Case
A boy, aged 10 years, presented with a two-week history of pruritic lesions on the frontal region. His medical history included scalp psoriasis, which he controlled with topical application of clobetasol. The patient’s immunisation status was up to date and he had no known medication allergies.
Physical examination revealed the presence of monomorphic papules and pustules on an erythematous base (Figure 1). No open or closed comedones were identified. There were no other mucocutaneous lesions or associated systemic symptoms.
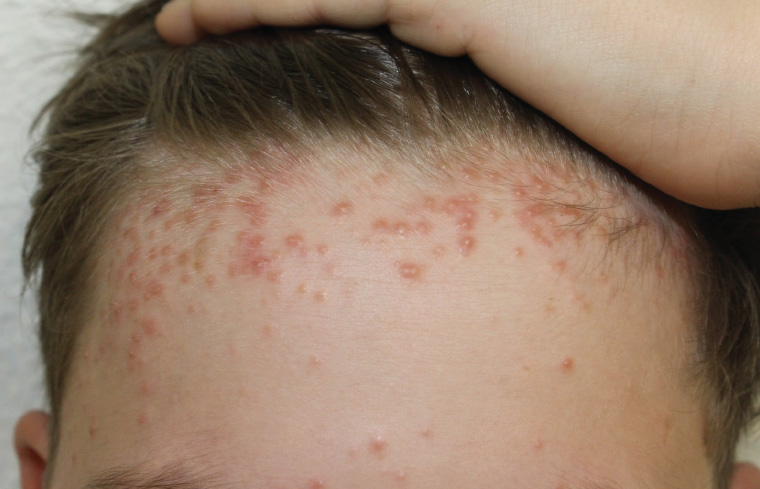
Figure 1. Monomorphic papules and pustules on an erythematous base located on the forehead and more densely clustered towards the scalp.
Question 1
What differential diagnoses should be taken into account?
Question 2
What features may help determine the diagnosis of steroid acne?
Question 3
What is the pathophysiology of this condition?
Question 4
What management is required for this condition?
Answer 1
Acne vulgaris is an important differential diagnosis to consider, which is characterised by the constant presence of comedones (blackheads and whiteheads). The heterogeneity of acne vulgaris lesions, which may include nodules, pseudocysts, postinflammatory erythema or scarring, can help distinguish it from other conditions.1,2
In contrast, rosacea commonly manifests on the central face with reddened areas that exhibit warmth or tenderness upon palpation, accompanied by the presence of papules, pustules and telangiectasias.2
Malassezia folliculitis is another possible diagnosis, presenting as a monomorphic eruption of small papulopustules, accompanied by perifollicular erythema, perilesional scaling and coiled hairs. Clinical history can be crucial for making the correct diagnosis in such cases.1,2
Acneiform eruptions caused by certain drugs, including antibiotics, isoniazid, naproxen or epidermal growth factor receptor inhibitors, are also worth considering. Suspecting this entity should prompt a careful review of the patient’s medical history for potential drug exposure.1,2
Both the patient’s history and the previous clinical findings are consistent with a diagnosis of steroid acne. This condition occurs secondarily to the use of topical or systemic glucocorticoids in predisposed individuals.
Answer 2
A history of prolonged steroid use is required for the diagnosis. The locations of the lesions may also be a clue, because they typically occur on areas where the corticosteroids have been applied or where there is a high concentration of sebaceous glands, such as the face, chest and upper back.1–3
As mentioned previously, steroid acne lesions are typically small, uniform and monomorphic, unlike traditional acne, which can have various sizes and morphologies. Another supporting factor would be the presence of pruritus reported by some of these patients. 1 A rapid onset is also characteristic, because steroid acne develops rapidly within a few days to weeks.1–3
Finally, steroid acne usually resolves after the discontinuation of corticosteroid therapy.1,3
Answer 3
Although the exact cause of steroid acne is not yet fully understood, several factors are thought to contribute to its development. Corticosteroids have the ability to stimulate the sebaceous glands in the skin, leading to an increase in sebum production. They may also promote the accumulation of dead skin cells within hair follicles, leading to hyperkeratosis. These changes, combined with local immunosuppression caused by the steroids, create an environment that is conducive to bacterial colonisation and subsequent inflammation.2,3
Answer 4
Treating steroid acne typically involves discontinuing or reducing the dose of topical steroids, as well as using various acne therapies alone or in combination.1,3
Topical retinoids, such as tretinoin and adapalene, can help unclog hair follicles and reduce inflammation. However, these treatments can increase dryness and irritation, which should be monitored closely, especially in patients with atopic dermatitis. Sun protection should also be recommended to prevent further damage.4
Benzoyl peroxide is a common acne treatment due to its antibacterial properties and mild keratolytic effect. However, it can also cause skin irritation, sun sensitivity and clothing bleaching. Patients should be advised to avoid contact with fabrics and wash their hands after each application.4
Topical or oral antibiotics may also be used, depending on the severity of the acne. However, it is not recommended to use antibiotics as the sole treatment due to the risk of bacterial resistance. Topical clindamycin and erythromycin are among the most commonly prescribed antibiotics. The anti-inflammatory and antimicrobial properties of systemic erythromycin make it an effective treatment option for reducing the severity of acne. Nonetheless, its use can have limitations and potential adverse effects, including gastrointestinal disturbances and altered drug metabolism. As such, it is important for patients to inform their healthcare providers of all medications, supplements and herbal products they are taking before starting erythromycin.4
Case continued
These findings, together with a thorough investigation, after which the parents admitted to having exceeded the recommended amount of topical corticosteroid, led to the diagnosis of steroid acne. The parents were informed of the importance of not overusing this foam or other topical corticosteroid treatments, discontinuing it for the time being and recommending the application of a benzoyl peroxide gel.
At the one-month review, resolution of the previous lesions was observed. Topical steroids were resumed as maintenance treatment for the patient’s psoriasis with one to two applications per week.
Key points
- Steroid acne may appear in areas of topical steroid application or on patients taking systemic steroid treatments.
- Steroid acne usually presents as monomorphic papulopustules in the absence of comedones, occasionally accompanied by pruritus.
- Treatment should include discontinuation of steroid medication until the lesions have resolved.