News
GPs given ‘uncertain’ estimates for risk–benefit vaccine consultations
The fact sheet GPs have been asked to use when discussing AstraZeneca vaccines with patients aged under 60 relies on limited information that fails to consider extensive data from abroad.
 The risk–benefit analysis can be particularly difficult in areas with ongoing community transmission.
The risk–benefit analysis can be particularly difficult in areas with ongoing community transmission.
There are questions over a newly-updated Federal Government fact sheet aimed at helping GPs make risk–benefit assessments with patients aged under 60 who have requested access to the AstraZeneca COVID vaccine.
The 10-page document includes tables that compare the risk of developing thrombosis with thrombocytopenia syndrome (TTS) in specific age groups, against the number of potential hospitalisations, ICU admissions and deaths that may be prevented by vaccination during varying levels of community transmission.
The tables were sent to GPs following Prime Minister Scott Morrison’s late-night announcement last week, while Deputy Chief Medical Officer Professor Michael Kidd has also encouraged GPs to ‘please refer to [the] risk–benefit charts when … having the discussions with your patients’.
However, fine print below the tables states that the ‘estimates for risks are uncertain’ for cohorts aged under 50, as the rates are based solely on the low number of vaccinations that have so far been administered in younger age groups domestically.
As a result, it suggests the TTS risk for patients considering AstraZeneca is highest among those aged 40–49, at five cases per 100,000 vaccinations, and that those aged 18–29 have a risk equal to those aged 80 and over at 1.9 cases per 100,000 vaccinations.
Meanwhile, ATAGI’s latest update, states the risk of TTS for under-50s collectively is 2.9 per 100,000, and 2.0 per 100,000 for those 80 and over.
Director of the Immunisation Coalition, infectious disease and vaccine expert Professor Robert Booy told newsGP while the fact sheet is a valuable document, it is also ‘confusing’.
‘The clot risks are based on small numbers of cases, [and so] the risk appears to be highest in 40–49-year-olds,’ he said.
‘[But the risk is actually] higher in your 20s and 30s of getting the clotting syndrome than if you’re in your 50s and 60s. At 25, there is a risk of clotting syndrome in the order of 1 in 25,000 after the first dose of AstraZeneca.
‘When Australian data is sparse, it is appropriate to look at UK data where they have a lot more expertise and experience.’
GPs have also lamented recent crucial vaccine changes being announced publicly without doctors receiving prior forewarning and Professor Booy shares their concerns.
‘GPs must be educated and informed before the public is about decisions,’ he said. ‘GPs need to be able to have the best, most recent data and analysis on which to properly and effectively advise their patients.’
RACGP NSW&ACT Faculty Chair Associate Professor Charlotte Hespe told newsGP her practice received more than 150 additional phone calls after the Prime Minister’s announcement last week from people under 40 looking to be vaccinated.
‘At our practice we sort of had a double confounder because we’re one of the practices rolling out Pfizer this week,’ she told newsGP. ‘And so we’ve had that mixed [request] of “I want to access Pfizer, but if I can’t access Pfizer, how can I access AstraZeneca?”.’
Associate Professor Hespe said given AstraZeneca had only been rolled out to a small number of people under the age of 40 before ATAGI changed its advice, that GPs should be using data from abroad.
She also said as the Government has not supplied GPs with consistent up-to-date guidance to conduct an adequate risk–benefit assessment, they have been forced to request this information from the state health department instead.
‘We’ve specifically requested this from NSW Health,’ Associate Professor Hespe said. ‘A bunch of documentation to assist GPs in the consenting of anybody under the age of 40, which will include actual evidence and current risk for us to really have that informed consideration.
‘They’re doing that on our behalf at the moment.’
The Department of Health (DoH) did not reply to questions on why the document GPs have been asked to use relies on insufficient data and does not reflect the higher risk of TTS posed to younger people.
