Humans are social beings; hence, it is not surprising that extended periods of social isolation are so difficult to cope with. The superficial perspective of ‘stay at home and keep yourself safe’ fails to consider the significant potential psychological sequelae and impact on daily life.1,2 Excessive distress, fear, sadness and guilt,1 and escalating interpersonal difficulties3,4 are not uncommon, as are acute stress disorder,5 depressive episodes,4,6 anxiety disorders,6 post-traumatic stress disorder (PTSD)4,7 and suicide.8
Much of the research in this field has emerged from studying the outcomes of isolation (confinement of unwell individuals) or quarantine (confinement of individuals potentially exposed to a contagion) in previous infectious disease outbreaks and research on coping in long-term stressful confinement situations.9,10 In this article, the authors refer to confinement and confinement distress to encompass the psychological impact of quarantine, isolation and social isolation.
Two concepts are critical for the clinician managing confinement distress. The first is that biopsychosocial health – including psychological wellbeing, cognitive performance and physiological responses – are regulated by the environment (Figure 1).11–14 Environmental psychology shows that a confined, static environment leads to hypostimulation and secondary neurocognitive problems such as increased risk of depression.15
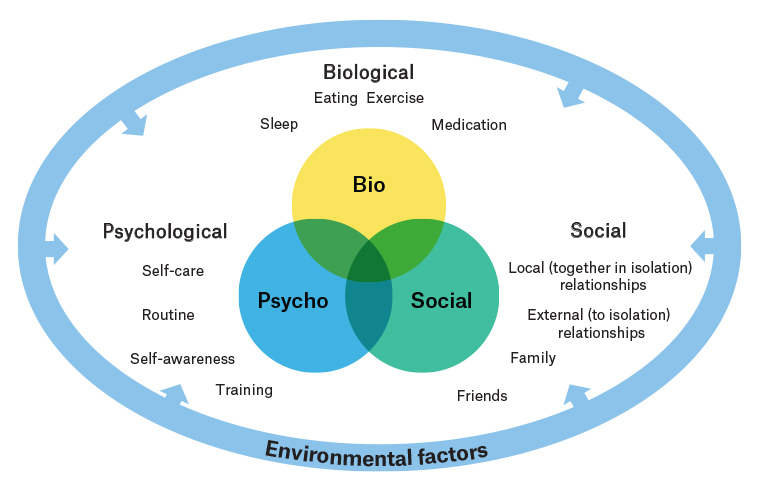
Figure 1. The biopsychosocial–environmental model of health50
Adapted from Engel GL, Romano G, The need for a new medical model: A challenge for biomedicine, Science 1977;196:129–36.
The second concept is the cumulative nature of stress. An individual’s stress exposure is a balance of environmental exposure versus offloading capability using coping mechanisms. People usually minimise their exposure to stressful environments by moving to less stressful environments when possible. If this is not possible, then stress accumulation is dictated by that environment. If this balance is even slightly net negative, overall stress levels will continue to rise. This is why small grievances such as food preparation, division of chores and personal hygiene balloon into major sources of conflict and distress.16 This is also a major contributing factor to the escalation of substance abuse, relationship breakdown and domestic abuse.
