Indwelling catheters (IDCs) are common devices used for urinary drainage. Nursing staff are often responsible for basic IDC management, with escalation to doctors when complications arise. However, the literature has shown that IDC insertion and management is poorly taught in medical schools and to junior medical staff.1 Limited exposure to IDCs in formative years and reliance on specialist nursing care poses a risk of de-skilling doctors. As a result, patients present to emergency departments unnecessarily or are placed on long specialist outpatient clinic waiting lists when most IDC-related problems can be adequately managed without specialist input.2
Indications for catheterisation
To prevent complications, catheters should be used only when clinically indicated.3 Initially, the least invasive form of catheterisation should be chosen and only advanced once a method is no longer appropriate.
Intermittent ‘in and out’ urethral catheterisation
Indications for intermittent catheterisation include relieving urinary retention, drainage of post-void residual urine, urethral stricture dilatation and obtaining sterile urine specimens. Individuals with certain neurogenic or detrusor muscle dysfunction may have regular self-catheterisation regimens. Depending on the indication, self-catheterisation can vary in frequency from weekly to multiple daily insertions. These patients require adequate knowledge and competency to safely perform self-catheterisation.4 Education and assessment can be obtained from continence nurses and doctors specialising in urinary issues.
Indwelling urethral catheterisation (short term and long term)
Short-term IDCs are commonly used in hospital for management of acute urinary retention (AUR), urine measurements, bladder irrigations, diversion and drainage of urine after surgery, or for patients requiring epidural anaesthesia.4 Individuals presenting with AUR may require an IDC to remain in situ for several days before attempting a voiding trial. This allows the bladder to regain its tone before attempting a voiding trial. Multiple failed, appropriately timed, voiding trials warrant specialist referral.
Long-term IDC should be avoided and is not a substitute for nursing care for incontinence management. In rare situations, when a suprapubic catheter (SPC) is contraindicated and other methods have failed, a chronic IDC may be needed.4 Safe community practice ensures IDCs are changed every 4–6 weeks. Scheduled IDC changes may vary according to individual needs. However, IDC changes should never persist beyond three months.
Suprapubic catheterisation
In hospital, short-term suprapubic catheterisation is used for AUR management when other methods have failed or for lower urinary tract diversion after surgery or trauma.4–6 In these situations the SPC is a temporary measure. Once efficient urethral drainage is achieved, the SPC can be removed and the fistula will promptly close. Long-term suprapubic catheterisation is needed when urethral catheterisation is no longer feasible or in certain neurological diseases.4,6 Compared with IDCs, SPCs are easier to clean and change, less likely to block, do not cause urethral erosion, maintain sexual function and reduce enteric microorganism contamination.7 A new suprapubic tract takes 10 days to four weeks to become established. Most institutions wait six to eight weeks before changing a newly inserted SPC. After this time, SPCs are typically changed routinely every four to six weeks.8 An SPC should be replaced immediately once it has been removed, as the suprapubic tract closes rapidly.
Patients with permanent catheterisation are at increased risk of bladder stones and bladder cancer. They require annual bladder ultrasonography and serum renal function investigations. They may also require ongoing urological review and cystoscopy surveillance.
Contraindications for catheterisation
IDCs are contraindicated in patients with abnormalities of the urethra, including false passages, severe strictures, injury or tumour.4 Pelvic injury associated with meatal blood, boggy prostate or perineal haematoma is highly suspicious for urethral injury, and specialist input should be sought before catheterisation. More caution should be undertaken in patients self-catheterising with a urinary tract infection.
SPCs are contraindicated when patient factors increase the risk of trauma or infection with insertion. These factors include coagulopathy, bladder carcinoma, pregnancy, ascites, severe obesity, large ovarian cysts, lower abdominal scar tissue, mesh or adhesions from previous surgeries, pelvic cancer or radiation treatment.4,6 Bladder and prostate cancer seeding along the cystotomy tract is also a potential risk.