‘Rates of thrombosis with thrombocytopenia syndrome [TTS] are based on Therapeutic Goods Administration [TGA] analysis of confirmed and probable cases of TTS in Australia,’ a TGA spokesperson told newsGP in a statement.
‘More information on rates of TTS are available in weekly TGA safety reports … and in weekly Australian Technical Advisory Group on Immunisation [ATAGI] TTS updates.
‘Australian rates of TTS are slightly higher than international rates, likely reflecting heightened clinical awareness and early case ascertainment.’
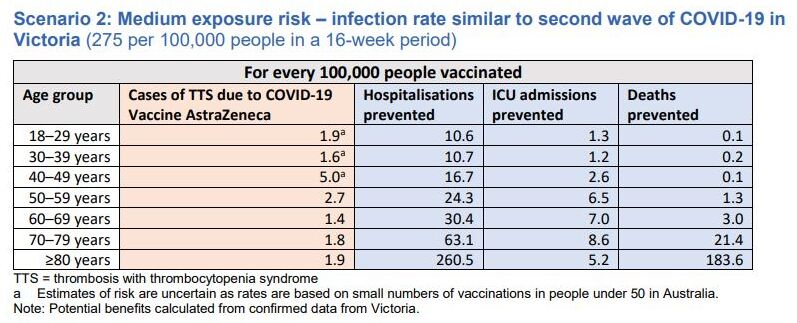
A screenshot of one of the tables GPs have been asked to use when conducting risk–benefit assessments with patients. (Image: Department of Health)
Like ATAGI, the UK’s Joint Committee on Vaccination and Immunisation has advised that adults aged under 30 (with no underlying health conditions that put them at higher risk of severe COVID-19 disease) should receive a different vaccine to AstraZeneca, if available.
But in situations like Sydney is currently experiencing – where more than 300 locally-acquired cases have been reported in the past fortnight – Associate Professor Hespe says the risk–benefit analysis can be particularly difficult.
‘I can’t [just] say to someone “You’re 28, so your risk of getting TTS is much too high for me to consider giving it to you, versus your risk of getting sick”,’ she said.
‘They may be doing something that if they unwittingly get sick, they then end up spreading it to 25 other people, who spread it to another five each, of which two people die.
‘If they sit down and go “Well, actually, I really don’t want to be the person who does that; that really, really worries me and I would rather take on the personal risk” that’s their choice, not my choice.
‘But personally, I’m saying to people [that] I still think it’s worth waiting, unless you’ve actually got that story of “I’m working in this scenario and I live at home with people who are at risk, and I really don’t want to be the cause of them getting unwell, as well as me getting sick”.’
To help individuals calculate the risk–benefit ratio for each individual person in the UK, an online calculator has been set up by the Oxford group and Professor Booy says a similar tool is needed for the Australian context.
‘Several groups are working on just that,’ he said. ‘For example, the Immunisation Coalition is in discussion with the Oxford group to quickly adapt their instrument to Australia.
‘In the meantime, GPs are well equipped to answer people’s questions; their opinions are respected, and the Government is supporting GPs to have enough time to undertake meaningful discussions with their patients about vaccinations.’
While there has been much confusion, Professor Booy says there is now a need to move forward ‘to undo the damage and improve GPs’ understanding’ so that patients can be advised as accurately and appropriately as possible.
‘It’s vitally important for the chief health officers, the premiers, and the experts who advise them to get together around a Zoom table and spend a good few hours thrashing out the best advice, the best communication, the best way of advising the public, so that we can be talking all on the same page,’ he said.
‘We just hit one million people a week. That’s a great improvement, but it needs to be 1.5 million people a week for the next 6–8 weeks, and then we need to get up to 2–3 million per week.
‘Only if we do that can we reach Christmas with every adult offered vaccination.’
Log in below to join the conversation.
AstraZeneca COVID-19 Pfizer risk–benefit assessment vaccine rollout
newsGP weekly poll
Health practitioners found guilty of sexual misconduct will soon have the finding permanently recorded on their public register record. Do you support this change?