Australian doctors have higher rates of stress and more attempts at suicide than the general Australian population,1 with an increased burden on those in their junior medical years and early stages of training.2
Burnout has been recognised as a causative factor for depression and suicide in the medical profession.3 It is considered to be a response to multiple significant stressors4 and incorporates feelings of emotional exhaustion, depersonalisation and reduced personal accomplishment.5
Burnout has been shown to have an impact on the person, their patients and the workforce. Junior doctors who report burnout are more likely to report increased absenteeism and depression, have self-reported medical errors and engage in risky alcohol use.6 The personal consequences are serious, with studies linking burnout with psychiatric morbidity7 and an increased incidence of suicidal ideation and suicide in doctors.8 Research has identified a number of contributory external factors for burnout, including job demands such as excessive patient loads, long working hours, difficult rostering requirements and disproportionate on-call and out-of-hours work,6,9 difficulty in maintaining work–life balance and issues managing challenging interpersonal relationships.9
An answer to burnout that has been introduced across Australian medical training environments is that of ‘resilience training’, where resilience is described as the ability to respond and react to difficult situations.10 However, there are mixed views on resilience training. Initially, resilience was hypothesised to be a way for doctors and medical students to process and manage daily ethical struggles and practice good professional development.11 Others see such training as a simplistic model providing only a short-term solution, where the individual is responsible for identifying and resolving workplace stressors rather than cultural or organisational factors being addressed at a system level.12,13
Burnout is an important problem with significant consequences. To our knowledge, the contrasting experiences of the demands across general practice training and hospital-based training have not been previously examined to identify if there are any causative factors for burnout that differ across the two environments. The aim of this qualitative study was to compare the experiences of hospital and community-based doctors in unaccredited and specialty training across known and hypothesised causative factors for burnout. The objective was to identify personal and environmental factors that may be involved in both the exacerbation and prevention of burnout in junior doctors in order to inform future interventions and research.
Methods
Population and recruitment
The general practice participant cohort was recruited by advertising in the regional training organisation’s newsletter, and the hospital cohort was recruited using convenience sampling through the local hospital junior medical officer unit, with one participant recruited by word of mouth. All participants were based in New South Wales or Victoria, Australia. Interviews were undertaken in person or via phone, as chosen by the interviewee. RH completed all interviews.
Interviews analysis
The interview guide was developed from themes arising from the literature and from personal experiences from the authors.
Questions included:
- What makes you feel stressed?
- Where do you go when you feel stressed/burnt out?
Recordings of interviews were de-identified and transcribed; interviewer field notes were kept. Participants were recruited and data collection continued until saturation was reached (a point at which no new themes were identified and there were no new codes being added to the themes).
Analysis
The research team included two doctors, one training in general practice (RH) and one with over 25 years of clinical general practice experience (AB). The researchers aimed to consider their personal biases in the choice of topic, analyses and interpretation.
Both authors read all transcripts in full, and codes inductively developed by RH were discussed and confirmed with AB. NVivo was used to assist with data management and grouping of codes for thematic analysis. In an iterative process, the analysis of the codes and formation of themes that developed from the analysis by RH was revised in consultation between the authors. The COREQ guidelines were used to guide the rigour of the analyses; respondents were invited to review their transcripts.14
Results
Ten interviews were completed and included in the analyses. Six participants were male and four were female. Interviewees were in their second to fifth postgraduate years; the majority (n = 4)were in their third postgraduate year. Half of the participants were general practice registrars (ranging from GPT1 to GPT4) and half were hospital doctors. Interviews ranged from 10 to 42 minutes in length. Data saturation was achieved by the seventh interview. Quotations are coded using H for hospital junior doctor and G for general practice junior doctor, then assigned numbers based on interview order.
Across both the hospital group and the general practice group, the same themes and codes were replicated, with no difference in causative factors identified between the groups. Three broad themes were identified in the analyses: expectations of self; expectations and response of others; and self-care.