Types of catheters
All Australian catheters must conform to Australian safety standards.9 Common catheter materials include polyvinylchloride (PVC), latex and silicone.4 The straight Nelaton catheter is a common, single-use PVC product used for intermittent catheterisation.4 Short-term IDCs are usually made of latex or silicone. Latex IDCs are not routinely used because of allergy risk. However, in the absence of allergy there is no difference in the incidence of urinary tract infections.4 Silicone catheters have larger internal diameters, are usually clear and have been associated with reduced rates of bacterial colonisation. Long-term use is associated with a lower risk of urethritis and urethral strictures, making them the preferred material.4
Catheter coatings were intended to reduce trauma and infections.7 Evidence supporting hydrogel, silver-coated or antibiotic-impregnated catheters is limited.4,8 However, there is a growing trend towards hydrogel catheter use in Australia for self-catheterisation and long-term IDC. Hydrogel catheters become smoother when wet, which reduces urethral friction.10 Some studies have shown that hydrogel IDCs can be left in situ for 12 weeks without complications.10
Catheters have one to three lumens. Single-lumen catheters are hollow tubes allowing unidirectional flow, and are used for intermittent catheterisation and sterile urine collection.3 Double-lumen catheters have an inflatable retention balloon in one channel while facilitating urine drainage in the other channel.3,4 Triple-lumen catheters use a retention balloon in one lumen and allow for bi-directional irrigation in the other two lumens. Triple-lumen catheters are used for bladder irrigations to remove pus, clots and thick fluids from the bladder.4
Catheter size is measured by the external diameter and expressed in French gauge (Fg or Fr; 1 Fr = ⅓ mm). The correct size is determined by patient characteristics, type of fluid drained and indication for insertion.
3 Generally, the smallest appropriate gauge should be selected to prevent urethral erosion or stricture formation.
3 Catheter lengths vary for adults and children (Figure 1).
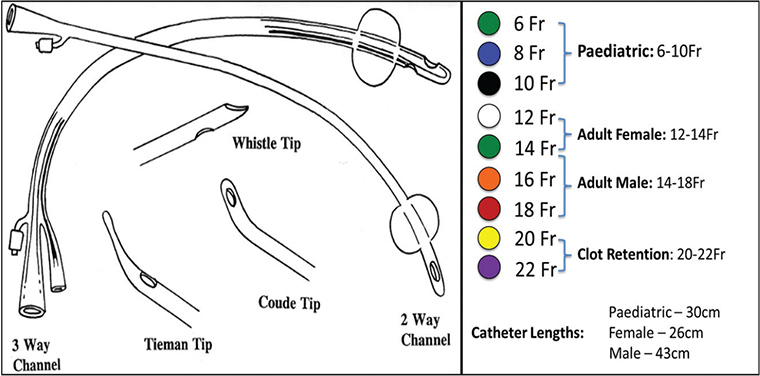
Figure 1. A summary of catheter tips, sizes and lengths4
Catheter tips vary in shape. Tip selection is guided by the indication for insertion and anatomical factors. Standard catheters have a rounded tip and a draining distal lateral opening, allowing easy insertion and drainage of clear urine.4 Whistle-tip catheters have an open, bevelled end that improves drainage of viscous fluids but poses increased risk of urethral trauma on insertion.4 Coudè and Tieman tip catheters are rounded catheters with an angulated tip. Both catheters are useful for males with enlarged prostates, high bladder necks and urethral strictures.4 Open-ended catheters result in less bladder mucosal irritation and may be useful for long-term catheterisation.11
Complications of catheters and management
Complications are reduced when catheters are inserted only when indicated and remain in situ for the minimum time required (Table 1).4,12 Catheter-associated urinary tract infections (CAUTIs) are the most common complication of catheterisation and frequently account for presentations to general practice or the emergency department.13 To a lesser extent, catheter blockages and catheter bypassing are other common emergency department presentations.2
| Table 1. Advantages and disadvantages of different types of catheterisation |
| Type |
Description |
Advantages |
Disadvantages |
| External catheters |
Devices adhering to the external genitalia; commonly referred to as ‘urodome’ or ‘condom catheters’ |
- Reduced incidence of bacteriuria, UTI, pain, or death compared to IDCs
