Feature
An ageing population and a GP workforce shortage: Is team-based care the answer?
newsGP speaks with a general practice where multidisciplinary care is the cornerstone of serving the needs of an increasingly complex patient cohort.
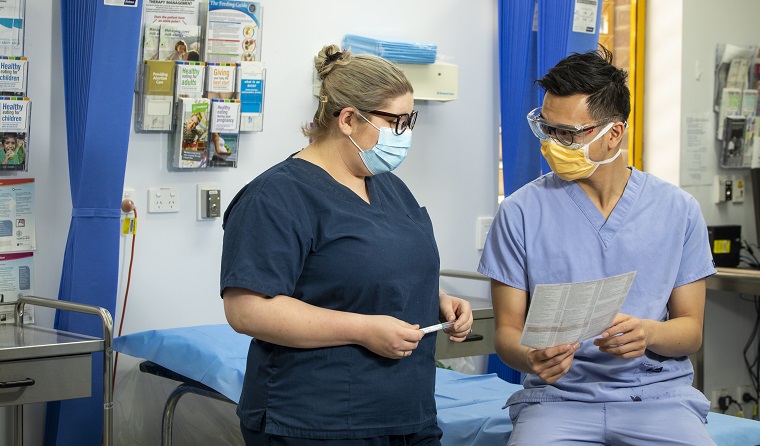 A nurse and a GP collaborating at Inala Primary Care. (Image: Supplied)
A nurse and a GP collaborating at Inala Primary Care. (Image: Supplied)
In less than a week, Treasurer Jim Chalmers will hand down the 2023–24 Budget with the healthcare portfolio – specifically strengthening Medicare and rebuilding general practice – set to be the Federal Government’s highest priority.
In February, patient-centred care supported by the expansion of multidisciplinary care emerged as a central recommendation in the Strengthening Medicare report with a view to managing Australia’s ageing population and a rise in complex and chronic disease.
This is a move away from the cottage style industry of delivering primary care, where individual doctors worked alone, to one of one collaboration and delegation – a transition that has been occurring at many practices for some time, among them Inala Primary Care.
The practice is based in Queensland’s largest social housing suburb, with more than 70% of its patients welfare dependent and more than 38% on five medications or more.
Tracey Johnson, the CEO at Inala Primary Care, told newsGP that team-based care is a reflection of the direction of modern medicine and says it serves as a ‘cultural anchor’ for the practice.
‘We acknowledge that GPs have a whole of life … responsibility for managing a patient but that GPs are not best positioned to do all the care for the patient,’ she said.
‘Medicine has moved on; we’ve now got well over 30,000, diagnoses and thousands of drugs and therapies available to us. So, philosophically, we have a stance that says team-based care should be usual care for patients who’ve got any sort of complex or ongoing issue, or who have particular episodes in their lives that might need care.’
The team at Inala is made up of 10 full-time GPs who are supported by a larger team of nurses working at different levels of scope – from treatment room nurses and chronic disease specialists, to credentialed diabetes educators and nurse practitioners – many of whom have worked at the clinic for many years, over which time they have upskilled.
Ms Johnson says this model, one that allows GPs to use their skills for work that only a doctor is trained to do, is communicated to all prospective employees during the recruitment process.
‘When it comes to chronic disease care planning for example … we have a rule that says no GP will ever do a care plan alone and that is because we’ve really upskilled our nurses,’ she said.
‘They do preventive health within their care plans, as well as all the primary and secondary prevention, care coordination and goal setting work that goes into a really decent care plan.’
In addition to GPs and nurses, the practice has embedded a variety of allied health professionals, including two part-time non-dispensing pharmacists, a podiatrist, physiotherapist, dietitian, social worker, and two psychologists.
The RACGP has been a vocal supporter for multidisciplinary care, including pharmacists, who the college says have an important role to play working under the stewardship of GPs in practice.
This is certainly the experience at Inala, according to Ms Johnson, who says the work of their in-house pharmacists is ‘incredibly invaluable’ to their GPs.
‘They review every incoming discharge summary from hospital before the doctors,’ she said. ‘If the discharge summary is inadequate, and they often are, they chase the hospital for further information.
‘They look at what’s changed in the medications, what might need to change again as the patient’s stabilised post-hospital, they book those patients in with the doctor to actually have a review and provide recommendations to the doctor around what needs to happen with medications.
‘In fact, our GPs are saying that our pharmacists could be given prescribing rights, so long as they’re working under the auspices and supervision of the GP. That’s what we’d like to see happening, but still have the GP as the lead and the pharmacist re-prescribing medications that the doctor has initiated.’
To further cater to the needs of its patient populations, the practice also has visiting nurses and non-GP specialists who work alongside the GPs to deliver specific clinics in areas including diabetes and hepatitis management, as well as refugee health.
Ms Johnson says taking the time to analyse its patient data and assess the best model of care for its aggregation of patients means the practice team can deliver better outcomes for patients.
‘I think in a lot of GP practices, because you’ve got doctors working pretty much solo as subcontractors, stepping back and asking that bigger question [isn’t always done]. But we’ve got the freedom to do that,’ she said.
‘We say we’re going to work as a team and then we decide how we’re going to work as a team on common areas of problems – whether it’s our 1000 patients with diabetes, our couple of hundred patients with hepatitis, our newly arrived refugee program, or our mental health stream.
‘We sit back and say, “What does the patient need? What does their journey look like now? What do we want their journey to look like in the future? Who’s best served to do that work that I need to induct into a team? Do they need upskilling in support?”
