Brucellosis is a disease caused by the intracellular, Gram-negative bacteria, Brucella species. Numerous species and biotypes (biovars) have been identified, but the most important ones from the human health perspective are:
-
B. suis
-
B. melitensis
-
B. abortus
-
B. canis.
The animal reservoirs and situation in Australia regarding each of the above species are listed in Table 1. B. ovis is present in sheep in Australia, but is not zoonotic.
| Table 1. Main Brucella species of importance to human health, including animal reservoirs and main risk groups in Australia |
| Species |
Main animal reservoir |
Disease situation in animals in Australia |
Main risk groups in Australia |
| B. suis |
Pigs |
Absent from domestic pigs but present in feral pigs in Australia. Dogs involved in feral pig hunting or fed raw feral pig meat may become infected |
Feral pig hunters, breeders, veterinarians |
| B. melitensis |
Sheep and goats |
Absent from sheep and goats in Australia |
Migrants from, and travellers to, countries where B. melitensis occurs in animals |
| B. abortus |
Cattle |
Absent from cattle in Australia (eradicated in 1989) |
Migrants from, and travellers to, countries where B. abortus occurs in animals |
| B. canis |
Dogs |
Absent from dogs in Australia |
Never reported in Australia |
Epidemiology
Brucellosis has a worldwide distribution. Between 1991 and 2016, an average of 30 human cases were diagnosed annually in Australia (1.6 cases per 1,000,000 population), 80% of which occurred in Queensland (6.7 cases per 1,000,000 population).1
In Australia, hunters and dogs become infected with B. suis following direct contact with feral pig tissues and blood via skin abrasions and mucous membranes during the hunting and slaughter process. Dogs, particularly farm dogs, can also be infected if they are fed raw feral pig meat or offal. Transmission of B. suis from dogs to humans has been documented;2 however, the principal risk to humans appears to be around the time a female dog is giving birth (eg breeders) and during surgical procedures (eg veterinarians performing de-sexing operations).3 To date, no humans in Australia have been infected through casual contact with an infected dog.
In countries where B. melitensis and/or B. abortus are present in animals (ie not in Australia), transmission occurs principally through ingestion of unpasteurised dairy products (especially cheese), or through direct contact with animal tissues (especially aborted fetuses), blood and urine via skin abrasions and mucous membranes.4 Aerosol transmission is also possible, particularly in laboratory environments. For this reason, Brucella species are considered a potential bioterrorism agent. Person-to-person transmission of brucellosis is extremely rare, and has been associated mainly with breast milk to a newborn;5 presumed sexual transmission has also been documented.6
Risk factors
Brucellosis was once a common abattoir-associated infection in Australia. Now that B. abortus has been eradicated from livestock in Australia, the main risk factors for brucellosis in patients presenting to clinicians in this country are (Figure 1):
-
feral pig hunting (B. suis) – particularly when carcasses are dressed in the field7
-
travel to, and/or consumption of unpasteurised dairy products manufactured in, countries where B. melitensis and/or B. abortus are present in animals, such as Mediterranean countries (Portugal, Spain, southern France, Italy, Greece, Turkey), the Middle East, central Asia, India, Central and South America, and Mexico.
Less common risk groups include:
-
farmers, abattoir workers and other animal handlers who have a history of working in countries where B. meletensis and/or B. abortus are present in animals – these people may manifest with signs of brucellosis after migrating to Australia
-
people who work in microbiological laboratories who handle Brucella cultures
-
people involved in storage, transport or processing of feral pig carcasses – these people may be at risk of acquiring B. suis from feral pigs in Australia
- veterinarians, dog breeders and (possibly) household contacts of feral pig hunters – these people may be at risk of acquiring B. suis from dogs in Australia.
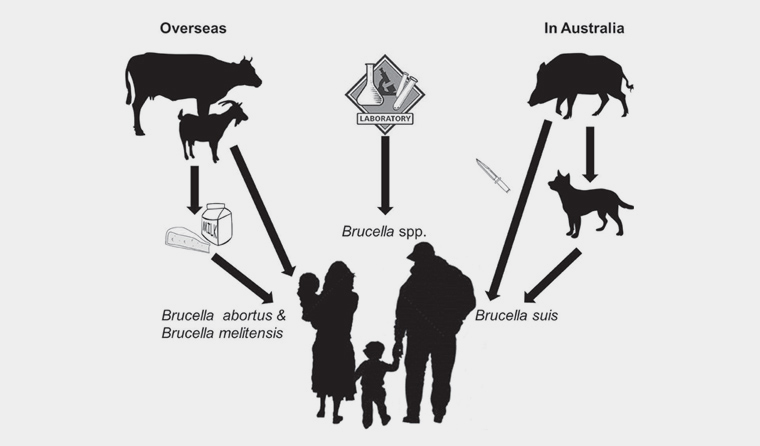
Figure 1. Main exposure pathways for brucellosis in patients presenting to clinicians in Australia. Brucellosis is re-emerging locally in association with feral pig hunting activities (right). Brucellosis is also seen in returning travellers and migrants from endemic countries, who acquire the infection through consumption of unpasteurised dairy products (left).
