News
Peer-reviewed AstraZeneca data raises questions over vaccine rollout
Publication of the highly anticipated data has highlighted the need for further trials to confirm dosage and efficacy.
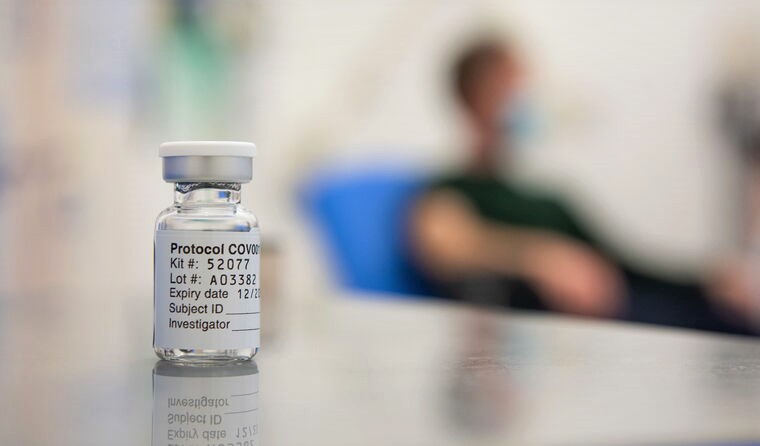 AstraZeneca and the University of Oxford are the first to publish full data on a vaccine for COVID-19 in a peer-reviewed journal. (Image: AAP)
AstraZeneca and the University of Oxford are the first to publish full data on a vaccine for COVID-19 in a peer-reviewed journal. (Image: AAP)
It was in August that Australia signed its first deal for a vaccine against COVID-19, placing its hopes of a return to normal on the efforts of AstraZeneca and Oxford University.
But the race for a vaccine has since taken a turn.
Long-awaited interim data from four randomised controlled trials published in The Lancet on Tuesday confirmed the vaccine’s safety, but left many crucial questions on dosage and efficacy unanswered, highlighting the need for further trials.
But Professor Dale Godfrey, Immunology Theme Leader at the Doherty Institute, told newsGP any delays that may result from further trials are unlikely to have a major impact on Australia.
‘I certainly think it’s an important thing to resolve. But I don’t think it’s a disastrous turn of events for Australians,’ he said.
‘Firstly because we do have the potential to access other vaccine candidates, and we have more time to see how the different vaccines perform as they are rolled out overseas.’
The published data has confirmed the vaccine’s efficacy rate at 70.4%, but that figure was reached by combining the results of two different regimens that vary considerably in efficacy.
The majority of volunteers received two standard doses, which resulted in an efficacy rate of 62.1%. This is compared to a smaller group, less than 6% of trial participants, who mistakenly received one-and-a-half doses and recorded an efficacy rate of 90%.
It was later revealed these dosing irregularities were the result of a manufacturing error.
The study authors concluded that ‘further work is needed’ to determine the reasons behind the lower dose recording higher efficacy.
‘[It] might be due to higher levels of neutralising antibody, lower levels of anti-vector immunity with lower vector-derived antigen content of the first dose, or differential antibody functionality or cellular immunity, including altered avidity or immunodominance,’ the authors hypothesised.
The data also failed to give insight into the vaccine’s effectiveness in older people. Only 12.2% of volunteers who received the two full doses were aged over 55, and just 4% over 70. All volunteers who received the more effective lower dose were aged 55 and under.
‘Vaccine efficacy in older age groups could not be assessed but will be determined, if sufficient data are available, in a future analysis after more cases have accrued,’ the study states.
Based on what it known so far, AstraZeneca is lagging behind competitors Pfizer/BioNTech and Moderna, whose vaccine candidates have reported an efficacy rate of 90% and 94.5%, respectively.
Professor Godfrey says this is likely to be more of a concern in northern hemisphere countries, many of which are experiencing significant community transmission.
‘At the moment in Australia, you probably wouldn’t be able to tell if a vaccine was working or not with our current situation, because there are no cases coming up anyway,’ he said.
‘So I think it’s nowhere near as urgent for people in Australia to be getting a vaccine as it is for people in the northern hemisphere.
‘Of course, we know that can change pretty quickly. It might be that there’s another outbreak tomorrow and suddenly we’ll all be screaming out for a vaccine – so nothing’s too certain in these times.
‘But let’s hope that doesn’t happen and that we get a bit more time to observe which vaccines perform the best and we aren’t desperately trying to get everyone immunised by yesterday.’
The data has shown some promise, however. In addition to having a good safety profile, AstraZeneca’s candidate is cheaper at US$2–3 per dose, easier to manufacture, transport, and store using routine refrigerated cold-chain, when compared to mRNA competitors Pfizer/BioNTech and Moderna that must be kept at sub-zero temperatures.
But Professor Godfrey says the potential for logistical challenges with mRNA vaccines may not be the case long-term.
‘It may be that they only have approval to store and transport at that temperature, it may turn out that their vaccine is stable for some time at higher temperatures,’ he said.
‘These are all first-generation vaccines, and I don’t think this is all we’re going to need. People are really just hoping that these will start to reduce the impact of this disease and set us up to start to return to normality, but it may take second- and third-generation vaccines that demonstrably prevent infection and transmission, not just disease, until we really can get back to normality.
‘Only time will tell.’
Federal Health Minister Greg Hunt welcomed the publication of the vaccine trial results as ‘great news’ for Australia.
‘The AstraZeneca vaccine is being produced as we sit here in parliament in Melbourne, by CSL,’ he said.
‘These things are critical for saving lives and protecting lives and giving us a strong 2021.’
With the World Health Organization having indicated a required
minimum efficacy of 50% for an effective COVID vaccine, AstraZeneca Executive Vice President Sir Mene Pangalos said the company plans to submit the newly-published data for regulatory approval.
‘We hope that once the regulatory authorities review the data, we can get approval any time from the completion of the submission, which could be any time from the end of this year to early next year,’ he said.
The data’s release coincided with
the rollout of the first doses of Pfizer/BioNTech’s vaccine after it was
approved for emergency use in the UK among priority groups, including healthcare and aged care workers, and older patient cohorts.
AstraZeneca and the University of Oxford are
the first to publish full data on a vaccine for COVID-19 in a peer-reviewed journal.
In
a commentary accompanying the article, Dr Maria Deloria Knoll and Dr Chizoba Wonodi of John Hopkins Bloomberg School of Public Health dubbed the mix up in vaccine dosage as ‘fortuitous’ in helping to uncover a potentially highly efficacious formulation.
‘But [it] was unplanned, and needs further evaluation in older adults and to confirm the unexpected results.’
Log in below to join the conversation.
AstraZeneca COVID-19 Oxford University vaccine
newsGP weekly poll
Which of the following areas are you more likely to discuss during a routine consultation?