News
‘Professional attendance’ a sticking point in COVID vaccine rollout
More than 5000 general practices have put their hand up to take part in the nationwide vaccination program, but questions over MBS rebate requirements could stall momentum.
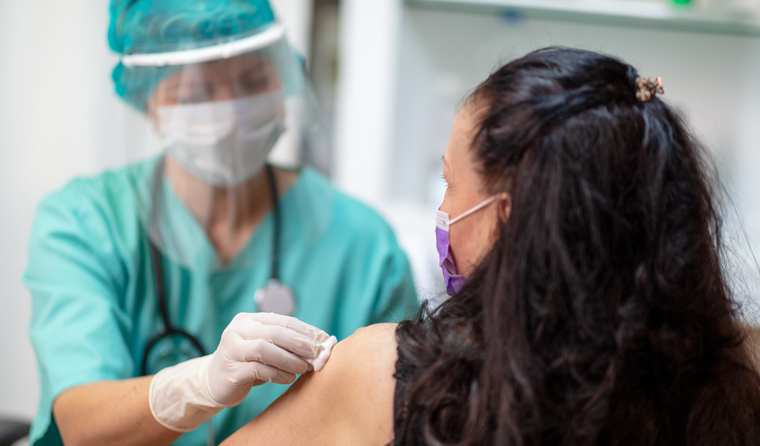 As it stands, GPs must attend to each patient receiving a COVID vaccine for practices to claim the MBS item number.
As it stands, GPs must attend to each patient receiving a COVID vaccine for practices to claim the MBS item number.
Practices that have expressed interest in taking part in the vaccination program will hear from the Department of Health (DoH) within two weeks.
But as the rollout date inches closer, a common concern has emerged among GPs; whether practices will be able to claim the Medicare Benefits Schedule (MBS) item number if the vaccine is administered by a practice nurse without a GP consultation.
During a recent COVID-19 webinar for general practice, Dr Lucas De Toca, Acting First Assistant Secretary for the DoH’s COVID-19 Primary Care Response, said the department is still working to finalise the descriptor in consultation with peak bodies, including the RACGP.
But as it stands, the items are classed as ‘professional attendance’.
‘They do require some degree of interaction of the GP in the conduct of the consultation,’ he said.
‘Of course, primary care functions in a multidisciplinary team and registered nurses, Aboriginal health practitioners or other authorised immunisers, according to the scope of practice and jurisdiction regulations, can provide the immunisation in itself.
‘But again, pending the finalisation of the MBS descriptor, these items are professional attendance items.’
However, RACGP President Dr Karen Price, who has been directly involved in the consultation process with the DoH, told newsGP such a requirement would make the vaccination program ‘very unworkable’ for general practice.
‘I think that would kill it dead in the water,’ she said.
‘The feedback from our members has been very strong on that.’
The rollout is set to be one of the largest mass vaccination programs ever undertaken in Australia, and the Federal Government has set a target of vaccinating all adults in Australia by October, starting with 80,000 doses per week.
However, to meet the target, new preprint modelling from the University of New South Wales suggests up to 200,000 people will need to be vaccinated per day.
That would require participating general practices to administer an average of 50 doses per day, seven days a week, for about six months.
‘Taking into account the necessary screening and record-keeping involved in addition to their usual workload, this may be quite a stretch for all but the largest practices,’ the authors note.
GP and practice owner Dr Mukesh Haikerwal, who is also a member of the RACGP Expert Committee – Funding and Health System Reform (REC–FHSR), is likewise concerned about the potential workload for GPs, especially if they are required to consult with every patient who receives a vaccination.
He told newsGP that while GPs should have ‘governance and oversight over everything’, that mandating they be ‘in front of every single patient, every single time, is just not tenable’.
‘We’ve got proper governance, we’ve got proper processes, we’ve got properly trained people that we are happy to have do some of the work whilst working to that governance structure – that is what every organisation does all the time,’ he said.
‘To tie it just to the GP, makes it very hard to make this work.’
Dr Andrew Webster, a Darwin-based GP and Head of Clinical Governance with the Danila Dilba Health Service, previously told newsGP the prospect of professional attendance also poses particular challenges for smaller practices and Aboriginal Community Controlled Health Services (ACCHOs) in remote communities.
He said nurses and Aboriginal health practitioners deliver the bulk of services, and only have a visiting GP fortnightly, or once per week at best.
While the DoH was unable to provide comment prior to publication, it is expected to finalise the language around the item descriptor soon.
Until then, Dr Price said the college will continue to ‘advocate strongly on behalf of our members’.
‘So that we can – as we always have – work in partnership with our fabulous nurses to deliver this,’ she said.
‘We support our nurses in that vaccination role by not necessarily attending every single patient, but certainly by being around and on call for medical issues.’
Log in below to join the conversation.
coronavirus COVID-19 MBS professional attendance vaccinations vaccine rollout
newsGP weekly poll
As a GP, do you use any resources or visit a healthcare professional to support your own mental health and wellbeing?