A red, scaly cutaneous eruption in an older patient (age >65 years) is a relatively common dermatological presentation to general practice. These patients often have higher levels of chronic disease, polypharmacy and frailty, and might have limited social support. Therefore, a comprehensive approach to assessment is required.
Aim
This article will discuss an approach to assessment of red scaly eruptions in an older patient (age >65 years), the relevant differential diagnoses and practical clinical tips for common causes. We define a red, scaly eruption as an acute to subacute onset rash, composed of erythematous and scaly plaques present on multiple body sites.
Assessment of red, scaly eruptions in an older patient
Red, scaly eruptions in the older patient have a wide differential diagnosis. Assessment requires a working knowledge of common causes and paying attention to clues in the clinical assessment.
Pathogenesis
Scale can accompany many inflammatory conditions and is due to the presence of excess keratin.1 Epidermal inflammation can be driven by underlying immunological dysregulation, atopy, infections/infestations, drug reaction or cutaneous lymphoma (Table 1).
| Table 1. Diagnosis of red, scaly cutaneous eruptions in the older patient |
| Diagnosis |
Morphology |
Distribution |
Clinical clues |
Diagnostic tests |
| Atopic dermatitis (eczema) |
- Erythema, scale, excoriations, lichenification, xerosis
- Ill-defined plaques, except in discoid eczema, where plaques are well-defined and coin shaped
- Honey-coloured crusts if secondarily infected
|
- Can be widespread over trunk, limbs, head/neck
|
- History of atopy (eg asthma, hay fever, eczema), including in family members
- Xerosis
- Itch can be significant and disturb sleep
- Can be secondarily infected
|
- Skin biopsy
- Histopathology (if diagnosis unclear)
- Bacterial MCS if secondarily infected
|
| Psoriasis |
- Well-defined, scaly, salmon-pink plaques
- Non-scaly if involving the flexures
|
- Favours scalp, elbows, knees, umbilicus, natal cleft
- Might have palmoplantar or nail involvement
- Can be widespread
|
- Mostly asymptomatic but can be itchy
- Personal or family history of psoriasis
- Might be associated with seborrhoeic dermatitis (sebopsoriasis)
- Joint involvement: arthralgias, synovitis
Associated metabolic syndrome |
- Skin biopsy
- Histopathology (if diagnosis unclear)
- Blood pressure, liver function tests, fasting lipids, BMI and waist circumference
|
| Seborrhoeic dermatitis |
- Ill-defined erythema, greasy scale
|
- Favours seborrhoeic areas: scalp, forehead, eyebrows, nasolabial fold, conchal bowl, post-auricular
- Chest and back might be involved
|
- History of dandruff or flaking scalp
- Can be itchy if inflamed, otherwise relatively asymptomatic
- Oily skin/scalp
- Not washing hair or cleansing skin regularly
|
|
| Tinea |
- Classically annular eruption with a leading edge, central clearing and peripheral scale
- Can often produce non-specific rashes (especially if pretreated with topical steroids)
|
- Favours feet, groin and trunk
- Can also affect nails, hair or be widespread
|
- Associated onychomycosis in one or more toenails
- Asymmetrical
- Can be itchy or non-itchy
- ‘Two feet, one hand’: tinea pedis on feet with unilateral tinea manuum
- Might have associated secondary eczema (id reaction)
|
- Skin scrapings for fungal microscopy and culture
- Skin biopsy: histopathology (if diagnosis unclear)
|
| Scabies |
- Erythema, scale, excoriations
- Erythematous nodules on genitals
- Serpiginous thread-like tracks (burrows)
- Palmoplantar hyperkeratosis, significant crusting or scale (Norwegian scabies)
|
- Favours hands, wrists, feet, ankles, genitals
- Can be widespread
|
- Associated risk factors: residential facility, hospitalisation, homelessness, crowded or unhygienic living conditions, overseas travel
- Symptom onset might be delayed up to four to six weeks from time of exposure
- Itchy close contacts
|
- Clinical diagnosis
- Dermoscopy (delta sign)
- Skin scrapings for microscopy (taken from burrow)
|
| Drug eruption (generalised) |
- Various morphologies: eczematous, psoriasiform, lichenoid
|
- Widespread rather than localised
|
- Preceding culprit medication(s) up to three to six months prior to onset of eruption, although might occur more quickly
- No prior history of skin conditions
