Case
A girl aged seven years presented with a three-year history of an indurated longitudinal plaque on her left shoulder, extending down her posterior arm. A second plaque was present in her left antecubital fossa (Figures 1, 2). The skin change was well demarcated and not tender. The surrounding skin appeared pinched. The lesion had been previously diagnosed and treated as dermatitis and a fungal lesion, with no improvement. There was no significant antecedent or comorbid pathology. She had otherwise been well.
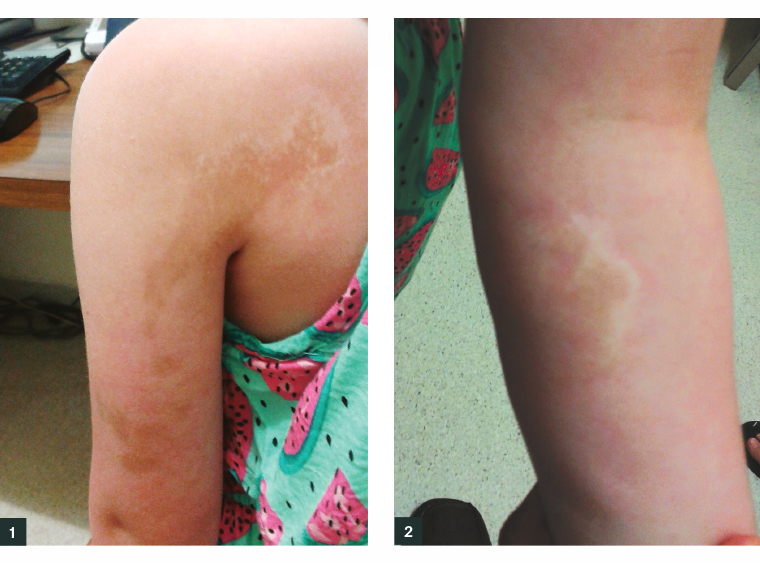
Figure 1. Linear scleroderma (morphea) present over the posterior shoulder and down the upper arm
Figure 2. Circumscribed (plaque) morphea present over the anterior cubital fossa
Question 1
What is the most likely diagnosis?
Question 2
How does the diagnosed condition typically present?
Question 3
What diagnostic testing is required? What other differential diagnoses could be considered?
Question 4
What is the pathogenesis and aetiology of the diagnosed condition?
Question 5
What management is required for this condition?
Answer 1
This presentation is consistent with linear scleroderma, also known as morphea. This is the most common type of localised scleroderma in children. The lesion over the elbow is consistent with circumscribed (plaque) morphea.
Answer 2
The lesions of linear scleroderma present as fibrotic lesions that are elongated. The direction is usually transverse when on the trunk and longitudinal on the limbs. It may follow the lines of Blashko. On the face or scalp, it is referred to as ‘en coup de sabre’. Circumscribed morphea, the most common form of localised scleroderma, can also be present. The lesions are confined to the dermis with occasional involvement of the superficial panniculus.1
Although scleroderma consists of a spectrum of disorders that can occur at any stage of life, the predominant form of childhood scleroderma is localised. Morphea has an incidence of 1–3 per 100,000 children and is three times more common in females than males.2
Answer 3
Differential diagnoses could include one of the five types of localised scleroderma including:
The features of other differential diagnoses are outlined in Table 1.
Morphea is generally diagnosed clinically. A biopsy of the skin and/or subcutaneous tissue may be useful for confirmation if there is doubt about the diagnosis. This would also help exclude the aforementioned differential diagnoses.
There is no requirement for, or use in, other laboratory testing in morphea.
|
Table 1. Features of differential diagnoses of morphea
|
|
Condition
|
Features
|
|
Non-genital lichen sclerosis et atrophicus
|
Dry, wrinkled and thin skin with prominent hair follicles among bruising and blistering
|
|
Lipodystrophy
|
Subcutaneous fat loss with resulting skin depression and prominent definition of the underlying muscle and bone
|
|
Lupus panniculitis
|
Thickened and firm nodules and plaques, erythematous skin and tenderness
|
|
Atrophoderma of Pasini and Pierini
|
Sharply demarcated, hyperpigmented, non-indurated patches
|
|
Sarcoidosis
|
Non-specific features may include erythema nodosum, nummular eczema, erythema multiforme, calcinosis cutis and pruritus
|
Answer 4
The pathogenesis of morphea remains uncertain. Two contributing processes could include fibroblast function and autoimmune dysfunction. Skin lesions typically show an initial marked inflammatory reaction, followed by matrix deposition (including collagen), fibrosis and, ultimately, atrophy.3 There also appears to be an increased incidence of autoimmune disorders in those affected with morphea and their relatives. A particular cytokine and chemokine profile is also observed, with a T-helper cell type 1 (associated with interferon-gamma) and type 17 (associated with interleukin 17A) predominance.4
Answer 5
Treatment is usually required in linear scleroderma to avoid the following complications:5
-
atrophy of soft tissue muscle, periosteum and bone
-
extensive and disfiguring growth defects in either all or part of an affected limb
-
flexion contractures in lesions that cross joint lines
-
hammer toes or claw hands if toes or fingers are involved
-
fixed valgus or varus deformities from leg-length inequalities if these are involved.
One in four children with localised scleroderma will develop extracutaneous manifestations during the course of their disease, including, among others, arthritis, focal neurological deficits and vascular findings (eg vasculitis rash and deep vein thrombosis).
Non-pharmacological treatment includes measures such as physiotherapy and massage to maintain functional ability, muscle strength and joint movement. Topical treatment includes use of emollients and low-concentration topical corticosteroids to relieve dryness and itching. Systemic measures include the use of methotrexate where there is a risk for significant disability.6
Given the potential consequences of morphea and the nature of treatment required, timely referral to a specialist paediatric dermatologist or unit is recommended for children suspected of having morphea.
Case continued
The patient was commenced on methotrexate because of the location of the lesion on her upper limb and involvement of the elbow joint. No new lesions have occurred. Treatment is ongoing, with progressive improvement and reduction in size of the lesion.
Key points
-
The predominant form of scleoderma in childhood is localised scleroderma.
-
Localised disease principally involves the skin, subcutaneous fascia, muscle and bone. A quarter of patients will have extracutaneous findings.
-
The diagnosis is primarily clinical, although biopsy can help confirm the diagnosis.
-
Treatment is individualised, matched to the type and stage of disease.