While there are many reasons for radial wrist pain, De Quervain’s tenosynovitis is a common pathology and is described as stenosing tenosynovitis of the tendons within the first dorsal compartment of the wrist.1 The prevalence of De Quervain’s tenosynovitis in adults of working age (18–65 years) in the general population is approximately 1.3% of women and 0.5% of men, with peak prevalence at the age of 40–60 years.2
Aetiology
While the exact cause of De Quervain’s tenosynovitis is still debated, possible aetiologies include acute injuries (eg blunt trauma, biomechanical compression), forceful repetition of the wrist and thumb leading to increased frictional forces or microtrauma (eg workplace-related activity, actions performed by new mothers), inflammatory diseases, anatomical variations, abnormalities of the first dorsal compartment and, rarely, pathogens.1,3
Pathophysiology
The pathophysiology of De Quervain’s tenosynovitis is generally defined in the literature as a stenosing condition of the first dorsal compartment.1 The extensor tendons are divided into six compartments as they cross the dorsum of the wrist. The first dorsal compartment comprises the extensor pollicis brevis (EPB) and the abductor pollicis longus (APL) tendons. They lie within a closed fibrous sheath or tunnel with a synovial lining3 that is approximately 2.2 cm in length.4 This tunnel lies over the radial styloid and under the extensor retinaculum, which can cause tendon gliding difficulties and entrapment of the tendons when thickening of the sheath occurs.3 Thickening of the tendon sheath and therefore narrowing of the tunnel occurs because of the presence of fibrocartilage, which is a response to the shear and compression forces placed on the tendons. Neovascularisation is also seen in patients with De Quervain’s tenosynovitis. It is important to note that this increase in vascularity in the tendons is not associated with inflammation or tissue repair and is responsible for some of the pain experienced with this condition. Histopathology may also show signs of chronic overuse within the tendon substance resulting in myxoid degeneration.5
Many studies have looked at anatomical variations and at the prevalence of an intercompartmental septum within the first dorsal compartment. The prevalence of a septum ranges from 24% to 91% in the literature.1,6 Many authors link the presence of a septum to an increased likelihood of developing De Quervain’s tenosynovitis and also to the success of different treatment types.1,6 Those with an unidentified septum will not respond as well to corticosteroid injections1,6 because only one compartment tends to be injected.5 Those with a septum will need both compartments surgically released; therefore, it is important to identify the septum pre-operatively.7
Assessment
Patients present with pain and swelling over their radial styloid that is exacerbated with thumb motion and wrist deviation.8 Patients often report difficulties with activities that involve grasping, twisting and lifting.9 Physical examination may reveal tenderness on palpation over the first dorsal compartment;10 if swelling is present, it is usually 1–2 cm proximal to the radial styloid following the course of the EPB and APL tendons.8 Finkelstein’s test, first described in 1930, has long been used by clinicians in suspected cases of De Quervain’s tenosynovitis.11 A positive test will elicit pain along the radial wrist when the thumb is held into flexion across the palm and the wrist is moved into ulnar deviation by the examiner (Figure 1).12 Eichoff’s test is very similar but requires the patient to hold their own thumb into flexion using their other fingers while deviating the wrist into ulnar deviation.9
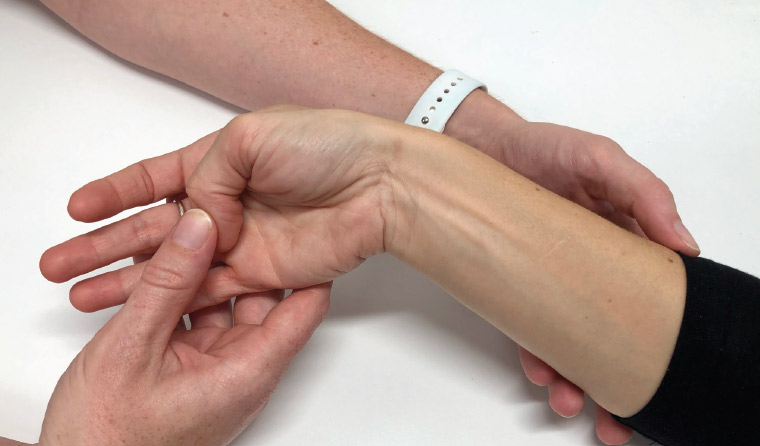
Figure 1. Finkelstein’s test
Pain is caused by the restricted glide of the tendons as they lie in their now narrower compartment.10 The contralateral side should always be assessed, as false-positive results can be seen with this manoeuvre in patients with asymptomatic wrists.9 In their 2010 article, Dawson et al describe a staged approach to Finkelstein’s test,9 which may help to eliminate this. This manoeuvre starts with the patient actively ulnarly deviating their wrist over the edge of a table. In acute presentations this may be enough to elicit pain and the assessment can be halted. If there is no pain, the examiner then passively deviates the wrist. Finally, the examiner passively flexes the thumb across the palm.9 These last two stages can indicate more chronic disease. The authors report the manoeuvre provides an accurate diagnosis while minimising patient discomfort in both acute and chronic cases of De Quervain’s tenosynovitis9 and allows for easy comparison to the contralateral side.
Plain radiographs are not helpful in the diagnosis of De Quervain’s tenosynovitis but may help to rule out other pathologies associated with radial wrist pain.13 Differential diagnosis for De Quervain’s tenosynovitis includes:8,10,12
- intersection syndrome
- osteoarthritis of the first carpometacarpal
- osteoarthritis of the scaphoid-
- trapezoid-trapezium joint
- trigger thumb
- superficial radial nerve neuritis (Wartenberg’s syndrome)
- fractures of the scaphoid or radial styloid.
