Case
A girl aged 2.5 years presented to her general practitioner (GP) with a firm lump on her left jaw. The child had not noticed any change; however, her mother had noticed a swelling over the past week with no antecedent trauma. The patient did not complain of pain, mastication or airway compromise, paraesthesia or abnormal facial movements. She had a genetically confirmed past medical history and family history of familial adenomatous polyposis (FAP). She did not taken any medications and had no other social or medical history.
Clinically she had a firm immobile swelling of the left mandibular body measuring 12 × 9 mm with no soft tissue induration or skin changes. Her cranial nerve examination was normal. Her deciduous dentition had no caries, mucosal changes, intra-oral swellings or lymphadenopathy. The floor of the mouth and palate was normal. Her other systems were unremarkable.
Question 1
What differential diagnoses should be considered?
Answer 1
Initial examination should first exclude lymphadenopathy. Other considerations should include lymphoma, soft tissue and other extraosseous sarcomas such as rhabdomyosarcoma and osteosarcomas, and malignant bone tumours. Primary jaw lesions can be classified into odontogenic cysts (epithelium produced during tooth development) and non-odontogenic cysts (arising from facial sutures during embryonic development). Although uncommon in the paediatric population, cysts appear to be more common than in adults.1 Dentigerous cysts are odontogenic cysts that are associated with an unerupted tooth and are the most common paediatric cystic lesion of the jaw.2
Case continued
A posteroanterior radiograph was ordered to visualise the lesion (Figure 1). The patient was referred to a tertiary centre and underwent a multidisciplinary assessment that included a review of medical, dental, allied health and surgical disciplines, and confirmed the diagnosis of desmoid tumour.
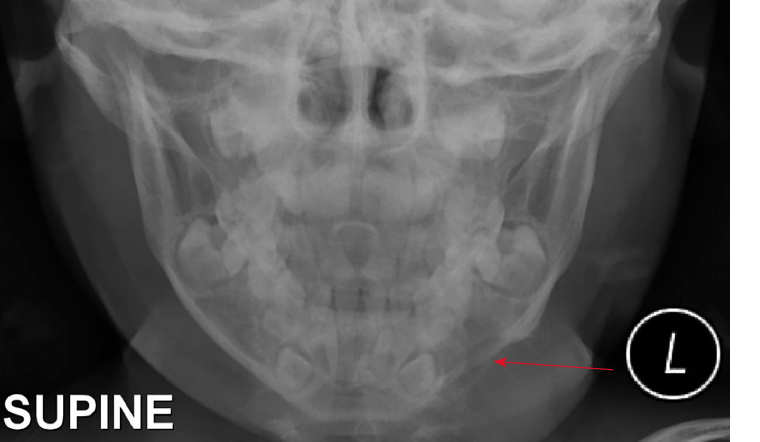
Figure 1. Posteroanterior radiograph demonstrating translucent lesion of the left body of mandible involving the tooth germ
Question 2
What is the natural history and aetiology of desmoid tumours?
Question 3
How is this condition diagnosed?
Question 4
What is the appropriate management of this condition?
Question 5
What is the prognosis for this condition?
Answer 2
A desmoid tumour is a soft tissue tumour often arising from musculo-aponeurotic structures that has a tendency for local invasion rather than metastasis.3 Often associated with genetic mutations such as adenomatous polyposis coli, it can manifest intra-abdominally and extra-abdominally from the extremities, head and trunk.4 Desmoid tumours are extremely rare and present with two peaks: age 6–15 years and 40 years.5
The patient had a familial inheritance of FAP, which was a key component in the differential diagnosis and workup. Other known factors include trauma, genetic predisposition and endocrine factors related to hormonal changes.