- Increased safety and comfort, especially in delirious and demented patients
- Practical option for incontinent elderly males where IDC is not appropriate
|
- Tissue damage to penile shaft with incorrect placement
- Inadequate bladder drainage capacity
- Only male products commercially available
|
| Intermittent catheters |
A straight, hollow PVC tube inserted via the urethra and removed post-void. |
- Less impact on mobility, independence and body image
- Reduced incidence of CAUTI
|
- Only used in competent patients
- Increase incidence of urethral trauma with multiple insertions
- Compared to IDCs, reduced efficacy for treating urinary retention
|
| Indwelling catheters |
Double or triple lumen catheter, held in situ via inflation of a balloon with sterile water; commonly referred to as a 'Foley cathete'r |
- Able to remain in situ for 1–12 weeks
- Generally efficient and accepted treatment of urinary retention
|
- Highest incidence of CAUTI compared to other methods of catheterisation
- Risk of urethral and bladder neck injury on insertion or removal, due to balloon
- Self-extraction risk in demented and delirious patients
|
| Suprapubic catheters |
A double lumen catheter enters the bladder through a surgically formed tract through the abdominal wall |
- Can remain in place for 2–3 months at a time
- Ability to use a catheter valve as an alternative to free drainage when urine storage within bladder is acceptable
|
- Contraindications to insertion include coagulopathy and abdominal wall infection
- Potential risk of abdominal organ injury and peritonism
- Requires prompt access to a urology service in case of complications
- Difficult insertion and maintenance in obese individuals
- Patients may continue to leak urine via urethra
|
| CAUTI, catheter-associated urinary tract infection; IDC, indwelling catheter; UTI, urinary tract infection |
Infections/colonisation
CAUTIs are the most common nosocomial infection worldwide.4 Of healthcare-associated urinary tract infections, 80% occur in catheterised patients, resulting in increased morbidity, mortality and length of hospital stay.14 CAUTI incidence is reduced by appropriate placement and care of catheters. This includes ensuring insertion is indicated, using aseptic technique, implementing good hand hygiene when handling catheters, maintaining a closed drainage system, ensuring patients are adequately hydrated and providing timely removal.4,14
In patients with a long-term IDC, bacterial colonisation of the urinary tract is progressive and 95% of catheterised patients will have bacterial colonisation at four weeks.15 CAUTIs are defined by the presence of bacteriuria and simultaneous symptoms, including generalised malaise, malodorous urine, urinary colour change and systemic signs of illness.16 Antibiotic therapy should be reserved for patients with symptomatic infections and guided by culture sensitivity to prevent antibiotic resistance.15,16 If a CAUTI is suspected, the IDC should be changed while under antibiotic coverage.
Catheter obstruction
Accumulation of blood clots, crystals, tissue and biofilms can cause obstruction. Urinary retention causes discomfort, increases infection risk, causes autonomic dysreflexia in patients with spinal cord injuries and chronically results in permanent bladder dysfunction from detrusor overstretching.6,17,18 Promoting diuresis through adequate hydration prevents obstruction.4,18 Manually flushing a catheter with sterile normal saline can relieve obstruction. If unsuccessful, the blocked IDC should be removed and replaced immediately.17 Larger catheters with irrigation channels may be required. For instance, >20Fr IDC and bladder irrigations are necessary for clot obstruction.