Risk factors
Quarantine-related distress has been associated with factors such as low socioeconomic background,4 lower level of formal education and previous history of psychiatric illness.1 Being a healthcare worker in an epidemic situation is also a specific vulnerability.7,17 Quarantine results in a significantly higher incidence of both depression and PTSD symptoms in healthcare workers even three years following the event.6,18
How personality influences coping under confined conditions is researched using the ‘big five’ or OCEAN model of personality (Figure 2). This model classifies individuals according to the five dimensions of openness, conscientiousness, extraversion, agreeableness and neuroticism. People who struggle most with confinement are those with high scores of neuroticism (low resilience to stress) and low scores in conscientiousness and agreeableness (which broadly correlate with interpersonal living and conflict resolution skills).19 Highly extroverted or introverted individuals are also likely to struggle, the former because of insufficient external social contact, and the latter because of overwhelming contact within the home. In any group living situation, the specific mix of personality traits results in a unique combination that may predispose to conflict or be protective.20
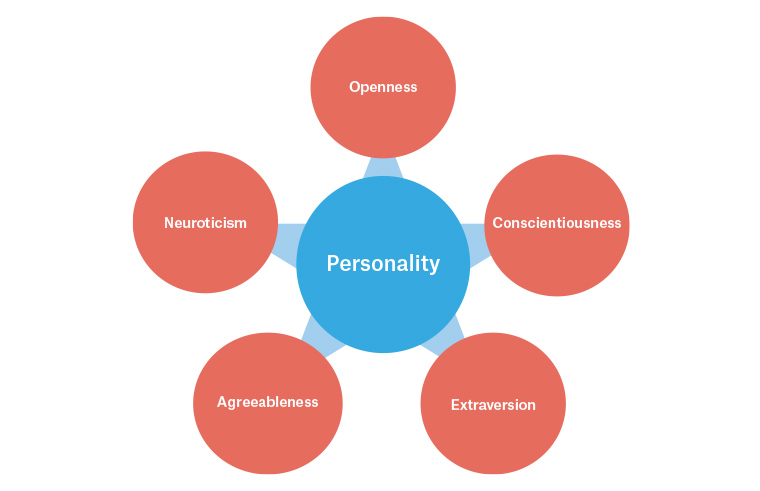
Figure 2. OCEAN model of personality51
The most important stressor is the duration of the confinement as this magnifies the cumulative load of most others. The second is inadequate information from health authorities. This is a major cause of confusion, stress and poor quarantine adherence. Individuals often report a poor understanding of why quarantine is even necessary, with some believing that quarantine is indicated for their own protection rather than that of others.21 Other sequelae include increased fear, inappropriate measures such as stockpiling and either poor quarantine adherence or excessive quarantine behaviours that may further escalate isolation distress. Lastly, inadequate access to essential supplies (eg prescription medication, food or hygiene products) increases the perceived stressfulness and therefore mental health risks of the experience.
Notable differences exist between types of confinement. Mandatory hotel quarantine involves a poorly adapted space due to both a hotel room’s small living area and the lack of stress-reducing environmental features intrinsic to a home. The short duration of hotel quarantine (usually two weeks) may have fewer adverse effects than confinement in the home as it allows psychological preparation for both the environment and an end date of the confinement. In contrast, confinement in the home usually involves more liveable space and less environmental stress. However, confinement with an uncertain end date is particularly stressful as it limits psychological preparation for the experience. When compared with non–health related confinement, being infected with COVID-19 or awaiting the possibility of becoming ill is likely to be more stressful because of the fear of mortality or morbidity associated with a novel disease.
In the post-quarantine period, financial difficulty is associated with anger and anxiety several months after quarantine as well as a predisposition to PTSD and depression.22 Stigma is another important societal consideration. Healthcare workers and recovered individuals have previously been particularly stigmatised by members of the general public and even in personal social circles because of a fear that their exposure risk may result in spread of infection.1,5
Adapting to the stress of isolation and quarantine
Difficulties experienced during confinement can be divided into intrapersonal and interpersonal. Both are closely associated with the personality traits (previously discussed) and coping strategies of the individual (Table 1).