‘Quite often they do, and the GPs can be part of transferring skills to other members of the team so that together we can actually see more patients more efficiently and more effectively.’
Most health professionals, Ms Johnson says, tend to enjoy working as part of a team as it gives them a chance to share knowledge and the stresses of the day, making for an enjoyable and harmonious environment.
But is it financially viable?
Barriers to care
General practice funding has failed to keep up with the true cost of delivering quality care, resulting in a number of practices having to pass on costs to patients or close their doors.
Inala is no exception, with Ms Johnson admitting the practice has felt the pinch.
Over the past 12 months the clinic has moved to a mixed billing model, charging patients $20 out of pocket for certain services – a big decision given the practice cares for some of the state’s poorest patients – but she says, like other practices, they were left with no choice.
‘We have had patients ask for their records to be transferred to other clinics. They’ve been really quite angry and feeling like we’re leaving them in the lurch by introducing fees,’ Ms Johnson said.
‘But some of the practices that they’ve had their records transferred to over the last 12 months are now also charging. So very quickly our patients have found that their options for accessing free care are closing or closed.
‘We’ve had other patients who wanted to know more about why we’re introducing fees and we’ve been very clear with them: if we don’t introduce fees, we will close the doors. There’s not enough money coming into our kitty to retain staff and to pay all the bills.’
While she says the out-of-pocket fee has been confronting for patients, some of whom are being asked to pay for healthcare for the first time in their life, she believes that informing patients of the realities being faced in general practice is helping to create understanding and leading to a coalition of unhappy voters who are ‘sending a clear signal to Government, which says that funding is inadequate and something needs to be done for general practice’.

Inala Primary Care has 10 full-time GPs supported by a larger team of nurses working at different levels of scope. (Image: Supplied)
Following last week’s National Cabinet meeting, Prime Minister Anthony Albanese announced a series of measures designed to further support team-based care in general practice, including an expansion to the primary care nursing workforce and flexible funding for multi-disciplinary team-based models.
Ms Johnson says more needs to be done to retain nurses, noting that remuneration is low compared to hospitals and the aged care sector, but has welcomed the Government’s commitment to increase and index the workforce incentive payment (WIP) as a step in the right direction.
‘It needs to go up more and it definitely needs to continue to be indexed,’ she said.
‘The reality for us is our WIP here doesn’t even cover the full salary of one of our nurses and we’ve got five nurses in our core nursing team, let alone some of the other nurses that come in for some our specialty models of care.’
Other barriers include the need for more mental health professionals to be embedded into practices, as well as social prescribing to address the social determinants of health.
Meanwhile, Ms Johnson says as it stands the five allied health visits patients on chronic disease management plans can access is merely a ‘drop in the ocean’ for multimorbid patients.
This is where she says funding bundles to reflect a practice’s patient needs are important, ‘not some vanilla notion of who a patient is that might be defined in Canberra that has no reflection of the complexity’.
‘If you gave me a pharmacist full-time and a nurse practitioner full-time in my clinic, I would be able to increase my throughput of patients by somewhere between 30–50%,’ she said.
‘By having those other members of the team, they’re doing some of that shorter, quicker kind of medicine. It would free up my GPs to see a whole bunch of additional different patients and offer more comprehensive care to them.’
Patient populations
According to Australian Institute of Health and Welfare (AIHW) data, a woman aged 80 and over attends her GP practice 18.6 times a year. With people over the age of 80, and beyond that those aged over 100, Inala is being proactive and working on a Centre of Excellence for Ageing Well in Community Settings.
Without such initiatives, Ms Johnson, who also works with the AIHW on its health data collection, says she fears what is to come.
‘Our whole model of what are we doing with these people needs to change because it’s not sustainable to have those people in front of a GP in less than every three weeks,’ she said.
‘One of the things that we’ve got to get our heads around in this country is that the proportion of patients to GPs is one of the lowest in the OECD. And when you’ve got doctors that are only managing 600–800 patients, in some cases even less than that, we’ve got to ask ourselves the question: how do we provide access to a growing population of patients when we can’t grow our medical workforce anywhere near as fast?
‘We’ve got to expand the number of patients each GP is responsible for, but do it in a way that’s safe for the patients, not stressful for the doctor, and that pays for itself so that the doctor, the practice, and the system are getting the benefits of that investment.’
Ms Johnson says it all comes back to the team doctors are surrounded by. This, she says, will not only ensure patients receive quality care and better outcomes, but that practices will also be able to better attract and retain staff.
‘We need to be asking ourselves those proactive questions about who our patient population is and planning the interventions and the team we need around that, rather than being a reactive medical model where you just do what you can do in the time you have for the patients that come through the door,’ she said.
‘And that’s really the position that we’ve been forced to be in, where we just react to what comes through the door. You feel overburdened at the end of the day, get stressed and burnt out, realise how pathetic the money is that we’re making in the process, and we all decide that we just want to retire – we can’t end up with a system where these are the conclusions that people are drawing.
‘We need to build a team around GPs so they … enjoy work, it’s effective, it’s efficient, it’s population centred, and addresses need in the local community – the quintuple aim of healthcare effectively – and we can do this if we embrace team-based care.’
Log in below to join the conversation.
allied health Budget chronic disease funding GPs mental health multidisciplinary care nurse practitioners
newsGP weekly poll
Which of the following areas are you more likely to discuss during a routine consultation?