Ultrasonography has been shown to be highly effective in the diagnosis and treatment planning of De Quervain’s tenosynovitis6 as well as being much more cost effective for patients. Ultrasonography is reported to be useful in reviewing thickening of the tendons and narrowing of the fibro-osseous canal as well as identifying anomalies in tendon slips. Good specificity and sensitivity has been reported with identifying intercompartmental septums with ultrasonography.14 Identification of a septum is important when treatment for De Quervain’s tenosynovitis may include a corticosteroid injection. This will ensure the injection will infiltrate both compartments and increase the chance of symptom resolution without the need to progress to more aggressive forms of treatment.6,8,10
Treatment
Treatment options for De Quervain’s tenosynovitis will depend on the severity of the condition, but non-operative management is preferred. Options for conservative management include prescription of nonsteroidal anti-inflammatory drugs, corticosteroid injections and referral to occupational or hand therapy for fabrication of an orthosis (splint) and further treatment.10
Splinting
Splinting for De Quervain’s tenosynovitis has been found to decrease pain while increasing patients’ ability to continue to participate in activities of daily living.15 Wearing splints will assist by preventing aggravating movements of the thumb and wrist that lead to stenosis of the first dorsal compartment, facilitating rest and recovery.16 The splint must immobilise the wrist and thumb, excluding the thumb interphalangeal joint, in order to offload the APL and EPB tendons. Splints can either be rigid thermoplastic types (Figure 2) or ‘off the shelf’ types made of semi-stiff fabric with metal bars for support (Figure 3). Choosing the type of splint is dependent on the severity of pain and the functional needs of the patient. For example, new mothers with De Quervain’s tenosynovitis will often find it difficult to use a rigid splint.
Splinting regimens also vary depending on the severity of the condition and patient needs. Traditionally, 4–6 weeks of full-time splinting were required. As a result of the non-inflammatory nature of De Quervain’s tenosynovitis, research is now revealing that full-time immobilisation can have detrimental effects on tendon recovery because of the myxoid changes that are present within the tendon substance.15 Splints should not be used in isolation. Other techniques used by therapists include the following:
- Education and activity modification/ergonomics2 have been shown in the literature to be important in the treatment of tendinopathy.5,17
- Soft tissue massage to reduce tight musculature has been shown to decrease pain and promote fluid drainage from tissue.10
- Taping using either kinesiology tape or rigid tape is used during the splint weaning phase or in very mild cases of De Quervain’s tenosynovitis.18 Taping (Figure 4) can also provide proprioceptive feedback and assist with activity modification.
- Graded pain-free active exercises promote gliding of the tendons.10
- Eccentric and isometric exercises are gaining more popularity in the literature, though more studies need to be conducted to show their effectiveness. It is thought that applying controlled stress or load to the muscles and tendons promotes strengthening and healing of the soft tissues.8,10
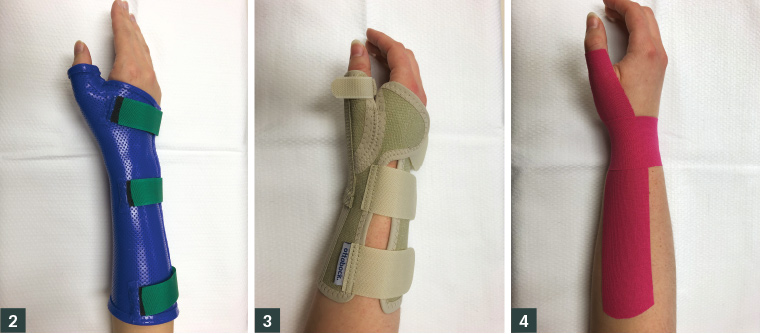
Figure 2. Thermoplastic splint; Figure 3. ‘Off the shelf’ splint; Figure 4. Taping
Corticosteroid injection
Many authors advocate for corticosteroid injections in the treatment of De Quervain’s tenosynovitis.5,8,15,16,19,20
Debate continues in regards to the use of splints post-injection. A Cochrane systematic review in 2009 reported that splinting was not necessary, but it was limited by its inclusion of one study only.20 More recent research has shown that the addition of immobilisation splinting post–corticosteroid injection improved outcomes versus injection alone.5,15,19 The addition of exercises has also been shown to improve longevity of pain relief versus steroid injection plus splinting.10 As previously mentioned, ultrasonography-guided injections are beneficial, especially in the presence of an intercompartmental septum.6,8,10,16 Care should be taken to review the complications of multiple corticosteroid injections with patients. Side effects can include subcutaneous fat atrophy, pain, swelling, bruising and tendon rupture.8,15,21
Surgery
Surgery should be considered for recalcitrant cases that have shown no improvement with conservative measures over a 3–6-month time frame.7 The presence of a septum and multiple tendon slips are known to contribute to failure of non-operative treatment.7 There are many different surgical techniques reported and favoured by different authors. All require the decompression of the first dorsal compartment, some with reconstruction of the compartment to prevent possible subluxation of the tendons.7
Post-surgery therapy can include splinting, scar management including desensitisation, oedema management, active exercises and strengthening.10
Key points
- De Quervain’s tenosynovitis is a stenosing tenosynovitis with multiple possible aetiologies.
- Ultrasonography to determine the presence of an intercompartmental septum is important when planning for treatment.
- Referral to an occupational therapist or hand therapist for conservative management should be considered.
- Splinting should be used in conjunction with corticosteroid injections to improve results.
- There is emerging evidence for the use of tendon loading in non-operative and operative management of De Quervain’s tenosynovitis.