| Table 1. Examples of coping strategies in the context of long-duration isolation23,24 |
| Poorly adapted coping strategies |
Well-adapted coping strategies |
| Denial: Refusal or inability to accept an aspect of reality that is troubling |
Suppression: Conscious repression of distressing thoughts or feelings |
| Reaction formation: Reacting to uncomfortable feelings or thoughts with an exaggerated opposing response (eg fighting boredom by achieving a manic level of constant busyness) |
Sublimation: Using negative thoughts or feelings for a constructive purpose (eg distress fuelling creative art construction, a negative experience informing behavioural change) |
| Displacement: Unacceptable negative feelings are redirected towards a safer target (eg conflict with a household member taken out on a social support worker) |
Altruism: Transforming uncomfortable feelings by helping others who have similar experiences |
| Acting out: Impulsive expression of thought or emotion without reflection or consideration for the outcome |
Distraction: Consciously putting off thoughts or feelings by focusing attention on something less threatening/more positive |
Coping strategies can be adaptive or detrimental, and having fewer adaptive strategies results in higher risk.23,24 Hobbies, leisure activities and occupational work are goal-directed activities that distract from the environment and give meaning by contributing to an organisational purpose or driving aspects of personal development. Non–goal directed activities (eg watching television shows, watching movies, reading books) are helpful distraction strategies but typically do not give as much meaning to the experience. Any individual activity becomes onerous if overused; hence, having several strategies, with a balance of goal-directed and non–goal directed strategies, is protective. Boredom is a stress-producing cognitive hypostimulation state with neurophysiological implications. Studies have shown changes in physiological markers that have been correlated with isolation-induced stress.25
Routine is often lost in the less structured lifestyle of confinement, which can have significant sequelae. Malleable work or school hours can lead to increasingly late nights and sleep shifting, which, if left unchecked, can result in circadian rhythm disturbance and loss of daily routine.
Interpersonal conflict is typically the greatest source of stress in confined groups.26 In the COVID-19 social isolation context, the household is required to adapt to a very different set of circumstances in a familiar but static environment. This is further intensified by the entire family unit being at home and attempting to carry out home schooling and working from home. Bringing these external responsibilities into the home may combine with the usual personal and cohabitation routines – such as cleaning rosters, cooking duties and interactional styles – to cause a maladaptive family system. For example, if the stay-at-home partner usually managed all the kitchen chores, now that the entire family is home it may reduce group conflict if those activities are shared until confinement ends. In contrast, those living alone are particularly vulnerable to the stress of social isolation and loss of external supports; at-risk populations include older persons and those with pre-existing mental health disorders. This is further exacerbated by restriction of access to social support services during a pandemic situation.
Conflict can occur in strange ways in these situations. Within a small group of people living together under stressful conditions, a single person can sometimes be ‘scapegoated’ and blamed as the cause of conflict by the rest of the group, putting that person’s mental health at further risk.27 Another well-studied phenomenon is for groups to smother internal conflict with the unintended result of displacing their frustrations and negative emotions onto an external agency. In the COVID-19 setting, this may result in unexpected hostility toward support services such as healthcare or other outreach workers.27,28
Assessment of confinement distress
Assessment of quarantine distress entails an evaluation of psychological wellbeing, psychopathology and risk factors, which situationally may benefit from the development of telehealth-specific skillsets.29 After addressing any potential acute psychiatric illness, questioning may be directed towards identifying confinement-related stressors.
The first step is to assess the individual’s personality, adaptive versus maladaptive coping strategies, daily routines, interpersonal skills and wider social supports. It is particularly important to consider daily routines and attention to diet, exercise and quality of sleep. All of these have an integral relationship with mental health, and poor attention to any will increase the vulnerability of the individual to poor coping. Questioning should also attempt to identify sabotaging behaviours such as poorly adapted coping strategies (eg alcohol or substances), which result in short-term relief and longer-term exacerbation. Interactional styles that exacerbate conflict may include avoidance of addressing interpersonal challenges, vengeful responses or an inability to compromise. Understanding the home environment is essential to understand the context of the current distress or conflict. This includes details such as who lives in the home, what they do with their time and what those relationships are like. An extroverted bartender who is suddenly unemployed is likely to come into conflict with an introverted computer programmer given their contrasting needs.
The most important aspects of the physical home include the size and type of property (house/apartment etc) and how much access to privacy/personal space the occupants have. It is important to check if the individual has somewhere to conduct a private telehealth consultation. Internet is an essential service as a method of communication with external social supports and access to occupational and leisure activities. It can therefore be beneficial to ask whether the patient has unrestricted access to a device or if it is shared. It is also important to inquire about about sufficient bandwidth (ie internet speed when multiple users are online at the same time) and data (ie overall monthly download limit).
