Primary care systems with interprofessional collaboration in the diagnosis and management of familial hypercholesterolaemia
I read with interest the study by Bulsara and colleagues reporting the awareness of familial hypercholesterolaemia (FH) among general practitioners (GPs; AJGP September 2021).1 FH is the most frequent genetic disorder with high low-density lipoprotein concentrations, and earlier treatment prevents coronary disease; GPs’ role in the diagnosis and management of FH is thus important. In primary care systems, interprofessional collaboration is also effective to manage FH patients; for instance, various medical staff, including community nurses and pharmacists, as well as healthcare companies, have roles in the FH practice. Non-medical partners can participate in the collaboration.2 Patient organisations/associations for patients and families help enlighten the general public about FH. Laypeople can be enticed to participate in initiatives, including genetic screening events and self-check-ups, once they have a proper understanding of FH.2 Australia is ahead of the curve with regard to such interprofessional collaboration with GPs, and the efforts to develop the systems are worthy of special mention.
Given the difference in primary care systems between countries, what is the system of diagnosis and management of FH in Japan, where people have free access to any clinic? Depending on their physical signs, patients with FH are known to visit non-GPs, including dermatologists/plastic surgeons (for skin xanthomas or xanthelasma palpebrarum) and ophthalmologists (for arcus corneae lipoides or xanthelasma palpebrarum).3 When paediatricians and obstetricians see physical signs and blood tests suspicious of FH, they may notice children/young patients with FH. As these non-GPs are the first-contact physicians for the identification of FH, greater education concerning FH for not only GPs but also non-GPs is needed. Meanwhile, a childhood genetic screening program was recently started in a prefecture of Japan,4 and the involvement of pharmacists in community-based healthcare networks has been recently promoted.5 The momentum of interprofessional collaboration to diagnose and manage patients with FH may thus be increasing by slim degrees in Japan. Accumulating information, such as that provided by the Bulsara et al study,1 would be useful when discussing the infrastructure in primary care systems – not only in Australia, but also in other countries such as Japan, where the development of systems for FH in the near future is anticipated (Figure 1).
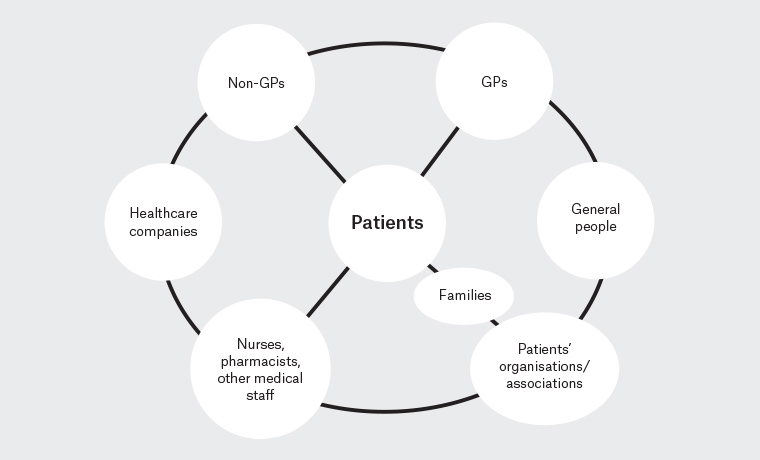
Figure 1. An anticipated network system with interprofessional collaboration for familial hypercholesterolaemia in Japan
GPs, general practitioners
Kazuhiko Kotani MD, PhD
Division of Community
and Family Medicine,
Jichi Medical University,
Shimotsuke, Japan
References
- Bulsara C, Brett T, Radford J, et al. Awareness of familial hypercholesterolaemia in Australian primary care: A qualitative descriptive study. Aust J Gen Pract 2021;50(9):634–40. doi: 10.31128/AJGP-04-21-5952.
- Brett T, Watts GF, Arnold-Reed DE, et al. Challenges in the care of familial hypercholesterolemia: A community care perspective. Expert Rev Cardiovasc Ther 2015;13(10):1091–100. doi: 10.1586/14779072.2015.1082907.
