Case
A previously healthy man, Caucasian, aged 52 years, presented to a dermatology clinic with an asymptomatic subcutaneous nodule located in the right temporal area, near the hair implantation line. The lesion was first noted by the patient approximately three months prior and had grown progressively in size. There was no history of local trauma.
Physical examination revealed a tender nodule, approximately 3 cm in diameter, with a smooth surface and normal overlying skin, not adherent to the deeper planes.
Question 1
What differential diagnoses should be considered in this patient?
Question 2
What is the most likely diagnosis at first evaluation?
Answer 1
The main conditions to consider in the differential diagnoses of this type of lesion are listed in Table 1. Other conditions to be taken into account include ossifying haematoma, chondroma, dermoid cyst, degenerating fibroxanthoma, metastatic bone formation and osteoma cutis.1
| Table 1. Main diagnoses to be considered in the setting of a nodule in the forehead1,10,11 |
| Disease |
Clinical differentiating features |
| Epidermal cyst |
Compressible not fluctuant cystic mass, with overlying skin usually smooth and shiny. A surface punctum is often present, which attaches the lesion to the skin. It is rare before puberty. |
| Pilar cyst |
Second-most common cyst occurring in the head and neck. Usually its content is homogeneous, with tender consistency at palpation. Frequently it can calcify and rarely ossify. Its location can be subcutaneous or intradermal. It is uncommon in young people. |
| Pilomatrixoma (calcifying epithelioma of Malherbe) |
Firm to hard papule, nodule or dermal plaque, usually painless, mobile and superficial, with variable size (usually 0.5–5 cm in diameter). It may be faceted on palpation or have a characteristic ‘shelf-like’ feel, possibly due to calcification. The overlying skin may be normal or have a bluish-red discoloration, and may present atrophy resembling anetoderma or striae. |
| Foreign body reaction |
A granuloma can develop, which may acquire different aspects, depending on the extension and type of inflammatory response.
It is a response to an irritation to the skin caused by endogenous or exogenous materials. It may present as a papule or a nodule. |
| Dermatofibroma |
Predilection for lower extremities, being rare in the scalp and face. It is a round or oval firm dermal nodule, usually small (approximately 1 cm) and dusky brown in color. A surrounding eczematous halo may be present. |
| Lipoma |
More common in the neck than in the scalp or face; a deep variant arising in the forehead has been described. Typically it is soft, mobile and encapsulated. |
Atypical fibroxanthoma
(AFX) |
Low-grade malignant lesion, common in sun-exposed parts of the head or neck in Caucasian people aged >50 years. Clinically it begins as a small, firm, solitary nodule, gray to pink/red in color, often dome-shaped and with an eroded or crusted surface without characteristic morphologic features. |
| Malignant fibrous histiocytoma (MFH) |
Most common soft tissue sarcoma of middle and late adulthood. Clinically resembles AFX, which is smaller and more superficial in the dermis, compared with the deeper location of MFH. Its prognosis is poor. |
| Squamous cell carcinoma |
More common in middle-aged adults. It usually has an indurated, rounded and elevated base, frequently with telangiectasia; in advanced stages, varying degrees of ulceration, crusting and adherence to underlying tissues are verified. Concomitant actinic keratosis lesions are common. |
| Merkel cell carcinoma (MCC) |
Usually arises on the sun-exposed skin of elderly patients, particularly on the head, neck and extremities. Clinically, it presents as a rapidly growing, nontender, red to violaceous nodule with a shiny surface and overlying telangiectasia. Although rare, MCC is an aggressive tumor with a propensity for local recurrence and nodal and distant metastases. |
| Rhabdomyosarcoma (RMS) |
A primary cutaneous presentation occurs in less than 1% of all
RMS. Cutaneous RMS has a bimodal age distribution, involving
children/teenagers and older adults. This lesion is usually a solitary, rapidly enlarging, firm mass that involves the striated muscle. Tumour margins are poorly defined. |
Answer 2
Despite its rapid growth, at first evaluation the lesion is suggestive of pilar cyst, due to the absence of symptoms, usual and superficial location, homogeneous tender consistency, absence of punctum, normal overlying skin, well-defined aspect and absence of excessive cumulative sun-exposure stigma.
Case continued
When the patient presented again to the clinic four weeks later, the lesion’s characteristics had changed significantly, with a 2 cm maximum diameter, lobulated surface and hard density (Figure 1A). Despite the defined limits and good mobility of the lesion at first observation, the decision was made to perform an excisional biopsy of the nodule in light of its fast growth.