- Cutaneous eruption might persist up to three months after cessation of culprit drug
|
|
| Non-bullous pemphigoid |
- Eczematous or urticated plaques
- Might be followed by a bullous phase: tense blisters, typically arising within the rash
|
- Can be widespread
- Rarely involves mucous membranes, head and neck
|
- Non-bullous phase can persist for months to years
- Might have temporal relationship with culprit drug if drug associated
|
- Skin biopsy
- Histopathology (taken from the edge of a blister if present)
- DIF (taken from non-inflamed adjacent skin)
- Further blood testing based on specialist assessment
|
| Subacute cutaneous lupus |
- Erythema, scale, annular plaques
|
- Photodistributed sites: V of chest, upper back, outer arms
- Face is less commonly involved
|
- Might have associated systemic symptoms (eg synovitis, chest pain, shortness of breath)
|
- Skin biopsy
- Blood tests: ANA, ENA, dsDNA
- Urine microscopy: proteinuria, dysmorphic red blood cells, red cell casts
|
| Mycosis fungoides |
- Faint erythema, fine scale
|
- Bathing trunk distribution: buttocks, thighs, lower back
- Favours photoprotected sites
|
- Generally asymptomatic, occasionally itchy
- Often misdiagnosed and treated as eczema or psoriasis, but is often recalcitrant to treatment
- Might require multiple biopsies over time before diagnosis is made
|
- Skin biopsy
- Referral to specialist centre for special tests if suspected or confirmed
|
| ANA, antinuclear antibodies; BMI, body mass index; DIF, direct immunofluorescence; dsDNA, double-stranded DNA; ENA, extractable nuclear antigen antibodies; MCS, microscopy, culture, sensitivity. |
Differential diagnosis
Red, scaly eruptions can be due to an underlying dermatological condition or drug reaction (Table 1). The distribution and morphology of the eruption can provide clues as to the underlying diagnosis.
Approach to a red, scaly cutaneous eruption in an older patient
Assessment of older patients can be complex. A detailed history from both the patient and carers/family might be required to ascertain the timeline and symptomology.
History
The history would be best focused on the following:
- Timeline of onset: Sudden or gradual onset?
- Distribution: Affected areas? Pattern of spread?
- Pruritus: Itchy or non-itchy? Does itch disrupt sleep?
- Blistering: Any fluid-filled blisters?
- Medication history: Timeline of medication changes relative to onset of rash?
- Previous skin treatments: Moisturisers or over-the-counter treatments?
- Environmental factors exacerbating xerosis: Electric blankets, heaters or very hot showers?
- Itchy contacts: Contacts experiencing a rash or itch?
- Rheumatological symptoms: Joint aches, photosensitivity, shortness of breath or chest pain?
A review of the medical and family history for evidence of prior atopy (eg eczema, asthma and hay fever), psoriasis or connective tissue disease is helpful. A travel history can be taken if relevant.
Examination
A full skin examination is required for an accurate assessment. In patients with physical disability, a carer or family can be requested to assist.
A thorough skin examination would provide further clues to the diagnosis (Table 1):
- Distribution of the rash: Involvement of flexures or extensor surfaces? Favouring photo-exposed areas? Involvement of genitals or web spaces of the hands/feet? Involvement of hair-bearing areas (eg scalp, eyebrows, chest)?
- Morphology: Well-defined or ill-defined? Presence of blisters? Annular appearance?
- Complications: Evidence of impetiginisation (ie honey-coloured crust or erosions)? Excoriations or lichenification?
- Assessment of uninvolved skin: Evidence of xerosis or postinflammatory hyper-/hypopigmentation?
- Systemic examination: Assessment for hepatosplenomegaly and lymphadenopathy for rare cases of lymphoma. Rheumatological examination if cutaneous lupus is suspected.
Common causes of red, scaly eruptions in the older patient
Once clinical assessment has been completed, a working diagnosis can be formulated. In this section, common causes of red, scaly eruptions are discussed along with practical clinical tips.
Drug eruption
Polypharmacy is an increasingly significant cause of adverse drug events, which frequently include skin rashes.2 Cutaneous reactions can manifest in various forms, including a widespread red, scaly rash.