Management of confinement distress
Much of the distress caused by confinement can be mitigated through simple interventions, many of which are available online.30–32 A clinician may identify stressors and suggest new, more adapted coping strategies (Box 1). This may be as simple as brainstorming potential hobbies and other goal-directed activities.33 The clinician can consider delivering education on the impact of substances and the benefits of sleep hygiene and routine.
| Box 1. Six key strategies to recommend to patients |
- Offer simple psychoeducation on the balance between build-up of stressors and the ability to offload them using coping strategies.
- Encourage patients to brainstorm multiple coping strategies to try. These should
include both individual (eg learning to draw) and group strategies for the entire household (eg board games).
- Advise that strategies should be a combination of goal-directed (eg learning a
skill/creating) and non–goal directed (eg absorbing media).
- Reinforce how important routine, diet, exercise and sleep hygiene are to maintaining mental health.
- Promote social engagement via phone, video chat or socially distanced meeting wherever possible to improve connectedness.
- Recommend simple changes to the home through light, furniture layout and decorations to bring novelty and visual interest to the environment.
|
Encouraging the engagement of wider social supports via electronic media and improvement of interpersonal skills is a way to quickly improve connectedness. There are numerous online communities that can provide quick methods of building social interaction opportunities.33 However, it is important that patients are warned regarding the saturation of social media with misinformation, which needs to be filtered out or avoided.
Finally, since the environment is a major stressor, reduction of hypostimulation has profound psychological results. Simple interventions include spring-cleaning the home, letting in more sunlight and innovatively using visual arts and interior furniture. The importance of natural environments should be emphasised as they are a source of reduction in physiological stress markers as well as a source of psychological benefits.34–38 Simple actions such as introducing natural imagery into living spaces enhance the visual novelty derived from physical space and its cognitive effects, which have been shown to synergise with behavioural interventions.39–42 For those working from home, recommendations include adapting their physical working space as best they can, maintaining a routine and placing more emphasis on supportive professional relationships to minimise isolation.
When to refer
Early intervention may de-escalate stress accumulation and thereby avoid the need for specialised supports. Early referral for psychological support is recommended for patients demonstrating a limited ability to engage with distress management strategies. A history of acute mental health deteriorations, limited social supports or significant vulnerability to escalating interpersonal conflicts are also important factors. A comprehensive risk assessment should always be part of the initial assessment, with the goal of looking at risks to self, others, finances and reputation, particularly online. Given the increased risk of domestic violence noted in COVID-19-related confinement, clinicians should ask about these risks and provide short-term support while linking with appropriate services if required.43–49
Psychiatric referral is recommended when psychiatric disorders or increased risk of suicide or deliberate self-harm are present. Likewise, early signs of significant chronic emotional impact suggestive of a high risk of developing PTSD may be appropriate indications for specialist consultation.
While isolation is psychologically challenging and potentially dangerous, it can paradoxically result in an improvement in overall mental health. Successfully navigating stressful experiences can bolster the individual’s self-agency and provide confirmation of the strength of relationships. Under lockdown, benefits have arisen as many cities have seen an increase in the use of parks and public spaces, and people find satisfaction in spring-cleaning their homes, engaging in long-delayed activities or simply spending time together. Assisting the individual to find meaning in the experience, together with simple interventions, can encourage such positive outcomes.
Key points
- Extended periods of confinement can be associated with psychological symptoms as well as depressive, anxiety and post-traumatic stress disorders.
- Factors predisposing individuals towards these outcomes include a past history of mental illness, belonging to a vulnerable group, and a lack of quality information about risks of infection, why these measures are necessary and clear guidelines to follow.
- Resilience to confinement is associated with having a range of adaptive coping strategies, goal-directed and non–goal directed activities, communication skills and interpersonal aptitude.
- Acute confinement-induced distress often responds to basic interventions such as psychoeducation, coping strategies and conflict management skills. If the clinician is unable to engage in these discussions at an early stage, referral for ongoing psychological support or management of psychiatric disorders with specialist services is suggested.