Case
A man aged 29 years presented with a 15-year history of atopic dermatitis, which started on his feet and spread to his thighs, lower abdomen, back and buttocks (Figure 1). He reported severe and distressing pruritus that had a significant impact on his ability to work and sleep. He reported frustration as he had used multiple topical corticosteroid preparations, which would provide some initial relief then rapidly lose efficacy.
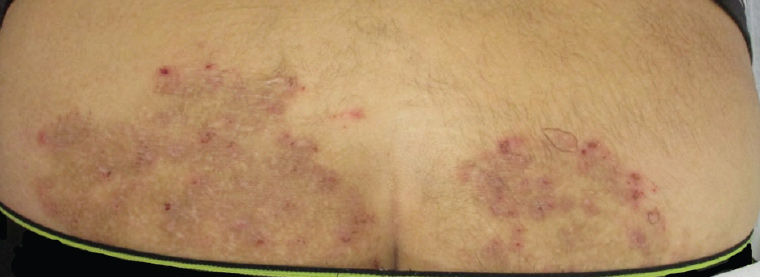
Figure 1. A representative area of involvement, with a large, hyperpigmented, excoriated and somewhat atrophic patch on the patient’s lower back and buttocks
He worked as a chef and described himself as otherwise well. His only regular medications were perindopril and agomelatine, both of which were initiated after the pruritus had commenced. He took no herbal or over-the-counter remedies. With the exception of childhood asthma that had resolved, he had no other features of atopy and did not have any family history of this or any other relevant medical concern. No other members of his household were affected, and he had no pets.
Question 1
What is the differential diagnosis?
Question 2
What investigations would you perform?
Answer 1
The differential diagnosis includes contact dermatitis, dermatophyte infection, incompletely treated psoriasis, dermatitis herpetiformis or mycosis fungoides. Medication reaction, atypical infection and systemic causes of pruritus such as uraemia, liver disease, haematological disease, malignancy and endocrine disorders are less likely given the presenting history.
Answer 2
Investigations may include skin scrapings to be sent for fungal microscopy, culture and sensitivity (MCS); skin biopsies to be sent for histopathology and basic blood tests including a full blood examination and chemistry panel to screen for underlying systemic causes and to assess for suitability of systemic treatments if required. Epicutaneous patch testing may also be conducted by a dermatologist if contact allergy is suspected.
It is important to examine the feet and toenails of patients with potential fungal superinfections, even if the patient denies involvement of these areas. Toenails often represent the reservoir for fungal infection, and if there is any suggestion of involvement, nail clippings or scrapings should also be sent for fungal MCS.
Case continued
Routine blood work, including a full blood examination and comprehensive chemistry panel, was requested, and results of these were within normal limits. Skin scrapings were collected, ensuring a good sample was collected from multiple edges of the involved areas, and were sent for fungal MCS. These showed no growth.
Following this, two 3 mm punch biopsies of the affected area were collected and sent for histopathology (Figure 2).
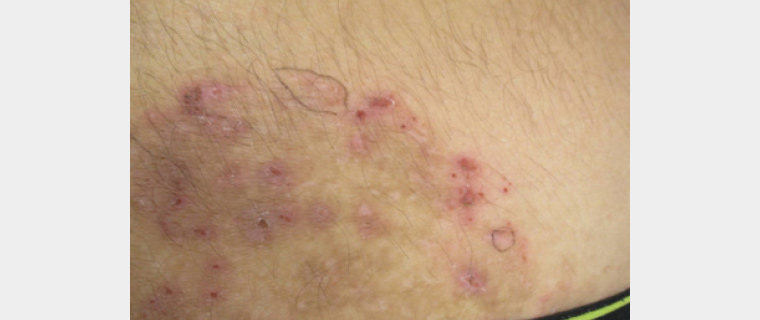
Figure 2. Close-up image of an affected area, showing the sites selected and marked for 3 mm punch biopsy
As extensive epicutaneous patch testing had been conducted for this patient previously and was negative for all allergens tested, it was not repeated.
The two 3 mm punch biopsies revealed compact orthokeratosis containing scattered fungal hyphae. The epidermis was moderately acantholytic, with mild spongiosis and a mild superficial perivascular infiltrate of lymphocytes and occasional eosinophils. This was consistent with a diagnosis of tinea incognita, with subsequent culture showing growth of
Trichophyton rubrum.
Question 3
What is tinea incognita?
Question 4
What are your options for management?
Answer 3
Superficial dermatophyte infections in humans are common and are often caused by fungi from the genera Trichophyton or Microsporum. Superficial dermatophyte infections present as pruritic, erythematous, scaling, sharply demarcated plaques with peripheral enlargement and often central clearing.1,2
Tinea incognita is the descriptive definition of a superficial dermatophyte infection that has had its usual appearance altered by the application of topical corticosteroid, with the relative immunosuppression caused by the corticosteroid’s application potentially leading to larger extension of the lesion than what might otherwise be expected.1,3
Answer 4
According to Therapeutic Guidelines,4 the use of oral antifungal therapies is appropriate for dermatophyte infections that are widespread or established; have not responded to topical antifungal therapies; recur soon after treatment; are on the scalp, palms or soles; are inflammatory, hyperkeratotic or vesicular; or, as in this case, have been inappropriately treated with corticosteroids.
Therapeutic Guidelines recommend the use of terbinafine 250 mg orally once per day for two weeks, fluconazole 150 mg orally once weekly for six weeks or griseofulvin 500 mg orally once per day for 8–12 weeks, initiated after careful consideration of potential medication interactions and relevant patient factors.
Case continued
The patient was commenced on a course of griseofulvin. He noted a significant improvement in his symptoms within two weeks of commencement, reporting no itch at all, improved sleep quality and improvement in longstanding anxiety. He did not report any adverse effects with the use of griseofulvin. He did not require the use of any topical treatments, though he did continue to use a bland emollient.
Conclusion
Chronic pruritus can have a significant impact on a patient’s quality of life, and atypical presentations or a lack of response to conventional therapies such as topical corticosteroids warrant investigation of potential differential diagnoses.
Key points
- Tinea incognita describes the atypical presentation of a superficial dermatophyte infection that has been misidentified and treated with topical corticosteroids.
- If there is suspicion that a presentation is caused by a dermatophyte but fungal scrapings yield negative results, a biopsy may be indicated.
- In some cases, superficial dermatophyte infections will require systemic therapy.