- Altschmiedová T, Vaclová M, Vráblík M. Diagnosis of familial hypercholesterolaemia on first sight? The role of the ophthalmologist in identifying patients with familial hypercholesterolaemia. Cesk Slov Oftalmol 2019;74(4):127–31. doi: 10.31348/2018/1/1-4-2018.
- Matsunaga K, Mizobuchi A, Fu HY, et al. Universal screening for familial hypercholesterolemia in children in Kagawa, Japan. J Atheroscler Thromb 2021. doi: 10.5551/jat.62780. Epub ahead of print.
- Sato N, Fujita K, Kushida K, Chen TF. Exploring the factors influencing the quality of ’Health Support Pharmacy’ services in Japan: Perspectives of community pharmacists. Res Social Adm Pharm 2020;16(12):1686–93. doi: 10.1016/j.sapharm.2020.02.012.
Reply
Thank you for your thoughtful comments on our recent article.1
Some of the biggest gaps in detecting and managing familial hypercholesterolaemia (FH) are among children and adolescents and in primary care, and this continues despite attempts to increase awareness among general practitioners (GPs), practice nurses, patients and families2,3 and the relatively easy access to general practice services in many countries.
The author correctly identifies ophthalmologists, dermatologists, paediatricians and obstetricians as non-GP specialists that are periodically confronted with a clinical presentation reflecting FH as the likely underlying pathology. You could also add the contributions of orthopaedic surgeons in identifying FH through their role in excising tendon xanthomata and that of chemical pathologists in flagging potential FH with grossly elevated hypercholesterolaemia. Likewise, pharmacists, community nurses as well as other healthcare providers may also have the opportunity to recognise previously undetected tell-tale signs of FH.
A basic understanding of the pathophysiology of FH among any alert healthcare provider can have enormous potential in facilitating the first tentative steps in alerting affected patients and their families of the need for further clinical assessment and potential FH diagnosis.
The author rightly encourages greater collaboration between GP and non-GP networks in the detection and management of FH. Close family relatives are also recognised as excellent advocates to optimise the treatment of affected family members. Similarly, reverse cascade screening to parents of newly diagnosed toddlers provides the opportunity for starting good health measures in childhood before the effects of their increased cholesterol burden become manifest in their coronary arteries but also to potentially save the life of one of their parents, who will also harbour the condition. 4
Increasing awareness and education about FH as well as implementing change in management practices can be challenging. Strategies to implement newer approaches to diagnosis and management need a broad-brush approach, and implementation scientists can have a major role in this regard. The recent taxonomy by Powell et al contains 73 strategies to assists with implementation.5
Your comments are welcome, timely and well placed.
Tom Brett MA, MD, FRACGP, MRCGP,
Professor and Director,
General Practice and Primary
Health Care Research,
School of Medicine, University of
Notre Dame, Fremantle, WA;
General Practitioner, Mosman Park Medical Centre, Mosman Park, WA
References
- Bulsara C, Brett T, Radford J, et al. Awareness of familial hypercholesterolaemia in Australian primary care: A qualitative descriptive study. Aust J Gen Pract 2021;50(9):634–40. doi: 10.31128/AJGP-04-21-5952.
- Brett T, Qureshi N, Gidding S, Watts GF. Screening for familial hypercholesterolaemia in primary care: Time for general practice to play its part. Atherosclerosis 2018;277:399–406. doi: 10.1016/j.atherosclerosis.2018.08.019.
- Brett T. Familial hypercholesterolaemia: Educational videos for general practitioners, practice nurses, patients and families. Fremantle, WA: University of Notre Dame, 2021. Available at https://vimeopro.com/notredamemedia/fh-awareness [Accessed 15 December 2021].
- Wald DS, Bestwick JP, Morris JK, Whyte K, Jenkins L, Wald NJ. Child-parent familial hypercholesterolemia screening in primary care. N Engl J Med 2016;375(17):1628–37. doi: 10.1056/NEJMoa1602777.
- Powell BJ, Waltz TJ, Chinman MJ, et al. A refined compilation of implementation strategies: Results from the Expert Recommendations for Implementing Change (ERIC) project. Implement Sci 2015;10:21. doi: 10.1186/s13012-015-0209-1.