Case
A female aged 60 years presented to her general practitioner (GP) with an atraumatic painful left ankle and overlying rash over the past two weeks. She was feeling systemically well and did not have any other focal infective symptoms. Her medical history included gastro-oesophageal reflux disease and hypercholesterolaemia on long-term esomeprazole and rosuvastatin. She had not commenced any new medications.
On examination, she had a temperature of 38.0 °C but was haemodynamically stable. She ambulated with an antalgic gait due to left ankle pain. There was some mild synovitis of her left ankle, but none in other joints. The petechial and coalescing rash (Figure 1) was non-blanching, mildly tender and palpable. The rest of the clinical examination was unremarkable.
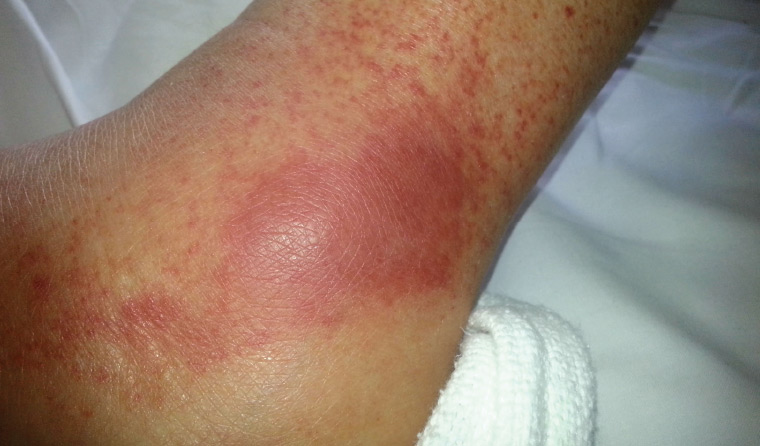
Figure 1. Rash on the lateral aspect of the patient’s left ankle
Question 1
What key diagnoses need to be considered and excluded?
Question 2
What initial investigations are required?
Question 3
What initial management should be considered?
Answer 1
Joint rash/erythema, swelling and fever point to possible infection (eg septic joint, cellulitis). Inflammatory arthritis such as gout should be considered as well.
Other differential diagnoses for the rash include:1,2
- haematological conditions, such as coagulation and platelet disorders
- scurvy
- dermatitis
- venous stasis.
General differential diagnoses for rash and synovitis/arthritis include:3
- vasculitis
- medication reactions
- psoriasis.
Answer 2
Blood cultures and arthrocentesis will need to be considered to help differentiate infectious from inflammatory arthritis. Basic imaging such as an X-ray may be considered to detect late changes of osteomyelitis. Rare causes such as septic emboli may mimic the rash; therefore, appropriate investigations to find the source (eg chest X-ray) can also be considered. Other auxiliary tests may include:
- basic blood tests including a full blood examination, biochemistry profile and inflammatory markers
- urine dipstick to look for evidence of possible infection or glomerulonephritis
- urine microscopy for urinary casts.
Answer 3
Because infection is the most common and likely cause, early antibiotics are recommended after liaising with the appropriate teams (eg orthopaedics). Analgesia should be given.
Case continued
The patient was referred to the emergency department (ED). She has an unremarkable urine dipstick/microscopy and normal chest and ankle radiographs. Blood tests revealed mild lymphopaenia (0.9 × 109/L [reference range: 1.0–4.0 × 109/L]), normal biochemistry and coagulation profiles, a slightly raised C-reactive protein (9 mg/L [reference range: <5 mg/L]) but normal erythrocyte sedimentation rate. Blood cultures were negative.
She was able to weight bear and there was minimal ankle irritability on active movement. This discouraged ED clinicians from pursuing septic arthritis or crystal arthropathy diagnoses, and an aspirate was not performed. A skin punch biopsy was performed; this confirmed leukocytoclastic vasculitis (LCV) and was negative for any microbiological growth. The patient correctly received empirical intravenous antibiotics to cover infection until biopsy confirmation of the diagnosis and exclusion of concurrent cellulitis.
Question 4
What should be done to determine the aetiology of LCV?
