Case
A Caucasian woman aged 68 years initially presented with a three-week history of a new-onset headache, postnasal drip and mild sore throat. The headache was dull in nature, persistent and located over her right forehead. The patient reported that it was worse when she was lying down at night. Examination at that time revealed mild tenderness over her frontal and maxillary sinuses, and the neurological examination was normal. A clinical diagnosis of acute sinusitis was made, and the patient was treated with oral cephalexin.
On day four of taking the antibiotic, the patient developed right upper lid drooping, eye pain and double vision. She presented to an optometrist on that day, who confirmed the findings and referred her back to her general practitioner.
The patient elected not to return for three more days. At that stage, she had also developed fatigue but no limb weakness, fever, jaw or scalp pain. The key examination findings were: blood pressure 178/104 mmHg, heart rate 77 beats per minute, normal temperature, right eye deviated down and out, right partial ptosis, both pupils equal and reactive to light (Figure 1), with thickened and mildly tender right temporal vessels (Figure 2).
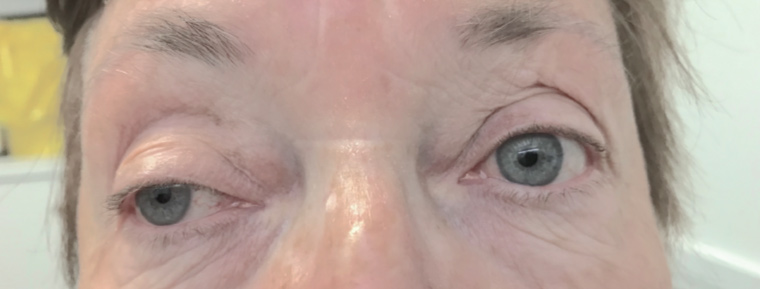
Figure 1. Right partial third cranial nerve palsy
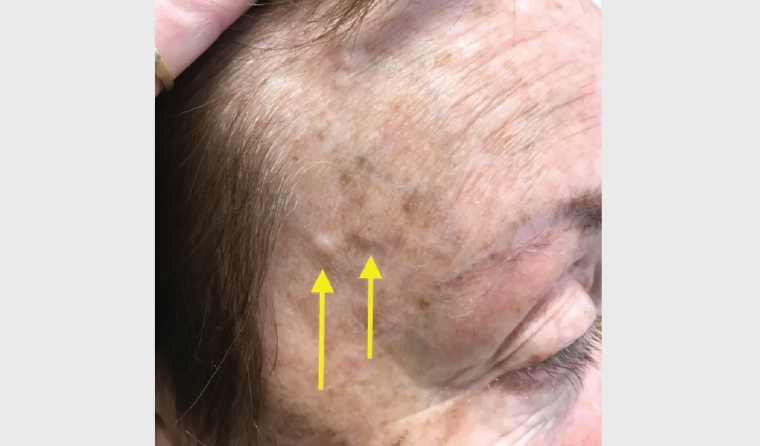
Figure 2. Thickened right temporal vessels (arrows)
Question 1
What is the neurological pathology of the patient’s eye signs (Figure 1)?
Question 2
What are the possible causes of this condition?
Question 3
What investigations would be appropriate for the patient at this stage?
Answer 1
The patient had right partial pupil-sparing third cranial (oculomotor) nerve palsy. The classic features of complete third nerve palsy are ‘down and out’ eye deviation, ptosis, mydriasis, failure of accommodation and absent light reflex with intact consensual constriction of the contralateral eye.1
Answer 2
The common causes of acquired third nerve palsy are microvascular, trauma, compressive effect from neoplasm and aneurysm, and post-neurosurgery; less common causes are thrombosis, inflammation and infection.2,3
Answer 3
At this time, it would be appropriate to perform a full blood examination; testing for erythrocyte sedimentation rate (ESR), serum C-reactive protein and acetylcholine receptor antibody; head computerised tomography (CT) and a temporal artery biopsy.
Case continued
The patient’s ESR was 63 mm/hour (reference range <20 mm/hour) and the serum C-reactive protein was 62 mg/L (reference range 0–10 mg/L), while the acetylcholine receptor antibody results and head CT scan were normal.
On the basis of the clinical presentation and laboratory results, a diagnosis of giant cell arteritis (GCA) with right partial third cranial nerve palsy was made. The patient was prescribed a high dose of prednisolone and amlodipine for raised blood pressure. The patient opted not to undergo temporal artery biopsy as her symptoms responded quickly to the prednisolone – her right eye pain and diplopia resolved after three days of treatment. The partial ptosis and thickened right temporal vessels almost completely recovered after three weeks of treatment (Figures 3 and 4). The prednisolone was tapered to half of the initial dose after one week, and it was lowered further two months after the initiation of the corticosteroid.