Pathophysiology
An infectious dose of 10–100 organisms is sufficient to cause systemic infection.8 After entry of the organism, three main phases can be distinguished: incubation phase, acute phase and chronic phase.9 The incubation period of brucellosis can be variable and difficult to ascertain, but is generally two to four weeks, with a range of five days to five months.4 The acute phase is characterised by the onset of signs and symptoms such as fever, sweats, fatigue, hepatomegaly and splenomegaly.10 Because of several virulence factors, Brucella is able to survive in host cells and evade host immune responses to establish chronic foci of infection.9,11
Clinical features and complications
Most cases of brucellosis have a gradual onset, although abrupt onset is also possible. Sub-clinical infection with Brucella species has also been reported.12
Brucellosis is a systemic infection in which any organ or system of the body can be involved. The symptoms are often non-specific, as are physical examination findings, although lymphadenopathy, hepatomegaly or splenomegaly can be present. Common symptoms include:13
-
fever (relapsing, mild or protracted) and sweats
-
anorexia and weight loss
-
fatigue and malaise
-
arthralgia, myalgia and back pain
-
headache
-
depression.
Depression is often severe, relative to other symptoms, and occurs in around 30% of patients.14
Osteoarticular complications, of which sacroilitiis is the most common, occur in 30–70% of cases.13 Other complications include genitourinary disease, most commonly epididymo-orchitis (10%).15 Brucellosis is associated with spontaneous abortion in animals; however, it is not clear if abortion is more common in brucellosis than other bacteraemias in humans. Nonetheless, in countries where B. melitensis is endemic, spontaneous abortion in the first or second trimester has been reported to occur in around 40% of pregnant women with brucellosis.16
Hepatosplenic brucellomas have also been reported, although any organ may be involved with a chronic suppurative granulomatous process. These focal suppurative sequelae may manifest years after the exposure event, even with treatment. Other rare complications of brucellosis include:
-
neurobrucellosis, usually presenting as acute or chronic lymphocytic meningitis17
-
cardiovascular manifestations such as endocarditis, aneurysms, myocarditis or pericarditis (often the main cause of death from brucellosis)18
-
respiratory complications, such as bronchopneumonia and pleural adhesions15
-
endophthalmitis.19
Overall, the case fatality rate is 2%.4 Early diagnosis and treatment are important for limiting duration and preventing complications.13 The disease may last months to years if untreated. Despite appropriate antibiotics, relapse occurs in up to 10% of all patients,20 and this usually occurs within the first year after infection.
Differential diagnosis
Given the wide spectrum of clinical presentations, brucellosis has earned its place alongside syphilis and tuberculosis as one of the ‘great imitators’ and causes of pyrexia of unknown origin. The non-specific symptoms are common and may mimic diseases such as tuberculosis, toxoplasmosis, infectious mononucleosis, typhoid (in overseas travellers), hepatitis, systemic lupus erythematosus and many others. When focal infection develops, localised symptoms may predominate.
Clinical features of brucellosis are similar to those of Q fever (caused by Coxiella burnetii), and risk factors for both of these diseases often coexist in a similar demographic.13 Determining risk factors for Brucella exposure (eg feral pig hunting, overseas travel) is important for narrowing the clinical differential. Note also that Q fever usually has an abrupt onset, which contrasts with the usual gradual onset of brucellosis.
Diagnosis
If acute brucellosis is suspected, serology and blood cultures are recommended. Serum IgM is often detectable at presentation because of the insidious nature of the infection, and cannot be relied on for diagnosis as cross-reactions may occur with other infectious agents. Diagnosis of acute brucellosis is confirmed when seroconversion for Brucella IgG (enzyme-linked immunoassay) or a fourfold increase in agglutinating titres and complement fixation test (CFT) on convalescent testing are demonstrated.
Blood cultures are important in the workup of suspected Brucella infection. Growth of the bacteria from blood cultures not only confirms the diagnosis, but allows speciation of Brucella which, if acquired in Australia, is invariably B. suis. Infections acquired from overseas in travellers, migrants and refugees are more likely to be due to B. melitensis. Blood cultures are also part of the ‘septic screen’ to exclude other causes of febrile illness. Two sets of blood cultures are recommended to detect bacteraemias. The organism is a laboratory hazard; therefore, it is prudent to notify the laboratory if brucellosis is suspected.
In relapsing disease, blood cultures are more useful than serology, as serological tests will already be positive at the time of relapse. Imaging techniques (ie radiographs, ultrasound, computer tomography [CT], magnetic resonance imaging and 18F-FDP- positron emission tomography/CT scan) are of value in localising focal suppurative lesions for further biopsy. Confirmation of relapsed infection is based on typical granulomatous histopathology of involved tissue, nucleic acid amplification testing (PCR) of tissue and culture of the organism. Both genus-specific and species-specific Brucella PCR assays are available from public health reference laboratories, and have most value when used on culture negative tissues and for organism speciation.