Expectations of self
The first key theme emerged from the junior doctors’ experiences with limitations in their own knowledge and ability. This limitation was exacerbated in times of uncertainty or unfamiliar situations and intensified in a perfectionist, high-achieving personality type.
Both hospital and general practice doctors felt some anxiety concerning their ability to practice and how competent they felt working independently. Both groups felt increased stress when they thought that they were working beyond their current competency levels.
What made me feel stressed was … not being certain of my skills and my anxiety about when I went to make calls and things. (H2)
I guess what would make me feel stressed, one thing would be support, like feeling that you don’t have sufficient support or supervision, especially when it’s early on in your career or if you’re in a new position and you’re not sure about decision making and what your role is meant to be. (G5)
The acknowledgement that certain personality types are more likely to enter medicine was identified by one participant.
Huge amounts of work and expectations, both internal and external expectations. And, not feeling like I have enough time to meet these expectations to the standard that I want to hold, I’m a bit of a perfectionist … I had no idea that I was a Type A personality until I entered medicine, and I was like, ‘Yes, that is my experience too.’ She was like, ‘I always thought I was so easy going,’ … yeah, it just sort of went haywire. (G2)
Expectations and response of others
The next theme identified was that of the expectations that the junior doctor has of other people and of their working environment, and the responses they receive from others. The expectation from junior doctors was that they would be working in a safe environment supported by their direct supervisors, teams, hospitals, colleges or colleagues, especially when stressed or in need.
The working environment has been identified as a clear stressor for both hospital and general practice registrars, with long hours and high patient loads being a recurrent theme for increased burdens.
At one stage when she was ortho reg [orthopaedic registar], in 25 calendar days, she spent 12 hours at home. (H5)
No registrar on site when I work my afterhours, it’s just me … I really don’t mind working after hours, it’s more that I don’t feel comfortable doing it by myself. (G5)
Increased stress around preparation for examinations has been identified by multiple respondents as a key exacerbator of stress and possibly a contributor to burnout and suicide.
And, so when I hear of these people committing suicide … the one thing that can’t be removed is the pressure to sit exams … that exam pressure can’t be ameliorated by anybody and so, unless we change the system … that’s never going to change the suicide rate. (H2)
You don’t have time, you’re working full-time and then you’re trying to write a paper or do a little bit of research, and turn up to these courses, and study for your primary or entrance surgical exams. (H5)
There are senior staff and training organisations that manage junior doctors throughout their junior doctor years. These include the direct supervisor, administrative teams and senior hospital or college supports.
The direct supervisor/team were seen as being supportive when all was going well and there were no conflicts. In situations where the junior doctor had encountered issues during the term and had approached their immediate senior for assistance, there was an overall feeling of not being provided the anticipated levels of support.
I’d already had meetings with my consultants and I didn’t feel like there was going to be any support from there. (G5)
For some it seemed that the senior clinicians had forgotten what the early training years were like.
They’ve been too far removed from their internship years; it’s 10, 15, 20 years on and they’re now an FRACP or FRACF or FRAC something, and they don’t remember how horrible it was when they first started out. (H5)
The medical administration (hospital) and regional training organisation (general practice) were seen as uninterested and unhelpful when approached by stressed registrars who needed further support.
From the hospital administration, the medical administration, shocking … I mentioned that I didn’t feel comfortable with the work and I needed more supervision … I felt concerned about patient safety … they just gave up and became exasperated by it all. (H4)
My training provider provides … [nothing useful] … It’s appalling … They say all the right things but I think actions speak louder than words. (G2)
However, for registrars who did not need to approach this level of supervision for any additional help or support, they were seen as kind and approachable.
