. ‘The non-GP specialists haven’t been having their rebate increase as well.
‘That gap is just reflecting the fact that they’ve been keeping up out-of-pocket fees in accordance with growth better in some ways than GPs have.’
Associate Professor Clements also said patient choice is likely having an impact.
‘When somebody can’t afford to see the private obstetrician, then they can go through the public service, to the public hospital,’ he said.
‘We are often the only provider and there is no alternative, which is certainly one of the reasons why rural doctors feel pressured to either bulk bill or just close.’
The AIHW figures also show that people are accessing significantly more MBS-subsidised services on average than in the early days of Medicare.
In February 1984, MBS services were used at a monthly average of 0.6 per person compared to 1.5 per person in March this year.
Dr Webster cited a number of potential factors, including changes to the scope and coverage of the MBS, additional services, and the population’s changing age demographic and wealth.
The AIHW data also showed a significant shift in complexity, with around 2300 MBS items at the system’s launch in 1984 compared to more than 6000 presently.
According to the AIHW statistics, there is also a substantial regional difference in the way health services are used.
People in areas categorised as ‘very remote’ used 8.5 services per person last year, with a subsidy rate of 85%, compared to patients in major cities using 18.3 services with a subsidy rate of 76%. The AIHW notes that those are crude rates that have not been adjusted for age or other demographic factors.
Associate Professor Clements said some caution could be needed in interpreting the data for rural areas.
‘It can be a little clouded by the fact that many people access their health through non-Medicare services,’ he said.
‘For example, some RFDS [Royal Flying Doctor Service] clinics don’t use MBS, or hospital clinics don't use MBS.
‘It’s quite common for health planners to look at the MBS and say, “Oh, yes, well, there’s enough doctors up here … there aren’t enough doctors there”.
‘But we’re often at pains to point out to them that Medicare is not a good proxy for healthcare in a remote area because of the different funding models.’
For most services, there has been a slight uptick in the proportion of fees covered by MBS rebates in March and April this year, although the coverage remains close to historic lows.
Dr Webster noted that in 15 years prior to COVID-19, the overall proportion of MBS subsidies covering fees had remained relatively stable at around 79%, before rising during the early stages of the pandemic, then declining more recently.
The AIHW said bulk billed telehealth items and a reduction in services with higher out-of-pocket fees such as elective surgery, as well as the subsequent rollout of COVID-19 vaccines, were likely to have had an influence on those trends.
Log in below to join the conversation.
AIHW MBS Medicare
newsGP weekly poll
Would it affect your prescribing if proven obesity management medications were added to the PBS?