Management of brucellosis
Dual therapy with doxycycline and gentamicin is the recommended treatment for brucellosis.21 Oral therapy with doxycycline is required for six weeks, with adjunctive daily intravenous gentamicin for the initial seven days (Table 2).
entamicin reduces the rate of treatment failure and relapse, but can be associated with significant renal, vestibular and ototoxicity, requiring specialist therapeutic drug monitoring and hospital admission.
If gentamicin is contraindicated or relevant precautions preclude its use, oral rifampicin daily for six weeks can be used instead in combination with doxycycline. It has been noted that clinical relapse occurs in up to 10% of cases even after a six-week treatment course; a higher failure rate is associated with rifampicin–doxycycline compared with gentamicin–doxycycline.20 If a patient presents with relapse, collect blood cultures, noting the likely diagnosis on the request form. Complicated Brucella infections (eg osteomyelitis, endocarditis) require longer durations of therapy and, on occasion, concomitant surgery. It is recommended that diagnosis and management of brucellosis cases be discussed with an infectious diseases specialist.
| Table 2. Current recommended antibiotics for the treatment of brucellosis according to eTG21 |
| Patient category |
Antibiotic |
Dose |
Adults and children
8 years or older |
Doxycycline |
100 mg (child 8 years or older: 2 mg/kg up to 100 mg) orally, 12-hourly for six weeks |
| Plus gentamicin*† |
5 mg/kg (child: 7.5 mg/kg up to 320 mg) intravenous, daily for seven days (monitor plasma concentration) |
Children 1 month to
8 years |
Trimethoprim + sulfamethoxazole |
5 + 25 mg/kg orally, 12-hourly for six weeks |
| Plus gentamicin† |
7.5 mg/kg up to 320 mg intravenous, daily for seven days (monitor plasma concentration) |
| If gentamicin is contraindicated or relevant precautions preclude its use, replace gentamicin in the above regimens with: |
| |
Rifampicin‡ |
600 mg (child: 15 mg/kg up to 600 mg) orally, daily for six weeks |
*In adults, use ideal body weight to calculate dose if body weight is more than 20% over ideal body weight
†In children, use ideal body weight to calculate the dose unless actual body weight is lower
‡Rifampicin: check for any drug-related interactions prior to prescribing |
Public health aspects
Brucellosis is a notifiable condition in humans in all states and territories of Australia. Travellers to endemic countries should be advised to avoid consuming unpasteurised dairy products and having unprotected contact with animal tissues, blood and other body fluids.22
Feral pig hunting is the main risk for locally acquired infections in Australia; therefore, reducing risk to the public focuses on safer hunting practices. Using waterproof dressings to cover cuts and abrasions, wearing eye protection and boots that can be cleaned and disinfected, and using good lighting and taking time to safely dress feral pigs in the field, are some of the steps that can be taken by hunters to reduce the risk of exposure.23,24
Pig-hunting dogs are also at high risk of acquiring infections from feral pigs, and can potentially pass on the infection to other dogs and humans.25 Hunters can reduce the risk of transmission by not feeding raw feral pig meat or offal to dogs, and by washing dogs (using appropriate personal protective measures) after each hunt.26
The extent to which infected dogs present an ongoing risk to household members is unclear but thought to be very low. The critical window in terms of transmission from dogs to humans is thought to be when a female dog is giving birth. Breeders should be advised to wear gloves and a mask when assisting birthing procedures, especially if handling aborted fetuses. Hunters and breeders with further questions about managing risk of brucellosis in dogs should be referred to a veterinarian.
While there are no vaccines for humans or dogs, several licensed live Brucella vaccines are available for use in livestock throughout the world, such as the B. abortus strain 19 used in the bovine Brucella eradication campaign in Australia.
Key points
-
Brucellosis is acquired through direct contact with tissues and fluids from infected animals. Overseas, brucellosis is also acquired through consumption of unpasteurised dairy products.
-
Brucellosis should be suspected in all patients with non-specific, flu-like illness who participate in feral pig hunting (B. suis) or who have a history of travel to, or residence in, countries where B. melitensis/abortus occur in animals.
-
Serology and blood cultures are the mainstay of diagnosis in acute presentations. Blood cultures are more useful than serology in relapsing cases, while imaging and biopsy are often required for diagnosis of focal suppurative infections.
-
Early diagnosis and treatment is important for limiting duration and preventing complications. Dual therapy with doxycycline and gentamicin is the recommended treatment for brucellosis. Relapse can occur despite appropriate treatment.
-
Brucellosis is a notifiable condition in all states and territories.
-
If a hunter is diagnosed with brucellosis, consider referring them to a veterinarian so their dog(s) can be tested.