The hospital admin, they seem okay. I mean, the JMO [Junior Medical Officer] manager ... she’s very approachable, so that’s great … Almost all the time it’s no hiccups and so you just turn up to work. So, that’s fine by me. (H5)
The training doctors’ college (only The Royal Australian College of General Practitioners general practice registrars were interviewed) or hospital senior administration were seen across the board as lacking in support and empathy.
You are totally vulnerable and at the mercy of the system. (H2)
Who wins at the end of the day is the practice, and the college knows about it … (G1)
I don’t think that college is really doing much about it because of financial conflicts of interest. (G3)
Self-care
The final key theme identified was that of self-care – one’s ability to negotiate the work–life balance. All participants were aware of the importance of self-care, and common strategies emerged, especially diet, exercise and engaging in personal relationships. Prioritising self and family were common goals that were seen as signs of being in a good mental state and also an opportunity to reduce stress. Neither the hospital doctors nor the general practice registrars prioritised having their own doctor as a strategy for reducing burnout, and one participant identified this as a key barrier that was increasing the rates of burnout in his colleagues.
All participants considered diet and exercise as critical for self-care and preventing burnout, and a good way to distract oneself from the workplace.
I enjoy walking to work and from work. It’s a good switch-on/switch-off. (H3)
Relaxation techniques, such as meditation, were also common across both groups, with many junior doctors participating in regular mindfulness and meditation activities.
I use exercise and meditation and talking to people, they’re probably my main stress management techniques. (G1)
I try and sit down and take a few slow breaths, call a friend, go to yoga. (G4)
I think that’s really important. I’ve got my cat sitting on my lap right now. (H2)
Balancing and juggling prioritisation self‑care and work–life balance was seen as important but difficult to achieve.
So, pretty much mental state–wise it’s a juggle between physical exhaustion, mental exhaustion and emotional kind of exhaustion, I guess, so, I don’t think you can have it all. You’re either going to be tired but happier, or less tired but miserable. (G3)
Those with families actually found they were able to prioritise life balance more easily and found that their families provided an escape from the stress at work.
I find just spending time with them a really good stress relief. I have to say that having a little one has probably made me mellow out a bit. She’s certainly made me focus less on work. (G3)
One participant identified health-seeking as being underused by themselves and their colleagues, and this underuse was considered to be a key contributor to the exacerbation of stress and burnout. This participant saw an opportunity for early teaching to increase awareness and use of self-care strategies.
There could be a role for greater support at the university level or greater dissemination of information at the university level so that people start to develop some skills in health-seeking behaviours. (G1)
I think that’s one of the biggest barriers. The friends that I’ve supported have just really, really struggled to access care. (G1)
Junior doctors saw resilience training as a strategy used by employers to appear as though they are doing something to improve wellbeing without actually looking at the cause of the problems.
It’s for show … we’ve been offered resilience training, wellbeing courses and encourage sort of work–life balance and healthy eating. I mean, I think that’s all well and good … it is almost implying victim blaming. So, if a person actually suffered, or even killed themselves because they weren’t resilient, because they didn’t eat well, because they weren’t exercising. I almost feel it’s a bit patronising, that we’re implying the current cohort of JMOs is actually not strong enough, we need to make them stronger so that they can survive the training. (H5)
When all three themes interact
The doctors who were able to identify a time when they had experienced burnout identified a deficit in more than one of the themes described above. One junior doctor described a situation where they had a poor outcome and expected themselves to behave differently, did not receive support from their senior staff and were lacking in their self-care strategies. After the incident, they engaged some external help to identify the cause and strategies to prevent future occurrence.
My behaviour was – is inappropriate … And, at that stage, I did not feel supported at all … [the hospital] offered me the EAP [employee assistance program], and I thought bugger that, I went and paid my own psychologist … just talk it over with her, so I did three sessions or whatever to really get to the bottom of it … but it could have turned really bad. So, I don’t know whether it’s because people were just too busy, or they just didn’t care, or whatever. Maybe I’m just more touchy feely than most other people, I don’t know. (H5)
Discussion
The junior doctor years are stressful, and recently published studies on mental health issues and doctor suicides have acknowledged the need to identify what can be done to reduce the emotional burden, especially among junior doctors.2,4 From the findings of this study, it is clear that there are many factors that have an impact on junior doctors’ stress, including their ability to self-care, their expectations of their own abilities and knowledge, and their expectations and the response of others.