Drug eruptions can be challenging to diagnose and require a high index of suspicion. A timeline of drug initiation or dose modification is essential to determine whether a drug reaction has occurred, although there can be a delay of months to years between initiation and presentation.3 The most common implicated drugs prescribed in general practice are cardiovascular drugs, which are ubiquitously prescribed in the older patient (Box 1).
| Box 1. Commonly prescribed medications associated with a drug rash3,4 |
Calcium channel blockers (eg amlodipine)
Angiotensin-converting enzyme inhibitors
Angiotensin receptor blockers
Diuretics
Statins
Hydrochlorothiazide
Methyldopa |
A skin biopsy sent for histopathology can be helpful in confirming the suspicion of a drug eruption. The most common histopathological pattern elicited by systemic drugs is the perivascular pattern.5 A mixed reaction pattern with or without eosinophils might also be seen.5
The gold standard for the diagnosis and management of a drug eruption is resolution of the rash after cessation of the culprit medication, which might take several months.
Tinea
The estimated prevalence of onychomycosis in adults aged >70 years is ≥50%.6 Onychomycosis acts as a reservoir for dermatophytes, leading to involvement of other body sites, such as tinea cruris, corporis and manuum. Tinea can be a challenging diagnosis if the rash is treatment modified by prior topical steroid use. This can mask the annular and scaly appearance. Initial improvement with subsequent worsening with ongoing treatment with a topical steroid should raise suspicion of a dermatophyte infection.7
Treatment is with either topical or oral antifungals. In the older patient, topical therapy might be challenging to apply if tinea is widespread and there are limitations in mobility or carer availability (Figure 1). If onychomycosis is diagnosed alongside cutaneous infection, a long course of oral antifungals (eg terbinafine 250 mg daily for 12 weeks) might be indicated to clear the source and prevent recurrence. However, oral therapy needs to be used with caution in the older patient due to potentially significant drug interactions and risk of hepatotoxicity. In these situations, measurement of liver function tests at baseline and at two to four weeks is advisable.8
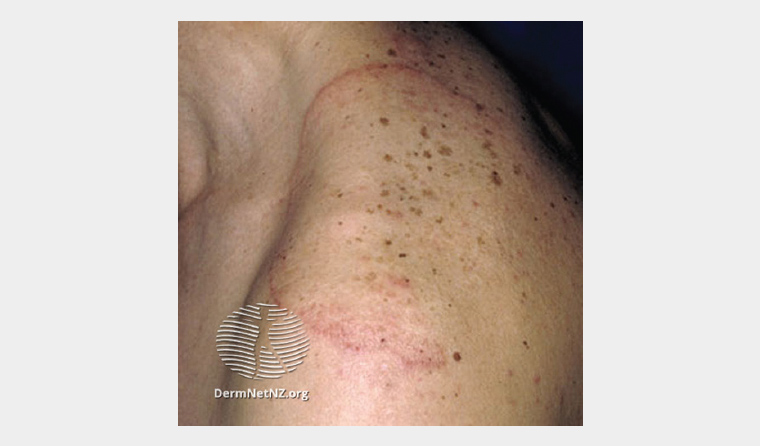
Figure 1. Tinea corporis: erythematous leading edge with central clearing.
In cases with a large area of involvement, oral antifungals are indicated, especially if onychomycosis is also present.
Reproduced from www.dermnetnz.org, with permission by ©DermNet and ©Professor Raimo Suhonen, 2023.
Scabies
Scabies is a skin infestation that affects vulnerable people in crowded conditions, including residents in aged care facilities.9 Scabies can be suspected when there is an itchy eruption favouring the ankles, genitals and web spaces of the hands and feet (Table 1). Dermoscopy can reveal a whitish curved or wavy line with a small dark brown triangular structure at the end (ie Delta sign).10,11
Scabies can be treated with either topical permethrin 5% cream or oral ivermectin 200 microgram/kg orally, with treatment repeated in seven days with either option.12 In the older patient, the oral dosing of ivermectin might improve adherence over topical treatment, especially when there are limitations in carer availability or mobility.
In the aged care setting, special consideration needs to be given to concurrent disinfestation of fomites (eg underwear, clothing, bed linen, personal effects), isolation of the case until 24 hours after treatment commencement and the identification of contacts who might have had close contact with the case.
Atopic dermatitis (eczema)
Although eczema is thought of primarily as a condition that affects adults and children, it also occurs in older patients. Due to the physiological effects of ageing on the skin, such as decreased sebaceous and sweat gland activity, cutaneous xerosis is present in >80% of older people.4 This is a risk factor for the development of eczema.
Management for eczema in the older person can be challenging. The general principles of generous emollients, topical steroids for inflamed areas and trigger avoidance can be difficult to implement for older people. These patients might be affected by physical limitations that constrain their capacity for self-application of topical treatments. Topical treatments can be costly and time-consuming for carers to apply.