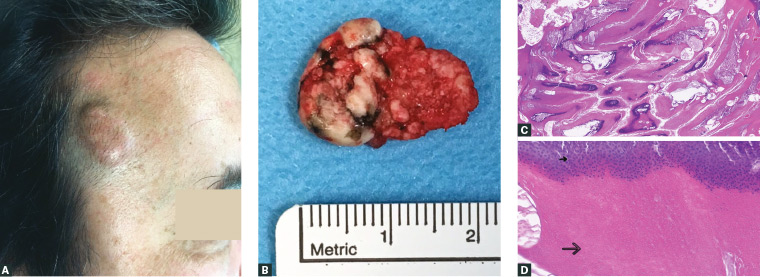
Figure 1. Different aspects of the lesion
A. Clinical appearance; B. Macroscopic aspect of the excised lesion; C. Microscopic aspect: peripheral layer of basaloid cells; central multiple nests of mummified ghost/shadow cells, some with calcification of the adjacent stroma (Haematoxylin and eosin [H&E] x4); D. Microscopic aspect: abrupt transition between basaloid cells layer (small arrow) and eosinophilic ghost cells (large arrow; H&E x100)
Question 3
What is now the likely diagnosis?
Question 4
What are the etiology, epidemiological features and most common locations of this type of lesion?
Question 5
How is this condition diagnosed?
Question 6
What is the appropriate management of this condition and the expected prognosis?
Answer 3
The evolution and clinical appearance are suggestive of pilomatrixoma, also known as pilomatricoma and calcifying epithelioma of Malherbe.2 Pilomatrixoma is a rare, benign appendageal tumour derived from hair matrix cells with calcification phenomena inside,3 giving it a stony touch at palpation.2 Figure 1B shows the macroscopic aspect of the excised lesion, clearly denoting hard consistency and calcified aspect.
Answer 4
Somatic mutations in the CTNNB1 gene, leading to loss of regulation of the protein complex b‑catenin/LEF-1 (involved in hair follicle development), are found in most isolated pilomatrixomas.4 Rarely, they occur in people with genetic disorders such as myotonic muscular dystrophy (associated with multiple and recurring lesions) and Gardner, Turner, Kabuki and Rubinstein–Taybi syndromes,5 but characteristic features of those conditions are usually present. Multiple familial pilomatrixomas inherited in an autosomal dominant pattern and with no demonstrable underlying association have also been reported.6
Pilomatrixoma accounts for 20% of all hair follicle–related tumours.7 They are more common in females (F:M ratio = 3:2)7 and in the first two decades of life, but a bimodal age distribution with a second peak in the sixth decade occurs,2 with increasing recognition in adults.3 The head, neck or proximal upper extremities are frequent locations, but they can also develop on the trunk and lower extremities.5
Answer 5
A diagnosis of pilomatrixoma is usually suspected on physical examination (Table 1). Two characteristic signs help identification:
- ‘tent’ sign – multiple facets and angles that become evident when the covering skin is stretched5
- ‘skin crease’ sign – a central longitudinal crease, perpendicular to the skin tension lines, only evident when the lesion is gently pinched.3
Specialised tests may help in confirmation and differential diagnosis. Ultrasonography usually reveals a well-demarcated lesion, with central punctate hyperechoic images (corresponding to calcification), a thin hypoechoic rim (representing the connective-tissue capsule) and posterior shadowing.8 Cytological evaluation may lead to misdiagnosis, because abundant basophilic cells may be interpreted as carcinoma.9
Its similarity with other conditions and low incidence make pilomatrixoma’s diagnosis a clinical challenge for most physicians, and frequently drives histological examination for diagnostic confirmation.2
Answer 6
Pilomatrixomas are not aggressive lesions. However, occasionally they grow to giant size, and malignant transformation has been reported. Recommended management is surgical excision, with margins of at least 1–2 cm to prevent recurrence.1
Case continued
Following excision, histology confirmed the diagnosis of pilomatrixoma (Figures 1C and 1D).
One year after surgical removal, the patient remains recurrence free and with excellent cosmetic outcome.
Key points
- When a subcutaneous nodule resembles an epidermal or pilar cyst, but has petrous consistency, faceted surface on palpation, ‘tent’ or ‘skin crease’ signs, or a calcified component on radiological examination, pilomatrixoma should be considered.
- The suspicion should be greater in a child or adolescent, given this lesion is more frequent at these ages, and the occurrence of epidermal cysts is rare.
- In fast-growing lesions or nodules with dubious aspects, biopsy should be considered, given the possibility of a malignant condition.