Answer 3
Classically, a patient may present to the GP with a painless enlarging mass. Before referral, initial ultrasonography can identify soft tissue or bony involvement. An orthopantomogram may also be a useful initial radiological tool (Table 1), but interpretation and official reports may delay diagnosis. Therefore, investigations should be swiftly coupled with referral; specialist advice should be sought early via referral to a local paediatric oromaxillofacial or plastic surgeon for comprehensive multidisciplinary assessment, further investigations such as computed tomography or magnetic resonance imaging and biopsy.
|
Table 1. Key radiological findings to consider in differential diagnosis on an orthopantomogram8
|
|
Lesions
|
|
Radiological key findings
|
|
Odontogenic cysts
|
Radicular cyst
|
Associated with a non-vital tooth
Occur around the root apex
|
|
|
Residual cyst
|
Dentition has been extracted
Centred above the mandibular canal
|
|
|
Dentigerous cyst
|
Associated with the crown of an unerupted tooth
Attaches at the cemento-enamel junction
|
|
|
Lateral periodontal cyst
|
Small, <1 cm
Arise on the lateral portion of the root
|
|
|
Odontogenic keratocyst
|
Commonly around posterior mandibular body and ramus, centred above the mandibular canal
May be associated with an unerupted tooth
|
|
|
Gorlin syndrome
|
Usually occur in the posterior body and ramus of the mandible
May be uniocular or septated; may mimic a dentigerous cyst
|
|
Non-odontogenic cysts
|
Nasopalatine duct cyst
|
Midline maxillary cyst
Divergence of the maxillary incisors
|
|
|
Simple bone cyst
|
Almost always mandibular
Smooth border without expansion
|
|
Benign lucent tumours
|
Ameloblastoma
|
Often cause massive bone expansion, tooth displacement and disruption
Unicystic or multicystic
|
|
|
Adenomatoid odontogenic tumour
|
Displaces but does not resorb dentition
May have subtle or popcorn-like internal calcifications
|
|
|
Odontogenic fibromyxoma
|
Straight internal septae are characteristic
Scallops alveolar bone between teeth
|
|
Malignant lucent tumours
|
Mucoepidermoid carcinoma
|
May appear as radiologically innocent lesions
Unilocular or multilocular appearance with jaw expansion
|
|
|
Multiple myeloma
|
Multiple punched-out lucencies
Coalescent lesions may appear destructive
|
|
|
Fibrosarcoma
|
May be radiographically occult: check the mandibular canal
Ill-defined lesions without a clear margin
|
|
|
Metastatic tumours
|
Poorly defined lytic lesions
Frank bone destruction
|
|
|
Squamous cell carcinoma
|
Ill-defined lesions with bone destruction
Only arise in tooth-bearing areas of the jaws
|
|
Miscellaneous
|
Fibrous dysplasia
|
Ill-defined margin with a ground glass appearance
The only lesion that can displace the mandibular canal superiorly
|
|
|
Neurofibroma
|
Lucent expansion of the mandibular canal
|
|
|
Stafne defect
|
Below the mandibular canal, anterior to the angle of the mandible
Densely sclerotic margin
|
|
|
Eosinophilic granuloma
|
Poorly defined mandibular radiolucency
|
|
|
Giant cell granuloma
|
Well defined, radiolucent lesions in the anterior mandible
May appear more sinister in the maxilla
|
|
|
Xanthoma
|
Poorly defined mandibular radiolucency
|
Answer 4
In general practice, early investigation and swift referral with any doubt of a jaw lump is fundamental to diagnosis and long-term management of a growing child’s face. The mainstay of treatment for desmoid tumours is surgical resection with clear margins. These heterogeneous lesions are locally aggressive, with varying biological behaviour. The treatment can be complex, requiring a multidisciplinary team across disciplines. The adjuvant role of chemotherapy, radiotherapy and hormonal receptor therapy has been considered in unresectable, recurrent or progressive cases.6 However, the toxicity profile for these therapies poses its own specific complications and high morbidity. The patient in this case study underwent a multidisciplinary assessment for a wide surgical resection with a fibular flap. She had clear margins and has regular follow-up.
Answer 5
The literature from large trials is sparse, but the overall prognosis is good if detected early in disease progression. Early detection and referral by GPs is crucial and has an impact on the time taken to investigate and operate, with known recurrence rates ranging from 19% to 50% after primary resection.7
Key points
-
Bony lesions of the jaw in children can present nonspecifically, but they can be rapidly aggressive in the growing face.
-
A comprehensive history, examination and appropriate investigations can help with differential diagnoses.
-
Children require urgent referral to a local oromaxillofacial or plastic surgeon for multidisciplinary management.