To encourage adherence, the regime might need to be modified to make it simpler and more practical to use. Most topical steroids can be applied once daily, preferably in the evening or at night.13 In addition, tubes of a potent topical steroid can be expressed into a tub of moisturising emollient and then mixed with a spatula. This combined cream can then be applied to affected areas of the skin providing both moisturising and anti-inflammatory effects.
In cases where suspected atopic dermatitis is not responding to treatment, work-up for alternative diagnoses and/or escalation of treatment (eg systemic therapy) is advisable, possibly in conjunction with a dermatologist.
Psoriasis
Psoriasis onset follows a bimodal age pattern with the first peak at around age 30–39 years and the second peak at age 60–69 years.14 Clues to the diagnosis include well-defined red, silvery, scaled plaques, a family history of psoriasis and the pattern of distribution (Table 1).
Diagnosis can be made on clinical grounds, although a skin biopsy is helpful if there is doubt. Treatment is with topical therapies (eg steroids, calcipotriol, liquor picis carbonatum + salicylic acid), phototherapy or systemic agents depending on the site/extent of disease and impact on quality of life.15 In addition, the patient would ideally be assessed for joint symptoms, as well as their cardiometabolic profile.15
Bullous pemphigoid
Bullous pemphigoid onset is typically after the age of 70 years.16 Non-bullous pemphigoid is a clinical variant that can present as eczematous and urticated plaques (Figure 2).10 These plaques can be widespread and usually spare mucous membranes, the head and neck.
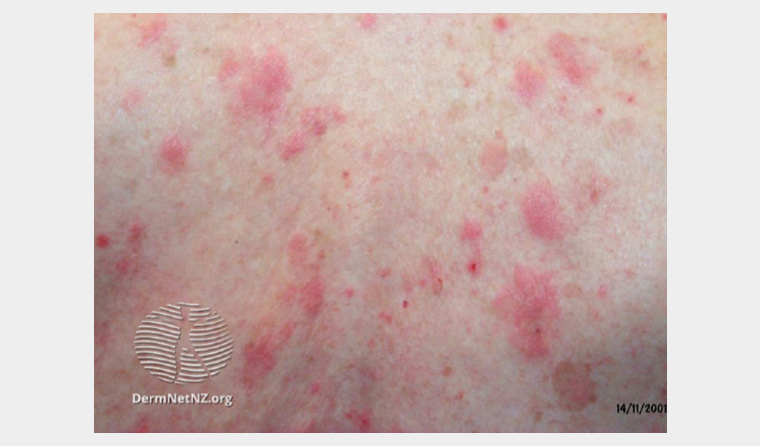
Figure 2. Bullous pemphigoid: eczematous and urticated plaques that might be followed by a bullous phase.
Reproduced from www.dermnetnz.org, with permission by ©DermNet, 2023.
Drug-associated bullous pemphigoid has been reported (Box 2).17 If the timeline is suggestive, the suspected medication should be ceased upon diagnosis. Dipeptidyl peptidase-4 inhibitors have increasingly been reported to induce bullous pemphigoid.18
| Box 2. Commonly prescribed medications associated with bullous pemphigoid17 |
Aspirin
Dipeptidyl peptidase 4 inhibitors
Frusemide
Enalapril
Ibuprofen
Hydrochlorothiazide
Rosuvastatin
Sulfasalazine
Programmed cell death protein 1 (PD-1) inhibitors |
A skin biopsy is recommended in diagnosing bullous pemphigoid. Two punch biopsy samples are recommended:
- a biopsy taken from the edge of the blister (if present) and sent in formalin for histopathology
- a biopsy from an area of uninvolved skin adjacent to the blister/plaque, sent in saline-soaked gauze for direct immunofluorescence staining.
Bullous pemphigoid is often associated with comorbidities (eg cardiovascular disease, dementia, stroke), along with advanced patient age, making management more challenging.16 In severe cases, intensive nursing care and hospitalisation might be required. Patients with bullous pemphigoid are best managed in conjunction with a dermatologist.
Conclusion
Red, scaly cutaneous eruptions in the older patient can be diagnosed with a thorough clinical assessment and appropriate use of investigations. Treatment is tailored to account for physical frailty, limitations in carer availability, comorbidities and risk of clinically significant medication interactions.
Key points
- Red, scaly rashes in the older patient have a wide differential diagnosis.
- A skin biopsy sent for histopathology and/or direct immunofluorescence is very useful if the diagnosis is unclear after clinical assessment.
- Management requires consideration of physical impairments, carer availability and cost.