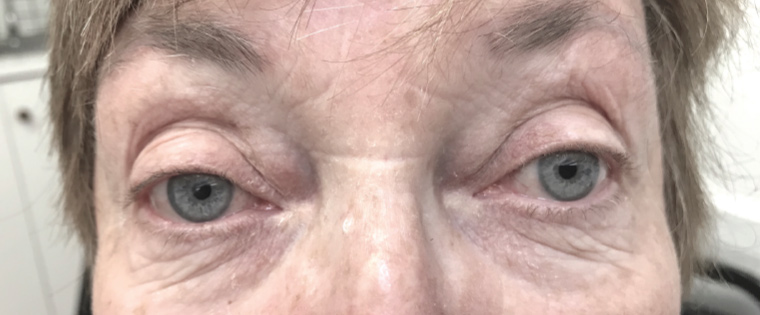
Figure 3. Recovery of third nerve palsy after three weeks of treatment
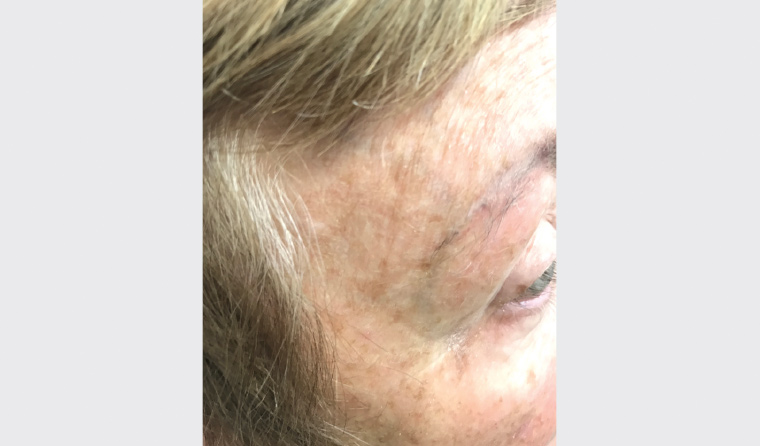
Figure 4. Recovery of right temporal vessels after three weeks of treatment
After four weeks of treatment, the patient was referred to a visiting consultant physician and was commenced on weekly risedronate, daily vitamin D and calcium supplementation to prevent corticosteroid-induced osteoporosis.4
The patient was referred to a rheumatologist four months later as she had intermittent loose bowel movements with prednisolone. Methotrexate was prescribed, and magnetic resonance angiography of the head was organised by the rheumatologist; this showed a normal study. However, the patient still had loose bowel movements, and the methotrexate was stopped subsequently. The patient was prescribed low-dose corticosteroid treatment for a total of 18–24 months. Her ESR and serum C-reactive protein were within normal ranges without headache, right eye pain or diplopia throughout the treatment.
Question 4
What are the common presentations of GCA, and why is early diagnosis important?
Question 5
What is the role of temporal artery biopsy in the management of GCA?
Answer 4
GCA, also known as temporal arteritis or cranial arteritis, is a vasculitis of the large and medium arteries of the head and neck.5 It is characterised by critical ischaemia and is one of the common causes of acute visual loss. GCA should be regarded as a medical emergency; early recognition, referral and treatment are extremely important.6
The most common symptoms of GCA are headache; neck, shoulder and pelvic pain; fatigue and malaise; jaw claudication and fever. Less common symptoms are limb claudication, transient ischaemic attacks or stroke, tongue or throat claudication, diplopia or ptosis, tongue numbness and myelopathic symptoms.7 The reported incidence of ptosis in patients with GCA is rare at approximately 1–2%.2,7
Answer 5
With 100% specificity, temporal artery biopsy is the gold standard of diagnosis of temporal arteritis.8 However, in accordance with the patient’s wishes, it was not performed in this case, and the diagnosis was made mainly on the basis of the clinical and laboratory findings and application of the American College of Rheumatology (ACR) 1990 criteria.9 A GCA diagnosis requires the presence of at least three ACR criteria, which include:
- patient age ≥50 years
- new onset of localised headache
- temporal artery tenderness or reduced pulse
- ESR ≥50 mm/hour
- abnormal temporal artery biopsy.
The fulfillment of three or more ACR criteria yields a sensitivity of 93.5% and specificity of 91.2% for the diagnosis of GCA.9 The patient in this case fulfilled four out of five criteria, and her symptoms responded promptly to a treatment regimen that aligned with the ACR guidelines.
Despite the fact that temporal artery biopsy is a standard procedure for patients with suspected GCA, it has a poor sensitivity, with a false-negative rate reported as high as 44%.10 It is affected by inadequate specimen length, skip lesion of the temporal artery, expertise of the surgeon, interpretation of histology and effects of medication.11 Consequently, temporal artery biopsy is particularly useful for patients who fulfill two ACR criteria, for whom the biopsy result may affect management.8
Key points
- GCA may present with acute features of third nerve palsy.
- It is important to consider GCA as one of the differential diagnoses in patients with acute painful unilateral third nerve palsy.
- Initial treatment with a high-dose corticosteroid rapidly improves third nerve palsy of GCA and avoids the complication of acute blindness.