Answer 4
Vasculitides can be classified according to size of vessel (small, medium or large) or aetiology (primary or secondary; Table 1). LCV is a classic small-vessel primary vasculitis and is commonly idiopathic;1 however, it may be associated with connective tissue diseases, other primary vasculitides, infections, malignancies (paraneoplastic phenomenon) and medications. As a result, comprehensive history-taking, examination and investigations are needed to explore these other diagnoses. Investigations should include autoimmune and vasculitis serology, and basic infection serology (including hepatitis and human immunodeficiency virus serology).4
Malignancy associated with LCV occurs in less than 5% of cases;5,6 but appropriate age-related investigations for malignancy should be considered, especially when LCV remains refractory to first-line treatments.7
| Table 1. Classification of vasculitides and main clinical manifestations |
| |
Primary |
Secondary |
Main clinical manifestations* |
| Small vessel |
- ANCA vasculitides
- Granulomatosis with polyangiitis (Wegener’s)
- Eosinophilic granulomatosis with polyangiitis (Churg–Strauss)
- Microscopic polyangiitis
- Henoch–Schönlein purpura/IgA vasculitis
- Goodpasture’s disease
- Leukocytoclastic vasculitis
|
- Cryoglobulinaemia
- Urticarial vasculitis (may also be primary)
- Malignancy-associated
- Infection-related
- Medications
- Leukocytoclastic vasculitis
|
- Sinusitis, epistaxis
- Lung haemorrhage
- Palpable purpura
- Haematuria/glomerulonephritis
|
| Medium vessel |
- Polyarteritis nodosa
- Kawasaki disease
- Behçet’s disease
|
- Connective tissue diseases (eg lupus, rheumatoid arthritis)
|
- Mononeuritis multiplex
- Visceral infarction
- Hypertension (renal infarction)
- Myalgias
- Ulcers
- Livedo reticularis
- Skin nodules
|
| Large vessel |
- Giant cell arteritis
- Takayasu’s arteritis
- Primary CNS polyangiitis
|
- Aortitis (various causes)
|
- Strokes
- Limb claudication
- Headaches, blindness
|
*There is marked overlap of clinical manifestations between the vessel size classes – in particular, small and medium vasculitis. These include cutaneous, muscular and neurological manifestations.
ANCA, antineutrophil cytoplasmic antibodies; CNS, central nervous system; Ig, immunoglobulin |
Case continued
The patient received additional testing including a comprehensive autoimmune screen (antinuclear antibodies [ANA], extractable nuclear antigens, anti-double stranded DNA, complement, etc), serum ferritin, serum electrophoresis, cryoglobulin and a comprehensive infectious screen. All studies were normal or unremarkable except for a positive ANA (1:640, speckled), anti-Ro52 positive, positive rheumatoid factor (233 IU/mL [reference range:<14 IU/mL]) and low C4 complement (<0.02 g/L [reference range: 0.1–0.4 g/L]). The patient had no other signs or symptoms to suggest an underlying connective tissue disease.
Question 5
What is the management of LCV?
Answer 5
Most cases of uncomplicated and isolated LCV are self-resolving; however, the first step would be to attempt to elucidate and treat any underlying causes of LCV. Symptoms can be treated by taking simple analgesics, resting and elevating legs. Other first-line treatments include colchicine, dapsone and weaning courses of prednisolone.4,8 Refractory LCV or more extensive organ involvement will need additional immunosuppressants such as azathioprine and methotrexate.4,9 The patient should also be referred to a dermatology, rheumatology or immunology specialist.
Case continued
The patient was commenced on weaning prednisolone (from 40 mg). She responded well, with complete resolution of her symptoms. She was referred to a rheumatology specialist.
Key points
- Although infections such as cellulitis and septic joints are a common and likely cause for ankle pain plus rash, it may be helpful to consider a broad range of differentials in patients with focal signs and rashes.
- As infection and vasculitis may be concurrent, careful consideration is required for the timing of cessation of antibiotics.
- Vasculitis/vasculitic rashes have numerous causes, and possible underlying causes must be considered and investigated.
- A prompt referral to physicians experienced in vasculitis to search for complications and other organ involvement is required.
- LCV is one of the most common forms of vasculitis and may be both primary (idiopathic) or secondary to other underlying causes.
- LCV generally has a good prognosis and may self-resolve.