Our findings compared experiences of junior doctors in hospital and general practice environments. We found that both populations experienced unexpected factors that contributed to their stress. Neither group was better prepared for their practice or better at self-care. Both groups felt unsupported by their senior staff and support networks in times of stress.
Previous research has identified the interaction between work and personal stress as a multicausal model for burnout.15 The CARE study, looking at burnout in nurses, also proposed a multifactorial causality to burnout.16 The authors recommended strategies to reduce the occurrence of burnout and highlighted the need to focus on multiple elements, noting that supporting one element alone was insufficient and likely to be ineffective.16 Our study builds on these studies by identifying specific focus areas that contribute to burnout and hypothesising further research opportunities to minimise burnout within the junior doctor population.
On the basis of our findings, we hypothesise that the three elements – expectations of self, expectations and response of others, and self-care – are linked and balanced with one another, and we propose a model for burnout. The participants who were able to clearly describe a time when they were burnt out described a deficit across all three of these areas; those who were able to identify themselves as stressed but still coping maintained balance in at least one of the domains.
Figure 1 illustrates this hypothesis. Where two areas are affected, the junior doctor experiences stress. With all three affected, they are at risk of burnout.
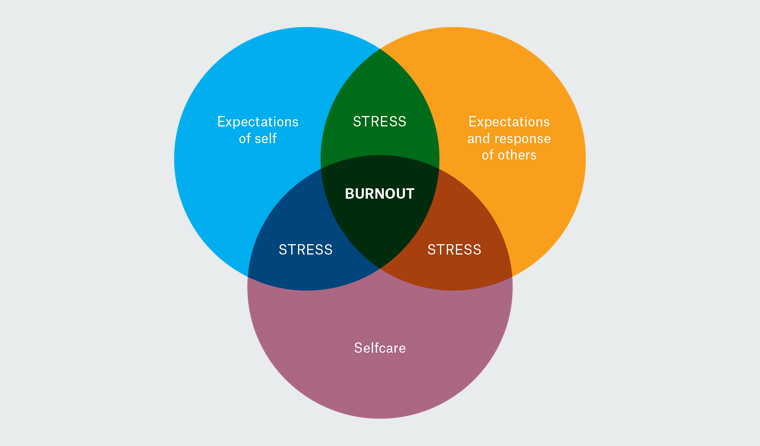
Figure 1. Model for risk of burnout
Limitations
Limitations of the study are the method of participant recruitment and the sample size. Those who chose to participate in the study self-selected and may have either experienced burnout or had a specific interest in the topic. As a result of the small sample size and nature of qualitative research, it may not be possible to apply this model to broader populations.
Conclusion
Our findings suggest that junior doctors will burn out when they fail to be supported by others, are working beyond their perceived abilities and are not engaging in self-care. Further confirmatory research and intervention studies are required to explore the hypotheses raised by this study and the viability of implementing this model into junior doctor or medical student training. It is important across the entire medical profession that burnout is researched and evidence-based methods for reducing it are funded and implemented.
Implications for general practice
The hypothesised model allows doctors to identify the need to prioritise self-care and the need to be fully informed of the expectations of new roles and career pathways. For those who work with junior doctors, this model identifies a need to ensure that strategies are research-based and do not shift blame. With the current changes in the training environment, there is an opportunity to introduce new policies and guidelines to encourage each theme – expectations of self, expectations and response of others, and self-care – to be further researched and included as a preventive measure in the general practice training environment, instead of the current focus purely on the individual’s abilities to manage confronting situations.