Catheter bypass
Urine bypassing a catheter occurs for various reasons. These include small IDC size, under-inflated retention balloon, constipation, obstruction and bladder spasms. Bladder spasms are sudden involuntary contractions of the detrusor that result in lower abdominal pain, intense urgency and, potentially, urinary bypass in a neurologically intact individual. Removing a catheter usually eliminates bladder spasms, but when not possible, anticholinergic agents (oxybutynin) or β3-agonists (mirabegron) are needed.17 Prevention of constipation through a bowel care regimen also prevents catheter complications, including leakage and obstruction.4
Trauma
Urethral, prostate or bladder neck injury resulting in false tracts, strictures and bleeding are related to traumatic urethral insertion.4 For correct catheter insertion, refer to Figure 2. Traumatic injury is less likely to occur with appropriate catheter selection, lubrication, correct patient positioning and insertion into a full bladder. Retention balloons should only be inflated inside the bladder, which is indicated by urine return with IDC inserted to the hilt. If there is any uncertainty regarding catheter placement, the balloon should not be inflated. If the patient experiences pain with inflation, deflate the balloon immediately and reassess IDC position as this may indicate the catheter is outside the bladder. IDCs should be used with caution in patients at risk of self-extraction, such as those with dementia or who are delirious. When available, ultrasonography is recommended to evaluate bladder volumes and guide SPC insertions.4,6 Urethral erosion occurs more commonly with catheters of larger gauge, prolonged tension or use.4
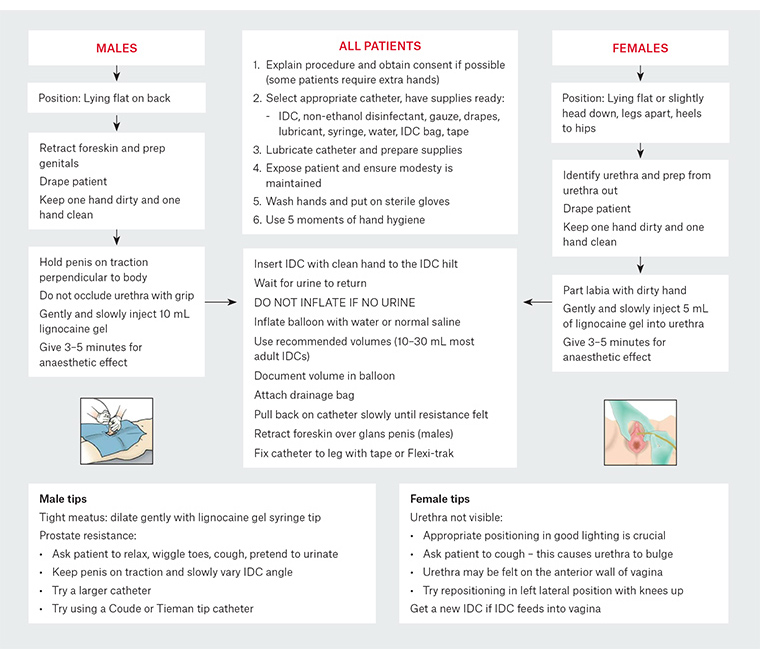

Figure 2. Appropriate catheter insertion in male and female patients
Images reproduced with permission from Michael D'Alessandro, from Bergman R. Bladder catheterization. Anatomy Atlases, www.anatomyatlases.org/firstaid/BladderCatheterization.shtml
IDC, indwelling catheter
Referral to the emergency department or urologist
Hospital referral should be made if specialist input is required. This includes instances where catheter removal or re-insertion is unsafe or difficult, perforation is suspected and visualisation of the urinary tract is required. Specialist input should also be sought for sepsis or CAUTIs unresponsive to oral antibiotics, ongoing and uncontrolled bleeding, recurrent catheter obstruction and inadequate pain management.
Conclusion
Appropriate knowledge and experience of catheter management and associated complications by general practitioners reduces the impact on acute-care facilities. Many issues related to catheters can be safely and adequately managed in the community, resulting in timely management and increased patient satisfaction. Emergent specialist input should be reserved for patients in whom basic measures are unsuccessful or where further harm or life-threatening complications are suspected.
Key points
-
Use the least invasive method when a urinary catheter is clinically indicated.
-
IDCs come in various shapes, lengths, diameters and materials.
-
Catheter-related complications are prevented when appropriate handling and insertion technique is used and when catheters remain in situ for the minimum time required.
-
Common catheter complications include infection, obstruction, urine leakage and genitourinary tract trauma.
-
Catheter-associated urinary tract infections are the most common nosocomial infection worldwide.
-
Most catheter-related complications can be adequately managed in the community.